Comprehensive Guide to Types of Arthritis and Effective Management Strategies
This comprehensive guide explores various forms of arthritis, including osteoarthritis, rheumatoid arthritis, psoriatic arthritis, and gout. It emphasizes early diagnosis, treatment options, lifestyle changes, and innovative therapies to manage symptoms effectively. Recognizing symptoms early and adopting a holistic approach can significantly enhance quality of life and joint health.
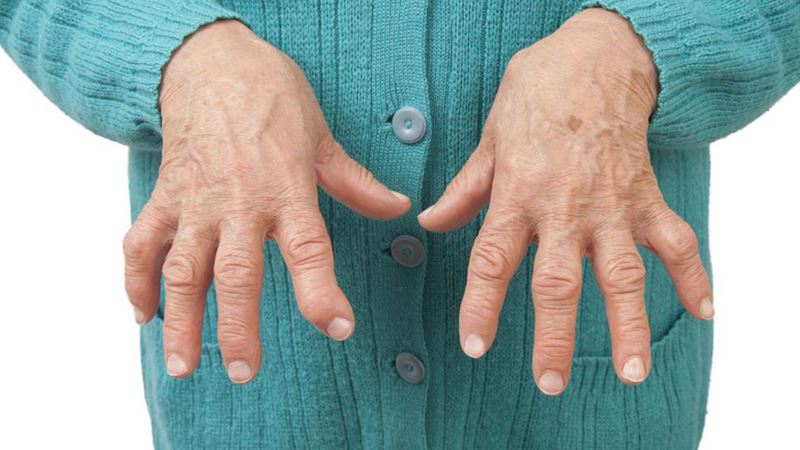
Arthritis is a prevalent condition characterized by inflammation and degeneration of joints, often leading to chronic pain and mobility issues. Although its onset can be gradual, the impact becomes more pronounced as the disease progresses, significantly affecting quality of life. Recognizing early symptoms and understanding various types of arthritis are crucial steps toward managing the condition effectively. This extensive guide provides detailed insights into the most common forms of arthritis, including osteoarthritis, rheumatoid arthritis, psoriatic arthritis, gout, and others. It also explores comprehensive treatment options, lifestyle modifications, and innovative therapies aimed at alleviating symptoms and improving joint function.
Arthritis commonly manifests through joint pain, stiffness, swelling, and decreased range of motion, especially after periods of inactivity or rest. Many individuals notice these symptoms first in the morning or after prolonged sitting. The severity and pattern of symptoms can vary depending on the specific type of arthritis and the joints involved. Often, both sides of the body are affected symmetrically, such as both knees or wrists, but certain types may target specific joints or areas. Recognizing these patterns helps in early diagnosis and tailored treatment planning.
- Osteoarthritis
Osteoarthritis (OA) is the most common form of arthritis, predominantly affecting older adults. It results from the deterioration of cartilage—the cushioning tissue between bones—leading to bone-on-bone contact, pain, and joint stiffness. As cartilage wears down over time, the body may attempt to repair itself by forming bone spurs, known as osteophytes, which can further restrict movement and cause discomfort. This condition most frequently impacts weight-bearing joints such as the knees, hips, and spine, as well as the hands. Factors like genetics, obesity, joint injuries, and repetitive stress accelerate its development.
- Rheumatoid Arthritis
Rheumatoid arthritis (RA) is an autoimmune disorder where the immune system mistakenly attacks the synovial membrane lining the joints, causing inflammation, swelling, and eventual joint damage. Unlike osteoarthritis, RA often presents symmetrically and can affect smaller joints such as those in the hands and feet. It's characterized by periods of flare-ups and remission, and if left untreated, it may lead to joint deformity and systemic complications including fatigue and fever. Early diagnosis and aggressive treatment can help control the disease progression and prevent irreversible joint damage.
- Psoriatic Arthritis
This form of arthritis is associated with psoriasis—a skin condition marked by scaly patches. Psoriatic arthritis involves inflammation of the joints and can affect any part of the body, leading to joint stiffness, pain, and swelling. It may also cause deformities if not managed properly. The disease varies greatly among individuals, with some experiencing mild symptoms while others develop severe joint damage. Managing psoriasis and arthritis simultaneously is key to controlling symptoms and preventing long-term complications.
- Gout
Gout is a painful form of arthritis caused by the accumulation of uric acid crystals in the joints, commonly affecting the big toe, knees, and ankles. Elevated uric acid levels in the blood can result from dietary factors, obesity, genetics, or certain medications. Gout attacks are episodic, characterized by sudden and intense pain, redness, and swelling. Chronic gout can lead to joint damage if not properly managed, emphasizing the importance of lifestyle modifications and medication to control uric acid levels.
Effective management of arthritis involves a combination of medical treatments, lifestyle changes, physical therapy, and sometimes surgical interventions. The goal is to reduce inflammation, alleviate pain, improve joint function, and enhance overall quality of life.
- Medical Treatment Options
Your healthcare provider might recommend medications such as non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroids, disease-modifying antirheumatic drugs (DMARDs), or biologics depending on the type and severity of arthritis. Pain relievers and anti-inflammatory drugs help control symptoms, but they should be used under medical supervision to avoid adverse effects.
Physical therapy plays a vital role in maintaining joint flexibility and muscle strength. Specific exercises tailored to your condition can reduce stiffness and improve mobility. Assistive devices like braces, splints, or orthotic inserts can provide support and reduce stress on affected joints.
Surgical options, including joint replacements or joint fusion, are considered when conservative treatments fail to relieve pain or restore function. Joint replacement surgery, particularly for hips and knees, can significantly improve life quality for patients suffering from advanced osteoarthritis.
- Lifestyle and Home Remedies
Adopting a healthy lifestyle is essential in managing arthritis. Maintaining a healthy weight reduces stress on weight-bearing joints, decreasing pain and slowing disease progression. Incorporating low-impact exercises such as swimming, cycling, or walking can enhance joint flexibility and overall fitness.
A balanced diet rich in anti-inflammatory foods—like fruits, vegetables, omega-3 fatty acids, and whole grains—can help reduce joint inflammation. Avoiding processed foods, excessive sugar, and alcohol is also beneficial.
Applying heat or cold therapy can provide temporary relief from joint pain and swelling. Hot packs or warm baths relax muscles and improve blood circulation, while cold packs reduce inflammation and numb the area to ease pain.
Stress management techniques, such as yoga, meditation, and mindfulness, may help reduce pain perception and improve mental well-being. Support groups and counseling services offer emotional support and practical advice for managing the challenges of arthritis.
- Emerging Therapies and Future Directions
Advances in medical research are paving the way for innovative treatment options. Regenerative medicine, including stem cell therapy and platelet-rich plasma (PRP) injections, shows promise in repairing damaged cartilage and tissues.
The development of targeted biologic drugs allows for more precise suppression of inflammatory processes in autoimmune forms of arthritis, minimizing side effects associated with traditional therapies. Personalized medicine approaches aim to tailor treatment plans based on genetic, environmental, and lifestyle factors.
Clinical trials continue to explore the efficacy of new medications, minimally invasive surgical procedures, and technological devices designed to improve joint health and functionality. Early diagnosis, combined with these evolving treatments, offers hope for better management and enhanced quality of life for arthritis sufferers.
In conclusion, understanding the different types of arthritis and their unique characteristics is essential for effective management. With a combination of medical intervention, lifestyle modifications, and emerging therapies, individuals can lead active, pain-free lives despite their condition.
