Understanding Trigger Finger: Types, Causes, and Prevention Strategies
Discover comprehensive insights into trigger finger, including its types, causes, symptoms, and effective prevention strategies. Learn how conditions like inflammation, systemic diseases, and repetitive motions contribute to this common hand issue. Expert tips on exercises, management, and when to seek medical intervention can help maintain finger mobility and reduce discomfort for both adults and children. Prevent trigger finger through proper care practices, early diagnosis, and understanding underlying health risks.
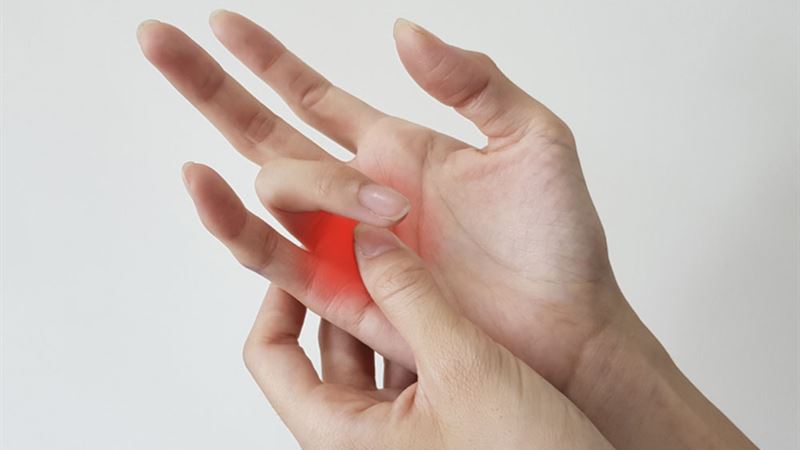
Overview of Trigger Finger in Adults and Children
Trigger finger, also known as stenosing tenosynovitis, is a condition affecting the fingers and thumb, characterized by catching, locking, or stiffness when moving the affected digit. It occurs due to inflammation or thickening of the sheath surrounding the flexor tendons, which impedes smooth finger movement. Although commonly seen in adults, especially those over 40, trigger finger can also present in children, often involving the thumbs. Understanding the different types, underlying causes, and preventive measures can help manage and reduce its impact on daily life.
Types of Trigger Finger
Trigger finger manifests primarily in two forms: primary and secondary. Each type has distinct underlying mechanisms and implications.
- Primary Trigger Finger
This form results directly from localized inflammation and thickening of the tendon sheath without an identifiable systemic condition. The inflammation causes the sheath to become constricted, making it difficult for the tendon to glide smoothly during finger movement. As a consequence, the finger may lock or trap in a bent position, particularly during flexion and extension. This type usually develops gradually and is often associated with repetitive finger motions, such as typing or manual labor. - Secondary Trigger Finger
Unlike primary trigger finger, this variant occurs secondary to underlying health issues that influence the tendons and their sheaths. Conditions like diabetes, rheumatoid arthritis, gout, and psoriatic arthritis can lead to systemic inflammation, promoting tendon sheath thickening and adhesions. Over time, these systemic diseases exacerbate the likelihood of trigger finger episodes, often affecting multiple fingers or both hands.
Why Does Trigger Finger Occur?
To comprehend trigger finger causation, it's essential to understand the anatomy of the finger's internal structures. A number of tendons, muscles, and bones work in harmony to facilitate finger movements. Tendons connecting the muscle in the forearm to the finger bones pass through protective sheaths that enable smooth gliding. During finger flexion, tendons contract and slide through these sheaths. Normally, this process is seamless; however, in trigger finger, the tendons or their sheaths become inflamed or thickened, leading to friction and obstruction.
When the tendons cannot glide smoothly, they may catch at the entrance of the sheath, causing the finger to remain in a bent or flexed position despite attempts to extend it. Often, a palpable lump, known as a nodule, forms along the tendon, contributing to the locking mechanism. Commonly, individuals notice stiffness and pain in the mornings, with symptoms worsening after repetitive use or prolonged inactivity.
Several factors can contribute to trigger finger development, although pinpointing an exact cause is often challenging. Some prevalent explanations include:
- Prolonged or repetitive use of fingers, leading to strain and micro-injury to tendons and muscles.
- Inflammation due to infections or autoimmune responses that increase the volume of the tendon sheath.
- Repeated friction or overuse causing the formation of nodules or lumps on tendons.
- Age-related degeneration, as the tendons lose elasticity and strength over time.
- Genetic predispositions, which might influence connective tissue resilience.
Causes of Bilateral and Multiple Trigger Fingers
When trigger finger affects both hands, it is referred to as bilateral trigger finger. Such cases often involve systemic factors like amyloidosis, a condition characterized by abnormal protein depositions. Multiple trigger finger occurrence, affecting several fingers simultaneously, can be caused by common factors such as repetitive strain, underlying systemic conditions, or injury. In these situations, it's essential to seek medical advice for comprehensive diagnosis and targeted treatment.
- Repetitive manual activities and overuse of fingers.
- Underlying health issues such as diabetes or rheumatoid arthritis.
- Recent or past hand injuries.
- Advancing age and genetic factors.
- Protein deposits associated with amyloidosis.
Trigger Finger in Pediatric Patients
Children are particularly susceptible to trigger finger affecting the thumbs, especially between ages one and four. Pediatric trigger finger may arise from congenital abnormalities or trauma. In many cases, the condition may resolve naturally or with conservative treatments, but some instances might necessitate surgical intervention if the finger becomes rigid and cannot extend accurately. Symptoms in children can vary from mild stiffness to complete locking, and the presence or absence of pain depends on the severity and inflammation level. Close observation and prompt treatment are vital to prevent long-term mobility issues.
Strategies to Mitigate Trigger Finger Symptoms
While the complete prevention of trigger finger can be difficult due to various inherent and environmental factors, several practical approaches can minimize its occurrence and severity:
- Avoid Overusing Fingers
Excessive use, especially in repetitive tasks like typing, gaming, or manual craftsmanship, can put undue stress on tendons. Taking regular breaks, using ergonomic tools, and practicing proper techniques are essential. Engaging in hand and finger strengthening exercises can also improve flexibility and resilience. - Perform Regular Hand and Finger Exercises
Regular movements help maintain tendon and joint health. Exercises such as squeezing stress balls, finger stretches, or web stretches can bolster muscle strength and prevent stiffness. Incorporating gentle stretching routines during work breaks can significantly reduce the risk. - Manage Underlying Conditions
Controlling systemic conditions like diabetes, rheumatoid arthritis, and hypothyroidism reduces the inflammatory burden on tendons, decreasing trigger finger risk. Follow prescribed medication plans and maintain a healthy lifestyle. - Apply Rest and Cold Therapy
Resting the affected hand and applying ice packs when inflammation or pain is present can decrease swelling and relieve symptoms. Proper rest allows tissues to recover and prevents further strain. - Professional Treatment and Interventions
If symptoms persist, consulting a healthcare provider for options like corticosteroid injections, splinting, or surgical release may be necessary. Early intervention can prevent permanent damage and restore normal finger movement.
Final Takeaway
Although trigger finger has no singular known cause, factors such as repetitive movements, age-related degeneration, and associated health issues contribute significantly to its development. Preventative measures like targeted exercises, proper rest, and managing systemic health conditions can reduce its severity and frequency. Recognizing early symptoms and seeking prompt care ensures better outcomes and maintains hand functionality.
