Comprehensive Guide to Different Types of Diabetes and Their Management
This comprehensive article explores the three main types of diabetes—Type 1, Type 2, and gestational diabetes—detailing their causes, symptoms, diagnosis, and management strategies. It emphasizes the importance of lifestyle choices, regular monitoring, and medical treatment in controlling blood sugar levels and preventing complications. With ongoing research, a future cure remains promising. Educating oneself about these conditions can empower patients and caregivers to make informed decisions for healthier living and better diabetes management.
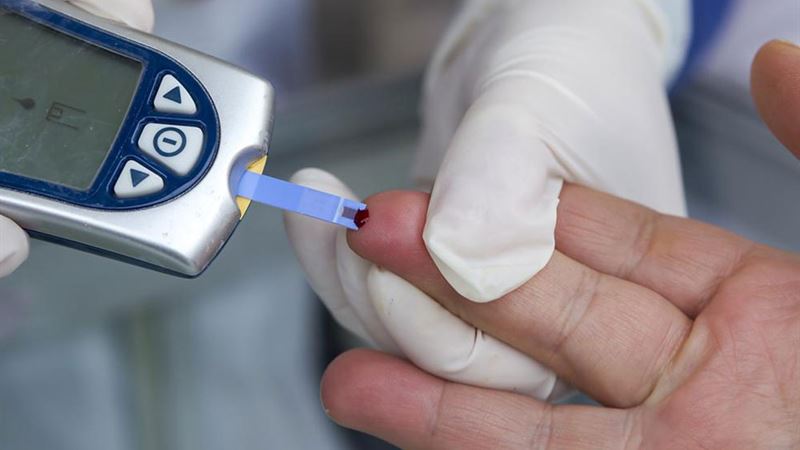
Understanding the Types of Diabetes
Type 1 Diabetes: A condition that typically develops during childhood or adolescence, although it can also occur in adults, Type 1 diabetes is an autoimmune disorder where the body's immune system mistakenly targets the insulin-producing cells in the pancreas. This leads to a significant deficiency of insulin, the hormone responsible for regulating blood sugar levels.
When the pancreas fails to produce sufficient insulin, glucose cannot enter the body's cells to be used for energy. As a consequence, blood glucose levels rise, leading to hyperglycemia. Patients with Type 1 diabetes often experience symptoms such as frequent urination, excessive thirst, unexplained weight loss, fatigue, and blurred vision. Managing this condition requires lifelong insulin therapy, along with meticulous blood sugar monitoring and lifestyle adjustments like diet and exercise.
A particular form of adult-onset autoimmune diabetes, known as Latent Autoimmune Diabetes in Adults (LADA), shares features with Type 1 diabetes and necessitates similar management strategies. Both conditions entail the immune system attacking pancreatic beta cells, resulting in insufficient insulin production.
Approximately 10% of all diabetes cases are classified as Type 1. Though not preventable, early diagnosis and effective treatment can significantly improve quality of life and prevent complications.
Type 2 Diabetes: The most common form of diabetes, accounting for around 90% of cases worldwide, Type 2 diabetes generally manifests in adulthood but is increasingly diagnosed in children and teenagers. It results from the body's inability to effectively use insulin—a condition known as insulin resistance—coupled with an eventual decline in insulin production.
When cells become less responsive to insulin, glucose remains in the bloodstream instead of entering cells to generate energy. Over time, persistent high blood sugar can damage blood vessels and organs, increasing the risk of heart disease, nerve damage, kidney failure, and vision problems.
Genetics, obesity, sedentary lifestyles, poor dietary choices, and certain medical conditions can predispose individuals to Type 2 diabetes. Symptoms include increased thirst and hunger, frequent urination, fatigue, slow healing wounds, and recurrent infections. The management of Type 2 diabetes involves a combination of lifestyle modifications such as regular physical activity and diet regulation, oral medications that improve insulin sensitivity or secretion, and sometimes insulin therapy.
Early intervention and consistent control of blood sugar levels can significantly reduce the risk of complications associated with this disease.
Gestational Diabetes: A temporary condition that arises during pregnancy, gestational diabetes affects about 2% to 4% of pregnant women. This form of diabetes occurs when hormonal changes during pregnancy cause insulin resistance, leading to elevated blood sugar levels. Although it is usually resolved after childbirth, it poses health risks to both mother and baby if not managed properly.
Women with gestational diabetes face a higher likelihood of developing Type 2 diabetes later in life. Additionally, the condition increases the risk of complications during delivery, such as preeclampsia and macrosomia (large baby). Babies born to mothers with gestational diabetes may experience hypoglycemia and increasing risk of obesity or Type 2 diabetes in the future.
Diagnosis is typically made through glucose screening tests during pregnancy. Management involves maintaining a healthy diet, engaging in regular physical activity, and monitoring blood glucose levels closely. In some cases, insulin injections or medications may be necessary to keep blood sugar within safe ranges, especially if dietary changes alone are insufficient.
The quest for a permanent cure for diabetes remains a major focus in modern medical research. While scientists continue to explore regenerative therapies, immune modulation, and advanced medication options, current management strategies emphasize lifestyle interventions and medication adherence. Patients are encouraged to follow a disciplined routine involving balanced nutrition, regular exercise, and routine health check-ups.
In summary, understanding the different types of diabetes and their unique characteristics is essential for effective management and prevention. With ongoing research and innovation, hope remains high for future breakthroughs that could offer a cure or more advanced treatment options for this widespread condition.
