Understanding Medical Conditions That Contribute to Osteoporosis-Related Bone Erosion
Discover how various medical conditions like autoimmune diseases, diabetes, asthma, and thyroid disorders can accelerate osteoporosis-related bone loss. Learn about risk factors, symptoms, and preventive strategies to protect your bone health effectively through early diagnosis and tailored treatments.
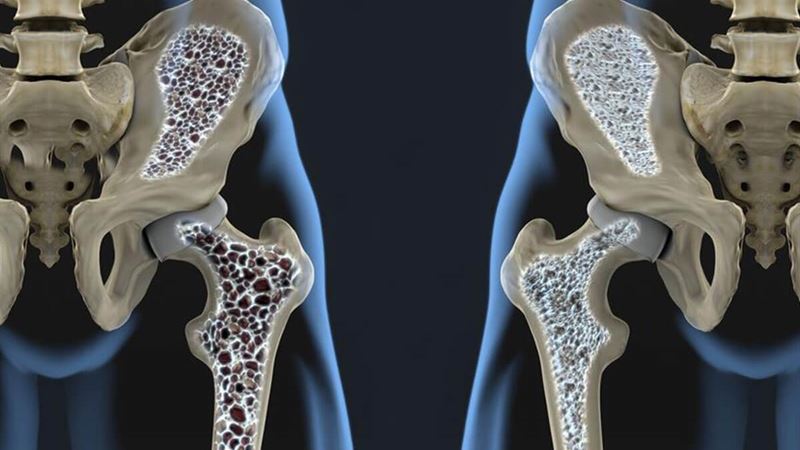
Understanding the risk factors for osteoporosis is vital for prevention and management. Factors such as genetic predisposition, body frame size, advancing age, sex, racial background, sedentary lifestyle, and certain eating disorders can influence bone health. For example, women, particularly after menopause, are at higher risk due to hormonal changes affecting bone density. Lifestyle modifications, medications, and dietary interventions form the cornerstone of management strategies, tailored to individual risk profiles in order to prevent fractures and maintain bone strength.
While the causes of osteoporosis are multifactorial, certain medical conditions play a significant role in accelerating bone loss either directly or through the side effects of treatments. Recognizing these conditions is essential for early intervention. Some of the most notable diseases linked with osteoporosis include autoimmune disorders, metabolic conditions, respiratory illnesses, and thyroid dysfunctions. Below, we explore the most common health issues associated with increased osteoporosis risk and delve into how they contribute to bone degradation.
- Rheumatoid Arthritis and Systemic Lupus Erythematosus
Rheumatoid arthritis (RA) and lupus are autoimmune diseases where the immune system mistakenly targets its own tissues. Both conditions can significantly impact bone density over time. An estimated three million Americans live with either RA or lupus. Lupus predominantly affects women aged 15 to 45, the critical years for bone development and accumulation. Dr. Beatrice Edwards, a renowned expert at Northwestern University’s Bone Health Center, emphasizes, “Anything that hampers bone growth during these formative years significantly raises the risk of osteoporosis later in life.” The chronic inflammation and long-term use of corticosteroids necessary for managing these conditions contribute to accelerated bone loss, making osteoporosis a common complication in affected individuals.
- Diabetes Mellitus
The relationship between diabetes and osteoporosis is complex and still being studied. Researchers notice that patients with type 1 diabetes tend to have lower bone mineral density. Dr. Edwards suggests that elevated blood sugar levels may inhibit bone formation, similar to the effects seen with steroid use. Since type 1 diabetes usually manifests during childhood or adolescence — the key period for attaining peak bone mass — these individuals may never reach optimal bone density levels. This deficit predisposes them to increased fragility and fracture risk in later years, highlighting the importance of vigilant osteoporosis screening and management in diabetic patients.
- Asthma and Respiratory Conditions
While asthma itself does not directly cause osteoporosis, the medications used to treat it—especially corticosteroids—are a significant contributing factor. Around 20 million Americans suffer from asthma, and long-term use of corticosteroids can diminish bone formation and increase resorption, leading to weakened bones. These medications effectively control symptoms but pose a risk for osteoporosis with prolonged use. Patients using corticosteroids for asthma or other respiratory illnesses should be aware of this side effect and discuss preventive strategies with their healthcare providers.
- Hyperthyroidism
Overactivity of the thyroid gland results in excess thyroid hormone production, a condition known as hyperthyroidism. Dr. Edwards explains, “Elevated thyroid hormone accelerates bone remodeling cycles, and after age 30, these cycles become inefficient, resulting in net bone loss.” Excess thyroid hormone stimulates increased bone turnover, which, without sufficient new bone formation, leads to decreased bone density over time. Managing hyperthyroidism effectively and monitoring bone health are crucial to preventing osteoporosis in affected individuals.
- Other Contributing Conditions
Additional medical issues linked with osteoporosis include Multiple Sclerosis (MS) and celiac disease. MS, characterized by nerve and muscle impairment, often results in decreased physical activity and secondary bone demineralization. Celiac disease causes malabsorption of nutrients essential for bone health, such as calcium and vitamin D, leading to osteoporosis risk. Recognizing these associations allows for comprehensive management strategies that encompass disease control and bone preservation. Proactive measures like supplementation, lifestyle adjustments, and regular bone density assessments can mitigate osteoporosis progression in these populations.
