Understanding the Similarities and Differences Between Rheumatoid Arthritis and Lupus
This detailed article explores the complex similarities and key differences between rheumatoid arthritis and lupus. It highlights symptoms, diagnostic challenges, and treatment strategies, emphasizing the importance of early detection. Understanding these autoimmune conditions helps patients and healthcare professionals better manage their health and prevent long-term complications. With ongoing research, future therapies may offer even more precise and effective management options for these chronic diseases, improving patient outcomes and quality of life.
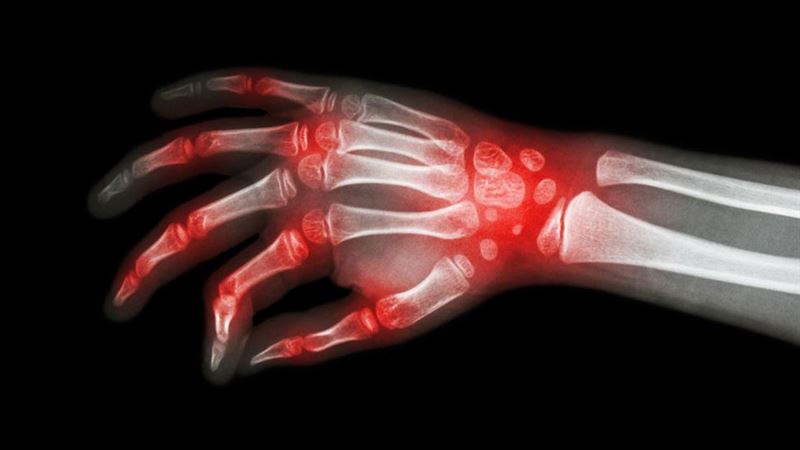
In many cases, patients suffering from either rheumatoid arthritis or lupus report joint discomfort that may be mistaken for other forms of arthritis or inflammatory diseases. The joints affected by these conditions tend to become warm, tender, and swollen, but the degree varies. Rheumatoid arthritis tends to cause more prominent joint deformities, with erosions visible on imaging studies over time, while lupus seldom produces significant bone erosion. This distinction is crucial for clinicians and helps guide appropriate treatment strategies.
Fatigue and general weakness are hallmark symptoms seen in both diseases, often signifying active disease. Patients may experience flares characterized by increased joint pain, fever, and a temporary worsening of overall health status. Recognizing these patterns aids healthcare providers in differentiating between the two. Moreover, both conditions are seen more frequently in women, especially those of reproductive age, though men can also be affected. The hormonal and genetic factors contributing to this gender disparity are subjects of ongoing research.
One of the primary challenges in managing rheumatoid arthritis and lupus is their chronic nature, requiring long-term treatment plans to minimize complications and improve quality of life. Without proper management, RA can lead to joint destruction and deformities, severely impairing mobility. In lupus, organ damage such as kidney failure or cardiovascular issues can occur if the disease remains uncontrolled. Early and accurate diagnosis is vital to initiate appropriate therapy and prevent irreversible damage.
Both diseases involve complex immune dysregulation, necessitating personalized treatment approaches. Disease-modifying anti-rheumatic drugs (DMARDs) are standard for managing RA, aiming to slow joint damage and reduce inflammation. In lupus, immunosuppressive medications, corticosteroids, and antimalarial drugs like hydroxychloroquine are employed to control systemic inflammation and prevent organ damage. Regular monitoring and adjustments are crucial, as each patient’s disease course varies significantly.
