Effective Strategies to Monitor and Manage Your Blood Glucose Levels
This comprehensive guide discusses effective methods to monitor and control blood sugar levels in diabetics. It covers insulin management, tracking techniques, interpreting results, lifestyle strategies, and prevention of long-term complications. Regular blood glucose checking, understanding readings, and maintaining a balanced diet are emphasized as essential components of optimal diabetes care. Incorporating modern technology like continuous glucose monitors and adopting healthy habits can significantly improve blood sugar stability, enhance quality of life, and prevent serious health issues associated with diabetes. Stay informed and proactive in your diabetes management.
Understanding the Role of Synthetic Insulin
Proper blood sugar regulation is a vital component in managing diabetes and preventing serious health complications. Elevated blood glucose levels, if left uncontrolled, can lead to a range of health issues, including damage to blood vessels, nerve damage, and increased risk of cardiovascular diseases. One of the cornerstone treatments for managing diabetes is the administration of synthetic insulin. This hormone helps to regulate blood sugar by facilitating the uptake of glucose into cells, thereby reducing hyperglycemia. Although the body naturally produces insulin, many individuals with diabetes rely on insulin injections to compensate for insufficient production or ineffective functioning of their endogenous insulin. Regular insulin injections, prescribed by healthcare professionals, work to maintain blood glucose within a safe range, preventing dangerous spikes and dips. Understanding how synthetic insulin functions and adhering to the prescribed dosage is crucial for effective blood sugar management.
Monitoring Your Blood Sugar: The First Step
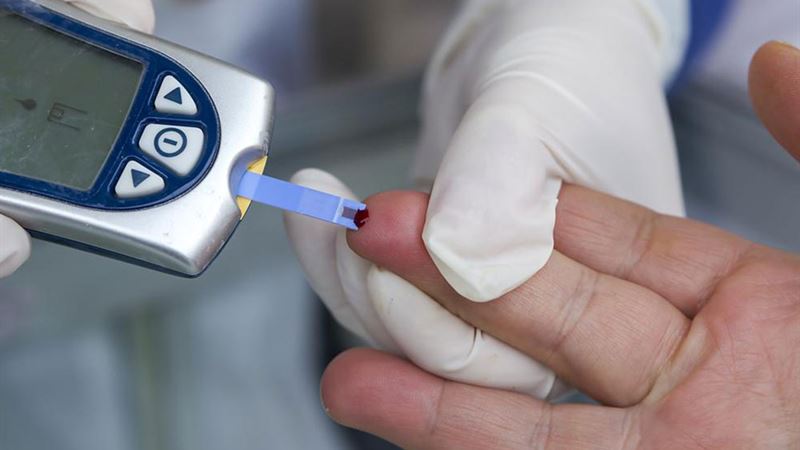
Consistent monitoring of blood glucose levels is essential for anyone managing diabetes. It allows for real-time insights into how your body responds to insulin therapy, diet, and lifestyle changes. The most common method for monitoring blood sugar involves using a glucose meter, a portable device that provides quick and accurate readings. To obtain reliable results, it’s advisable to check your blood sugar levels at specific times during the day, especially when fasting in the morning before breakfast. Fasting blood sugar measurements provide a baseline to assess whether your blood glucose is controlled during the overnight fast. To monitor your progress accurately, record each reading meticulously in a log. This log enables you and your healthcare provider to analyze patterns over time, helping to tailor your treatment plan effectively. It’s also recommended to check your blood sugar post-meal, particularly after breakfast, lunch, and dinner, to understand how different foods impact your glucose levels. Combining these readings offers a comprehensive picture of your diabetes control.
Interpreting Blood Sugar Results Effectively
Understanding what your blood sugar levels mean is pivotal for proper management. Normal fasting blood sugar levels typically range from 70 to 99 mg/dL, while post-meal levels should generally stay below 140 mg/dL. Readings significantly higher than these indicate hyperglycemia, which requires prompt adjustments either in insulin dosage or lifestyle. A blood glucose level exceeding 200 mg/dL consistently suggests poor control and possibly the need for medical intervention. Conversely, levels below 70 mg/dL may point to hypoglycemia, which can be life-threatening if untreated. Regular use of a blood sugar meter allows you to stay within safe limits and helps prevent the development of complications. Fluctuations outside the normal range signal that your current treatment plan may need revision. It’s essential to work closely with your healthcare provider, who can help interpret your results and adjust your insulin doses accordingly. Remember, maintaining stable blood glucose levels is the key to preventing long-term health issues associated with diabetes.
Strategies for Effective Blood Glucose Management
Achieving optimal blood sugar control involves a multifaceted approach that includes dietary management, regular physical activity, and medication adherence. First and foremost, diet plays a crucial role. Patients should focus on a balanced diet rich in fiber, lean proteins, healthy fats, and low in refined sugars and processed foods. Monitoring carbohydrate intake and choosing complex carbs over simple sugars can significantly stabilize blood glucose levels. Additionally, regular exercise helps improve insulin sensitivity and promotes glucose uptake by muscles. Engaging in at least 150 minutes of moderate-intensity activity weekly is generally recommended. Moreover, adhering strictly to your prescribed insulin regimen and other medications is vital. Regular follow-up appointments with your healthcare provider ensure that your treatment plan remains effective and allows for timely adjustments. Lifestyle modifications, such as stress management and ensuring adequate sleep, also contribute to better blood sugar control. By integrating these strategies into your daily routine, you can maintain more consistent blood glucose levels and reduce the risk of complications.
Preventing Complications through Consistent Monitoring
Long-term complications of unmanaged diabetes include kidney disease, nerve damage, vision problems, and cardiovascular issues. The key to avoiding these serious outcomes is consistent monitoring and management of blood sugar. Continuous glucose monitoring (CGM) devices offer a more advanced alternative to traditional finger-prick tests, providing real-time data and trends. This technology enables proactive adjustments, reducing guesswork and better preventing dangerous highs and lows. In addition to technological solutions, lifestyle choices such as maintaining a healthy weight, avoiding tobacco, limiting alcohol, and controlling blood pressure are vital. If your blood glucose readings are consistently out of range, consult your healthcare provider promptly to refine your management plan. Educating yourself about the signs and symptoms of hyperglycemia and hypoglycemia will empower you to act swiftly and seek medical attention if needed. Ultimately, adherence to your personalized diabetes management plan fosters long-term health, improved quality of life, and reduced risk of complications.
