Comprehensive Insights into Fibromyalgia: Symptoms, Diagnosis, and Treatment Approaches
Fibromyalgia is a complex disorder characterized by chronic widespread pain, fatigue, and sleep disturbances. This comprehensive article explores its symptoms, diagnostic criteria, and various treatment options, emphasizing a multidisciplinary approach to management. While no cure exists, personalized therapies combining medication, exercise, and holistic practices can greatly improve quality of life. Understanding fibromyalgia deeply enables patients and healthcare providers to develop effective strategies for symptom relief and emotional well-being, helping individuals manage this condition more successfully.
Understanding Fibromyalgia and Its Manifestations
Fibromyalgia is a complex chronic disorder characterized primarily by widespread musculoskeletal pain, alongside a host of other symptoms that can significantly impair an individual's quality of life. Recognizing this condition involves understanding its diverse symptoms, diagnostic processes, and available management options. Although the precise cause remains unclear, the syndrome's effects are profound, affecting not only physical health but also emotional well-being. This detailed guide aims to shed light on the various facets of fibromyalgia, from its clinical presentation to the latest approaches in diagnosis and comprehensive management strategies.
Core Symptoms of Fibromyalgia
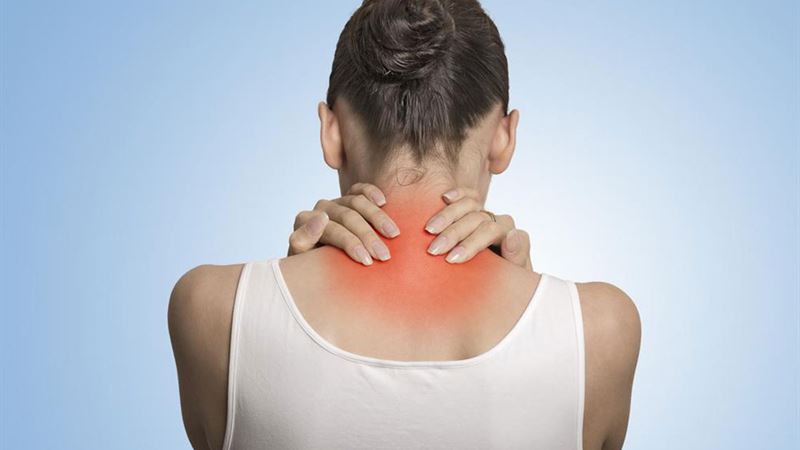
The hallmark of fibromyalgia is persistent, widespread musculoskeletal pain that does not originate from a clear injury or inflammation. Patients often describe this pain as a deep ache that pervades the entire body, frequently accompanied by profound fatigue. Even after extended rest or adequate sleep, individuals report feeling exhausted, which often leads to a vicious cycle of worsening fatigue and pain. Specific tender points, located on areas such as the neck, shoulders, chest, hips, or knees, are painfully sensitive upon touch, serving as important clues during diagnosis. Sleep disturbances are common, with patients experiencing non-restorative sleep or frequent awakenings due to discomfort or mood swings. Depression and anxiety frequently occur alongside fibromyalgia, further complicating the clinical picture.
Muscular symptoms associated with fibromyalgia go beyond pain. Patients may experience sensations of muscle pulling, burning, twitching, or stabbing pains—symptoms that mimic muscle overuse despite minimal physical activity. There can also be a persistent feeling of achiness targeting the back, shoulders, neck, joints, and hips, which often hampers daily activities like exercise or even simple movements. These symptoms contribute to a reduced quality of life and can escalate emotional distress.
Besides musculoskeletal discomfort, fibromyalgia manifests through various other signs that, although common in other conditions, may indicate the presence of this syndrome. These include dry eyes, mouth, and nasal passages; persistent abdominal pain; tingling or numbness in extremities; abnormal responses to temperature changes; recurrent headaches; urinary incontinence; irritable bowel syndrome; natural cognitive impairments often described as "fibro fog"—a state of mental sluggishness or forgetfulness; and general bodily stiffness. Recognizing these overlapping symptoms is vital for clinicians to differentiate fibromyalgia from other prevalent disorders.
The clinical features of fibromyalgia share commonalities with tendinitis, osteoarthritis, and bursitis—conditions often grouped under arthritis-related disorders by experts. Unlike localized pain seen in tendinitis or bursitis, fibromyalgia exhibits widespread, non-specific pain and stiffness affecting multiple regions simultaneously, often with fluctuating intensity.
Diagnostic Procedures for Fibromyalgia
Accurate diagnosis of fibromyalgia requires a comprehensive physical examination, detailed medical history, and a series of laboratory tests to exclude other potential causes. Due to the absence of definitive laboratory markers, physicians rely on established clinical criteria for diagnosis. An initial step involves ruling out treatable or more serious illnesses that share similar symptoms.
Blood tests are integral to the diagnostic process. A complete blood count (CBC) assesses for anemia or other blood disorders, while blood chemistry panels evaluate enzyme levels, nutrients, and calcium status. Since hypothyroidism can mimic fibromyalgia symptoms like fatigue and muscle aches, thyroid function tests are routinely performed. Additional laboratory investigations include measuring rheumatoid factor (RF) to rule out rheumatoid arthritis, Lyme disease titers to exclude Lyme disease, erythrocyte sedimentation rate (ESR) for inflammatory markers, antinuclear antibodies (ANA) for autoimmune conditions, and vitamin D levels due to widespread deficiencies linked to musculoskeletal pain.
The American College of Rheumatology has established specific criteria to diagnose fibromyalgia, emphasizing persistent, widespread pain lasting at least three months. This pain must persist on both sides of the body, include the axial skeleton (neck, back, chest), and involve specific tender points. Moreover, clinicians assess associated symptoms such as sleep disturbances, mood disorders, and fatigue to understand the syndrome's impact on the patient’s overall functioning. These evaluations help determine the severity and guide personalized management plans.
Strategies for Managing Fibromyalgia
Currently, there is no known cure for fibromyalgia. Treatments are aimed at alleviating symptoms and improving quality of life through a multidisciplinary approach. Management often involves combining pharmacological therapies, physical exercise, behavioral techniques, and alternative medicine to create a comprehensive care plan tailored to each individual’s needs.
Pharmacological options primarily focus on symptom relief. While no medications can eliminate fibromyalgia, several drugs have been approved by the FDA to reduce pain and improve function. These include:
- **Cymbalta** (Duloxetine): A serotonin-norepinephrine reuptake inhibitor that modulates pain perception and mood.
- **Lyrica** (Pregabalin): An anticonvulsant that targets nerve hyperexcitability, effective in reducing neuropathic pain associated with fibromyalgia.
- **Savella** (Milnacipran): An SNRI specifically approved for fibromyalgia, helping to manage pain and fatigue.
Non-opioid pain relievers are generally preferred to avoid dependency issues. Opioids are typically avoided unless under strict medical supervision, as they pose risks of long-term dependency and other adverse effects. Patients are advised to consult healthcare professionals before initiating any medication regimen, ensuring treatments are tailored to their individual health profiles.
Beyond medication, physical therapy and exercise play vital roles. A structured program emphasizing low-impact aerobic activities such as walking, swimming, or cycling can boost endurance, improve sleep, and reduce pain. Incorporating flexibility and strength training exercises helps maintain muscle function and reduce stiffness. Behavioral therapies, including cognitive-behavioral therapy (CBT), can aid in managing mood disturbances, enhance coping strategies, and mitigate the psychological burden of living with a chronic condition.
Complementary therapies, such as acupuncture, massage, yoga, and mindfulness meditation, have shown promising results in alleviating symptoms. These approaches help reduce stress, improve sleep quality, and promote an overall sense of well-being. An integrative treatment approach combining conventional and alternative methods can significantly improve patient outcomes.
Ongoing research aims to develop newer, targeted therapies, and improve understanding related to nerve signaling, brain processing, and the underlying pathology of fibromyalgia. Patients should maintain regular follow-up appointments to adjust treatment plans as needed, monitor symptom progression, and address any emerging issues.
Ultimately, managing fibromyalgia requires a sustained, patient-centered approach emphasizing education, lifestyle modifications, and a team-based healthcare strategy. With appropriate support and treatment, individuals can lead productive and fulfilling lives despite the challenges posed by this syndrome.
