Comprehensive Guide to Rheumatoid Arthritis and Lupus: Symptoms, Causes, and Management
This detailed guide provides an in-depth understanding of rheumatoid arthritis and lupus, covering symptoms, diagnosis, treatment options, and lifestyle tips. Early detection and personalized management are key to living well with these autoimmune conditions. Learn how to recognize early signs, adopt effective therapies, and improve your quality of life through informed decisions and supportive care.
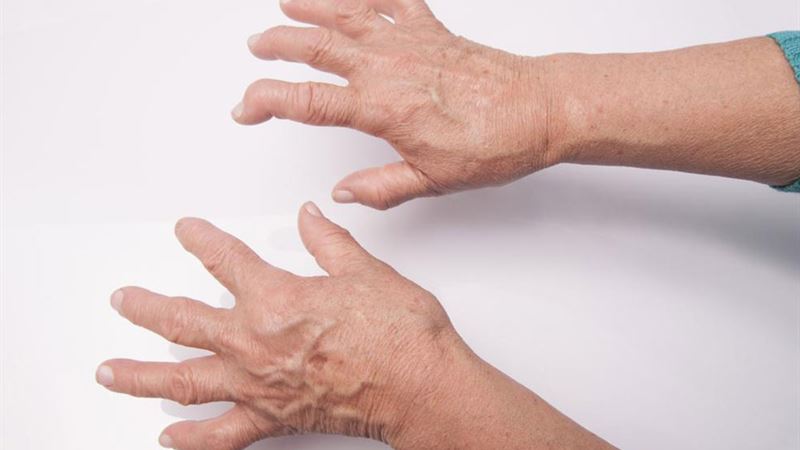
Imagine living with chronic conditions that can affect your entire body—from your skin and joints to your vital organs like the heart, lungs, kidneys, and brain. Rheumatoid arthritis and lupus are systemic autoimmune diseases that pose significant health challenges and require proper understanding and management. They are often misunderstood, yet awareness is crucial for early diagnosis, effective treatment, and improving quality of life.
Both ailments can strike individuals of all ages, impacting children, teenagers, and adults alike. Despite extensive research, the precise causes remain elusive, but genetic predisposition, environmental factors, and immune system dysfunction are believed to play roles. Recognizing early signs and consulting healthcare professionals promptly can make a substantial difference in managing these autoimmune diseases effectively.
This comprehensive guide explores the key symptoms, underlying causes, and treatment options for rheumatoid arthritis and lupus. It emphasizes the importance of early diagnosis, lifestyle modifications, and supportive care to help those affected lead healthier, more fulfilling lives.
Understanding Rheumatoid Arthritis and Lupus
Rheumatoid arthritis (RA) is a chronic inflammatory disorder primarily affecting the joints, leading to pain, swelling, and potential deformities. Over time, RA can damage cartilage and bones, impairing joint function. It often impacts symmetric joints—meaning both sides of the body are affected equally—such as wrists, knees, and fingers.
Lupus, or systemic lupus erythematosus (SLE), is another complex autoimmune disease characterized by the immune system attacking the body's tissues. It can induce widespread inflammation affecting the skin, organs, joints, and blood. Lupus exhibits periods of flare-ups and remission, making its management particularly challenging.
Recognizing Early Symptoms of Rheumatoid Arthritis
- Persistent joint pain and tenderness, especially in the smaller joints
- Swelling and warmth in affected joints
- Joint stiffness, particularly noticeable in the mornings or after periods of inactivity
- Deformities or changes in joint shape over time
- Loss of joint mobility and function
- Feeling of fatigue, fever, and malaise
- Symmetrical joint involvement—affecting the same joints on both sides of the body
- Reduced grip strength or difficulty performing daily tasks
If you experience any of these symptoms persistently, seeking prompt medical evaluation is essential for early diagnosis and intervention.
Recognizing Early Symptoms of Lupus
- Unexplained and recurrent fevers
- Fatigue and weakness that doesn't improve with rest
- Unusual skin rashes, notably a butterfly-shaped rash across the cheeks and nose
- Joint pain, swelling, or tenderness, often involving the fingers, wrists, or knees
- Photosensitivity—skin reactions to sunlight
- Hair loss and scalp issues
- Involvement of organs such as kidneys and lungs, leading to symptoms like chest pain or shortness of breath
- Dry eyes and mouth
- Gastrointestinal disturbances and neurological symptoms
- Thyroid involvement and hormonal imbalances
Recognizing these early signs can help prevent severe complications, emphasizing the need for regular medical checkups and early intervention in suspected cases.
Diagnostic Approaches for Rheumatoid Arthritis and Lupus
Diagnosing these autoimmune diseases involves a combination of clinical evaluation, laboratory testing, and imaging studies. Rheumatoid factor (RF), anti-CCP antibodies, and elevated inflammatory markers like ESR and CRP are typical in RA. Lupus is often diagnosed based on criteria including ANA (antinuclear antibodies), anti-dsDNA, and anti-Smith antibodies, along with clinical features.
Imaging techniques like X-rays, ultrasounds, or MRIs can reveal joint damage or organ involvement. Early diagnosis is crucial to start appropriate treatment, prevent irreversible damage, and improve long-term outcomes.
Effective Treatment Strategies for Rheumatoid Arthritis and Lupus
Currently, these autoimmune conditions have no definitive cure. However, modern treatments aim to control symptoms, reduce inflammation, and prevent tissue damage, greatly enhancing patients' quality of life.
Medical Treatments: Disease-modifying antirheumatic drugs (DMARDs), biologics, corticosteroids, and immunosuppressants are the mainstay of therapy. Your healthcare provider will tailor treatments based on severity and individual response.
Lifestyle Modifications: Adapting daily routines can significantly reduce disease impact. Regular low-impact exercises such as swimming, walking, or cycling improve joint flexibility and mental health. Maintaining a healthy weight reduces stress on joints.
Diet and Nutrition: Consuming a balanced diet rich in anti-inflammatory foods—like fruits, vegetables, omega-3 fatty acids, and whole grains—can help manage symptoms. Avoiding smoking and excess alcohol is essential, as they can worsen disease activity and interfere with medications.
Sun Protection and Skin Care: For lupus patients, protecting the skin from sun exposure by using sunscreen, wearing protective clothing, and avoiding prolonged sun exposure are critical to prevent skin rashes and flares.
Psychological Support and Patient Education: Living with a chronic autoimmune disease can be emotionally taxing. Joining support groups, therapy, and patient education programs empower individuals to manage their conditions confidently.
Managing Daily Life and Preventing Complications
Effective disease management involves a holistic approach. Regular follow-ups with healthcare providers ensure the treatment plan is effective and adjustments are made as necessary. Patients should monitor their symptoms, keep track of flare-ups, and communicate openly about side effects.
Incorporating stress management techniques—such as meditation, yoga, or deep-breathing exercises—can help reduce disease exacerbations. Adequate rest, balanced activity, and avoiding overexertion are equally important.
Protecting oneself from infections through good hygiene and avoiding crowded places during flare-ups helps prevent additional health complications. It's important to have a personalized emergency plan for severe reactions or sudden worsening of symptoms.
The Role of Patient Support and Education
Support groups and patient advocacy organizations can provide emotional support and practical advice. Connecting with others sharing similar experiences fosters resilience and provides a platform to share coping strategies.
Education about disease processes, medication side effects, and lifestyle adaptations empowers patients, leading to better disease management and improved outcomes.
Future Directions and Research
Ongoing research aims to develop more targeted therapies with fewer side effects, improve early diagnostic techniques, and understand the precise causes of these complex diseases. Advances in personalized medicine may soon customize treatments based on genetic and molecular profiles, promising even better management options.
In summary, rheumatoid arthritis and lupus are significant autoimmune diseases that require awareness, early diagnosis, and comprehensive management strategies. Patients can lead fulfilling lives by adhering to treatment plans, making lifestyle adjustments, and staying informed about new developments in medical science.
