Comprehensive Guide to the Causes and Prevention of Impetigo in Children and Adults
Impietigo is a highly contagious bacterial skin infection affecting both children and adults. Common causes include direct contact, shared personal items, skin injuries, and environmental factors like humidity. Proper hygiene, early diagnosis, and medical treatments are key to managing and preventing impetigo. Recognizing early symptoms and seeking prompt medical care can help prevent complications such as ecthyma. This comprehensive guide provides insights into causes, risk factors, and effective treatment strategies to ensure quick recovery and prevent spreading of this contagious condition.
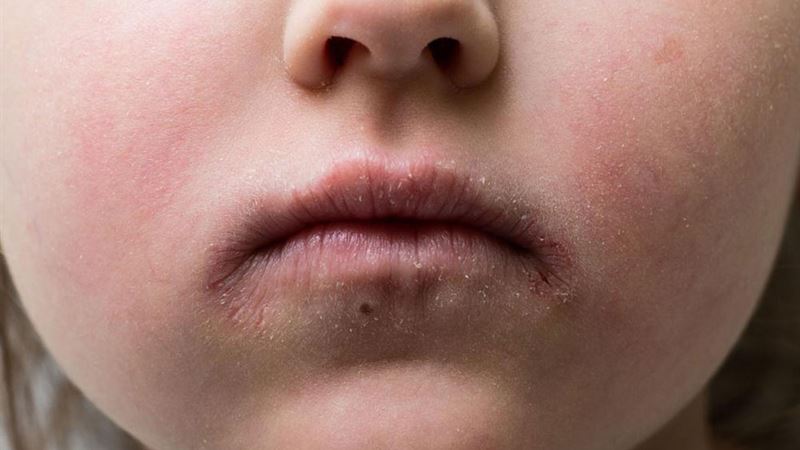
- Exposure to bacteria through direct contact with an infected individual.
- Sharing personal items such as towels, clothing, or toys that have been contaminated.
- Compromised skin, such as cuts, scrapes, or insect bites, serving as entry points for bacteria.
- Insect bites or bites from animals can also introduce bacteria, leading to infection.
How do adults develop impetigo?
While impetigo is most common among young children, it can occasionally affect teenagers and adults. Factors contributing to adult cases include:
- Poor personal hygiene practices
- Pre-existing health conditions like diabetes mellitus
- Weak immune system responses
- High exposure environments such as crowded places, public transport, workplaces, or communal living spaces
- Humid and warm climates, which foster bacterial growth, increase the risk of impetigo development.
Effective management and prevention strategies for impetigo
If you notice symptoms of impetigo in yourself or your child, prompt consultation with a healthcare professional such as a dermatologist or pediatrician is essential. In situations where immediate medical help isn't accessible, utilizing online resources like impetigo images can assist with initial assessments, especially during travel or in remote areas lacking comprehensive healthcare infrastructure. However, diagnosing and treating impetigo should always be performed under medical supervision; self-medicating without professional guidance can worsen the condition.
To confirm the diagnosis or assess the severity, sharing clear photographs with your healthcare provider via phone or email can be advantageous. Such images enable physicians to evaluate whether topical treatments or oral antibiotics are necessary. Common treatment options include antibiotic ointments like mupirocin or fusidic acid, alongside oral antibiotics for more extensive or resistant cases. Maintaining proper hygiene, such as regular handwashing, avoiding scratching lesions, and disinfecting personal items, is crucial for recovery and preventing spread.
Persistent cases that do not respond to initial treatment within a week or two may indicate a more severe form of impetigo known as ecthyma. Ecthyma involves bacterial invasion deeper into the skin layers, often forming ulcerative lesions. This condition primarily affects the shins and legs and is more prevalent among elderly individuals or those with weakened immune defenses. Recognizing early signs of worsening infection and seeking medical attention promptly are vital to avoid complications.
Understanding the causes and staying vigilant about early symptoms can significantly help in managing impetigo effectively. Good hygiene practices, prompt treatment, and avoiding known risk factors are essential steps in preventing this contagious skin infection. Always consult healthcare professionals for accurate diagnosis and tailored treatment plans to ensure complete recovery and minimize the risk of transmission to others.
