Comprehensive Approaches to Managing Cutaneous Lupus Erythematosus
This comprehensive guide provides detailed insights into managing cutaneous lupus erythematosus through medications, lifestyle adjustments, and preventive strategies. Emphasizing sun protection, healthy habits, and regular medical monitoring, it aims to empower patients to control their symptoms and reduce disease progression effectively, improving overall quality of life.
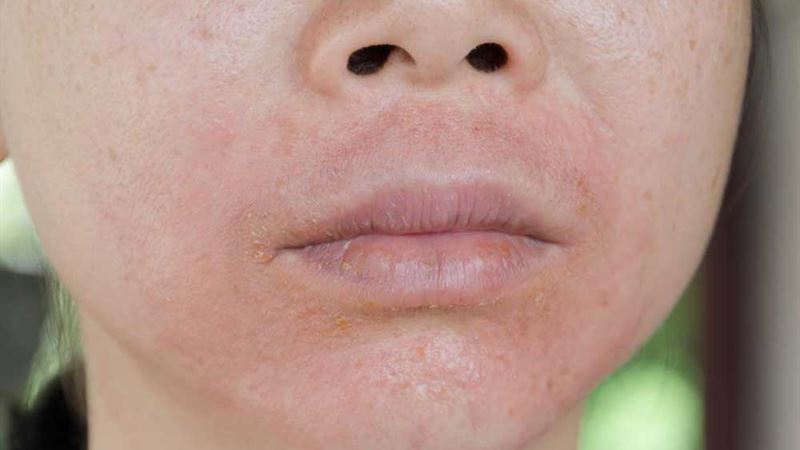
Medical Treatment Options for Lupus-Related Skin Conditions
Effective management of lupus skin symptoms often requires a tailored approach based on severity, extent of skin involvement, and individual health factors. The primary goal is to reduce inflammation, prevent flare-ups, and minimize long-term skin and organ damage. Here are some of the most commonly used treatment strategies:
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): These medications help alleviate joint pain, swelling, and inflammation, which are common in lupus. While many NSAIDs can be obtained over the counter, it is vital to consult a healthcare provider before use, especially for long-term therapy. They should be taken with food or milk to reduce gastrointestinal irritation. However, users need to be aware that prolonged use of NSAIDs can increase the risk of cardiovascular events such as strokes or heart attacks.
- Antimalarial Drugs: Agents like hydroxychloroquine and chloroquine are staples in lupus management. Besides their role in preventing lupus flares, they provide protection against skin damage from ultraviolet (UV) rays and help control symptoms such as joint pain, mouth sores, and skin rashes. These drugs also reduce the risk of blood clots, a concern for some lupus patients. Patients should be monitored regularly for eye health, as long-term use can affect vision.
- Corticosteroids: Corticosteroids such as prednisone are potent anti-inflammatory agents used in more severe cases of lupus. They suppress immune responses, helping resolve inflammation in blood vessels, lungs, kidneys, and other organs. When used topically or systemically, they can diminish skin rashes, swelling, and soreness. It is essential to use corticosteroids judiciously due to potential side effects, including osteoporosis, weight gain, and increased susceptibility to infections. Doctors typically prescribe the lowest effective dose for the shortest duration possible.
Supportive and Adjunct Therapies for Better Management
In addition to pharmacological treatments, supportive therapies play a crucial role in controlling lupus symptoms and preventing flare-ups. These include:
- Sun Protection: Ultraviolet radiation often worsens lupus skin lesions. Regular application of broad-spectrum sunscreen with high SPF, wearing protective clothing, and avoiding peak sunlight hours can significantly reduce skin sensitivity and flare-ups. The use of hats and sunglasses adds an extra layer of protection.
- Healthy Diet and Nutrition: Eating a balanced diet rich in anti-inflammatory foods, such as fruits, vegetables, omega-3 fatty acids, and whole grains, can help modulate immune responses and support overall health. Limiting processed foods and saturated fats may reduce inflammation.
- Lifestyle Modifications: Regular exercise, adequate rest, smoking cessation, and stress management are vital components of a comprehensive lupus care plan. Smoking, in particular, exacerbates vascular problems and increases disease severity, so quitting is highly recommended.
- Vaccinations: Staying up-to-date with flu, pneumonia, and other recommended vaccines protects lupus patients from infections, which they are more susceptible to due to immune-suppressing therapies.
Monitoring and Preventive Strategies
Routine medical checkups, laboratory tests, and skin examinations are essential to monitor disease activity and treatment response. Imaging and blood tests can detect early signs of organ involvement, allowing preemptive interventions. Patients are encouraged to keep a symptom diary and photograph skin lesions. This documentation aids healthcare providers in evaluating disease progression and tailoring treatment plans effectively.
Recognizing Symptoms and When to Seek Medical Advice
Lupus skin rashes typically appear as red, inflamed patches, often with a butterfly-shaped pattern across the cheeks and nose. Other signs include hair loss, sores in the mouth, and sensitivity to sunlight. Noticing these symptoms early and consulting a doctor can prevent escalation and organ involvement. Patients should seek immediate medical attention if they experience symptoms such as chest pain, severe fatigue, or neurological changes, which indicate possible systemic complications.
Conclusion and Preventive Tips
Living with lupus requires a proactive approach combining medical treatment, lifestyle choices, and vigilant health monitoring. Maintaining a healthy diet, avoiding triggers like sun exposure, quitting smoking, and ensuring adequate rest can significantly impact disease management. Also, regular screenings and medication adherence are key to preventing severe complications. With advancements in lupus research and personalized medicine, managing skin manifestations has become increasingly effective, helping patients lead healthier, more comfortable lives.
Images of lupus skin rashes serve as a diagnostic reference; however, early intervention and comprehensive care are crucial for optimal outcomes. Educating oneself about the condition and fostering a strong partnership with healthcare providers are essential steps toward effective disease control and improved quality of life.
