Comprehensive Overview of Sleep Apnea Risk Factors and Prevention Strategies
Discover the comprehensive risk factors that contribute to sleep apnea, from obesity and anatomical issues to lifestyle choices and medical conditions. Learn how age, gender, habits, and health concerns influence this prevalent sleep disorder. Early identification and lifestyle changes can help reduce risks and improve sleep quality. Consult professionals to explore effective treatment options and protect your overall health against sleep-disordered breathing.
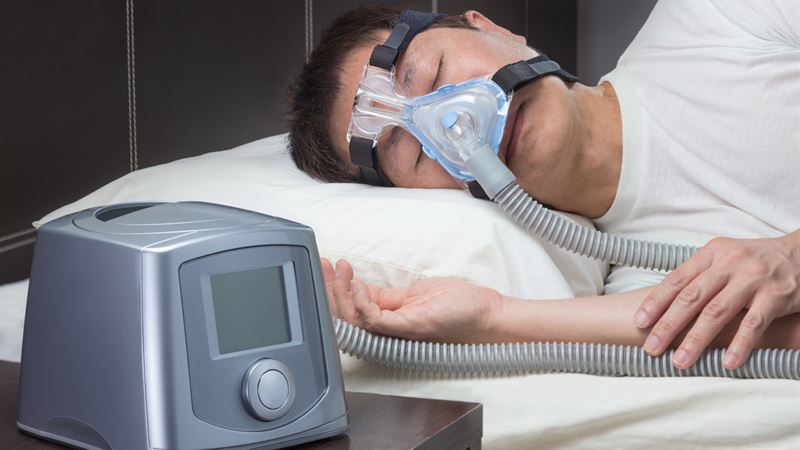
1. Excessive Body Weight
One of the most significant risk factors for sleep apnea is excess body weight or obesity. When an individual carries extra weight, particularly around the neck, it exerts pressure on the airway, causing it to narrow or partially collapse during sleep. This narrowing impedes airflow, leading to pauses in breathing that define sleep apnea. Furthermore, the accumulation of fat tissue under the chin can contribute to airway constriction, exacerbating the problem.
Obesity-related airway obstruction is often compounded by factors such as metabolic syndrome, insulin resistance, and other comorbidities that make the management of weight crucial for reducing sleep apnea risk. Maintaining a healthy body weight through diet, exercise, and lifestyle modifications is considered one of the most effective ways to lower the chances of developing sleep-disordered breathing.
2. Structural Narrowing of the Airway
Nasal congestion and structural abnormalities can significantly influence sleep apnea development. Partial blockage of the nasal passages due to allergies, sinus infections, or a deviated septum creates resistance in airflow, making breathing during sleep more difficult. Chronic nasal congestion, particularly when associated with allergic reactions, increases the likelihood of airway collapse during sleep cycles.
The soft tissues of the throat and nose may also collapse under the influence of gravity and relaxed muscles at night, further obstructing the respiratory pathways. These obstructions can cause repetitive pauses in breathing, reducing oxygen levels and disturbing sleep quality. Addressing nasal and structural issues through treatment options like decongestants, surgical correction, or nasal strips can help mitigate this risk.
3. Age and Gender-Related Factors
Age plays a crucial role in the prevalence of sleep apnea. Studies reveal that the likelihood of sleep-disordered breathing increases significantly in adults over 40 years old. As people age, muscle tone decreases, including the muscles in the upper airway. This decrease leads to increased airway collapsibility during sleep, heightening the risk of apneas and hypopneas.
Gender differences are also notable. Men are approximately three times more susceptible to sleep apnea than women of the same age group. The anatomical configuration of the male upper airway, combined with hormonal differences, contributes to this disparity. In men, the muscles of the throat tend to contract more vigorously during sleep, leading to potential airway collapse—a phenomenon known as oropharyngeal collapse. Additionally, postmenopausal women experience an increased risk, possibly due to hormonal changes affecting airway stability.
4. Lifestyle Choices and Habits
Certain lifestyle behaviors substantially influence the risk of sleep apnea. Smoking is a significant aggravator; it damages the mucous membranes in the throat and nose, leading to inflammation and swelling that narrows the airway openings. Nicotine in cigarettes causes increased muscle tone, which paradoxically worsens airway collapse and disrupts normal breathing during sleep.
Similarly, alcohol and sedatives profoundly impact sleep architecture. These substances relax the muscles of the upper airway, making it more prone to collapse. Regular alcohol consumption, especially before bedtime, can exacerbate existing airway issues, leading to more frequent breathing interruptions. Patients who consume sedatives or alcohol regularly should be aware of the increased sleep apnea risks and consider lifestyle modifications or medical consultation.
Other contributing factors include a sedentary lifestyle, poor sleep hygiene, and high alcohol intake. Adopting healthier habits, such as quitting smoking, limiting alcohol, and engaging in physical activity, can significantly reduce the risk or severity of sleep apnea.
5. Coexisting Medical Conditions
Several health issues contribute to the development or worsening of sleep apnea. Chronic allergies cause inflammation and swelling in the nasal passages, leading to airflow resistance. Conditions like hypothyroidism can also reduce muscle tone in the throat, increasing airway collapsibility. Additionally, structural abnormalities such as enlarged tonsils, adenoids, or a small jaw (micrognathia) can physically block the airway.
Patients with cardiovascular diseases, including hypertension and heart failure, are more likely to experience sleep apnea. This is partly due to shared risk factors like obesity and age but also because sleep apnea can cause blood pressure spikes and increase strain on the heart. Managing existing health conditions effectively can help minimize sleep apnea severity.
In conclusion, sleep apnea is a multifaceted disorder influenced by a combination of anatomical, physiological, lifestyle, and health-related factors. Recognizing these risk factors early allows for timely intervention, which can dramatically improve sleep quality, overall health, and quality of life. If you notice symptoms such as loud snoring, daytime fatigue, or breathing interruptions during sleep, it is crucial to consult a healthcare professional for assessment and personalized treatment options.
