Comprehensive Guide to Sleep Apnea: Causes, Symptoms, and Treatment Options
This comprehensive guide explores sleep apnea's causes, symptoms, diagnosis, and treatments, emphasizing the importance of understanding anatomical, lifestyle, and medical factors. It provides detailed insights into conventional therapies like CPAP and surgery, as well as natural remedies such as weight management and positional therapy, helping individuals manage this prevalent sleep disorder effectively.
- Severe snoring loud enough to disturb others
- Repeated breathing interruptions during sleep, often unnoticed by the sleeper
- Persistent fatigue and tiredness during the day despite adequate sleep
- Difficulty concentrating or memory problems
- Irritability and mood swings
- Dry mouth or sore throat upon waking
- Restless sleep or frequent awakenings
- Morning headaches
- Shortness of breath during sleep or waking up gasping
Obesity remains the leading cause of obstructive sleep apnea. Excess fat deposits around the neck and throat can constrict the airway, leading to breathing interruptions during sleep. The larger the neck circumference, the narrower the airway becomes, increasing the likelihood of collapse or obstruction. This physiological change results in increased effort to breathe and frequent interruptions, which fragment sleep and lead to daytime fatigue. Weight loss is often a fundamental aspect of managing and alleviating sleep apnea symptoms.
Structural features of the facial and respiratory anatomy play a significant role. For instance, individuals with a thick neck, enlarged tonsils, a small jaw, or a long palate are more prone to airway obstruction. The size and position of the tongue can also influence airway patency. Narrowed airways due to genetic predispositions or developmental anomalies can cause obstructive episodes during sleep. Surgical interventions or anatomical correction may be recommended when structural predispositions are identified.
Sleep apnea often runs in families, indicating a genetic component. Having relatives with sleep apnea increases the risk, highlighting the importance of family history in diagnosis. Hereditary anatomical differences may predispose individuals to airway obstruction irrespective of weight or other factors. Understanding genetic factors can help in early screening and preventive measures.
Heavy smoking causes inflammation and swelling of the upper airway tissues, leading to narrowing and increased likelihood of obstruction. Smokers are also prone to mucus accumulation and fluid retention, which exacerbate breathing difficulties. Lifestyle habits such as alcohol consumption and sedative use decrease muscle tone in the airway, increasing the risk of collapse. Quitting smoking and moderating alcohol intake can substantially reduce sleep apnea severity.
Nasal congestion due to allergies, sinus issues, or structural abnormalities impairs airflow, forcing mouth breathing during sleep. This impairs airflow and can contribute to apnea episodes. Persistent nasal blockages can significantly disturb sleep quality and exacerbate existing sleep apnea. Treatments targeting nasal congestion may provide relief and improve overall sleep quality.
Lying on the back or supine position is associated with increased airway collapse, especially in individuals predisposed to obstruction. This position causes gravity to pull the tongue and soft tissues backward, narrowing the airway. Habitual sleeping postures can be modified through positional therapy, which may lessen apnea episodes. Additionally, consistent sleep routines and avoiding late-night heavy meals can improve sleep architecture.
Various health conditions elevate the risk of sleep apnea. Patients with cardiovascular diseases, hypertension, type 2 diabetes, Parkinson’s disease, and stroke often experience higher prevalence rates. These comorbidities not only increase the likelihood of developing sleep apnea but can also worsen its severity. Managing these underlying medical issues with proper treatment can consequently improve sleep quality.
Accurate diagnosis of sleep apnea requires comprehensive evaluation. Sleep specialists typically recommend overnight polysomnography, a sleep study that monitors brain activity, eye movements, muscle activity, heart rate, airflow, and oxygen saturation. Home sleep testing devices are also available for simpler cases. Identifying the type and severity of sleep apnea guides clinicians in tailoring effective treatment plans tailored to individual needs.
- Continuous Positive Airway Pressure (CPAP) Therapy
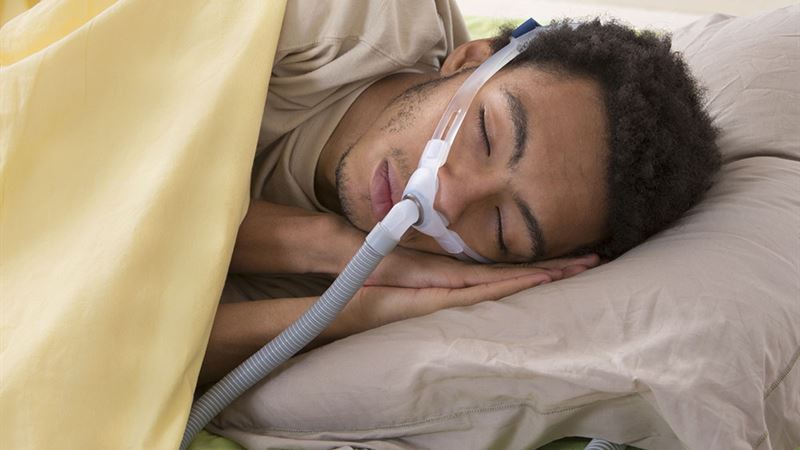
The most common and effective treatment for moderate to severe sleep apnea is CPAP therapy. It involves wearing a mask connected to a machine that delivers a steady stream of pressurized air to keep the airway open. Though highly effective, some patients find the mask uncomfortable, necessitating alternative options.
- Alternative Airway Pressure Devices
For those intolerant to CPAP, automatic adjustable airway pressure devices are available. These machines modify air pressure based on real-time needs, ensuring comfort while maintaining airway patency throughout the night. Such devices have improved compliance rates among users.
- Surgical Treatments
Surgery is considered a last resort when other treatments fail to provide relief. Surgical options depend on the individual’s specific anatomical issues and may include procedures such as uvulopalatopharyngoplasty (UPPP), maxillomandibular advancement, nasal surgeries, or nerve stimulation techniques. In severe cases, tracheostomy may be performed to bypass airway obstructions altogether.
- Natural and Lifestyle Remedies
Many patients benefit from natural approaches that complement medical treatments or serve as primary management options for mild cases. These include lifestyle modifications such as weight management, positional therapy, regular exercise, yoga, and relaxation techniques. Avoiding alcohol and sedatives, quitting smoking, and using humidifiers can also reduce symptoms.
Effective management of sleep apnea often requires combining multiple strategies—lifestyle changes, medical devices, and sometimes surgery. Continuous follow-up with healthcare providers ensures treatment efficacy and adjustments as needed. Awareness of sleep hygiene and ongoing health maintenance significantly improve outcomes and quality of life for those affected.
