Understanding Sjogren’s Syndrome: Causes, Symptoms, and Management Strategies
Sjogren’s Syndrome is a long-term autoimmune disorder primarily causing dryness in the mouth and eyes due to immune system attacks on glands. It often coexists with other autoimmune diseases, presenting diverse symptoms. While the exact cause remains unknown, infections and hormonal factors may influence its development. Managing symptoms through a combination of medications and lifestyle changes is crucial for quality of life. Early diagnosis and ongoing care are vital for preventing complications like dental problems, vision issues, and organ involvement. Continued research offers hope for future targeted therapies.
Sjogren’s Syndrome is a chronic autoimmune disorder characterized by the immune system mistakenly attacking the body's moisture-producing glands. Unlike infections that the immune system defends against, Sjogren’s causes inflammation and damage to these glands, leading to persistent dryness in various parts of the body. It primarily affects the salivary and lacrimal glands, resulting in dry mouth and eyes, but can also involve other organs, complicating the health condition. Since the root cause remains elusive, managing symptoms becomes essential for improving quality of life. The disease often coexists with other autoimmune diseases like rheumatoid arthritis, systemic lupus erythematosus, and sclerosis, making diagnosis and treatment more complex.
Understanding the causes of Sjogren’s Syndrome is critical for early diagnosis and effective management, though medical science has yet to uncover a definitive trigger. The prevailing theory suggests that certain genetic predispositions combined with environmental factors, such as viral or bacterial infections, may initiate the autoimmune reaction. These infectious agents might trigger the immune system to misidentify glandular tissues as threats, leading to immune aggression that damages secretory glands.
Additionally, hormonal influences may play a role, as the disease predominantly affects women, particularly those in middle age. Researchers believe that hormonal fluctuations interfere with immune regulation, possibly contributing to the development of Sjogren’s Syndrome. While some studies connect specific genetic markers to increased susceptibility, conclusive evidence remains lacking, and more research is necessary to understand the intricate causes.
The symptoms of Sjogren’s Syndrome are varied and often progressive. The hallmark features include dryness in the mouth and eyes, but systemic manifestations can affect multiple organs and tissues, complicating diagnosis and treatment. Recognizing these symptoms early is crucial to prevent long-term complications, such as dental decay, eye damage, and other secondary conditions.
Common Symptoms and Signs of Sjogren’s Syndrome
- Persistent dry mouth (xerostomia) is one of the earliest and most noticeable symptoms. Patients often describe an unusual chalky or sticky sensation inside the mouth, coupled with difficulty in chewing, speaking, or swallowing. Over time, this dryness can hinder the natural protective mechanisms of the oral cavity, leading to increased susceptibility to oral infections, such as candidiasis (yeast infections). The lack of saliva also contributes to dental issues like cavities and gum disease.
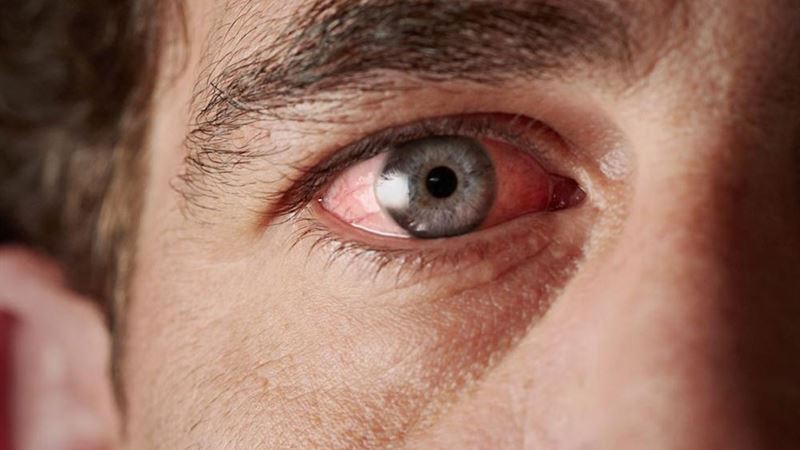
- Dry eyes are equally prominent, resulting from decreased tear production. Patients may experience sensations of burning, itching, or a gritty feeling in the eyes. These symptoms can significantly reduce visual comfort and clarity, especially during prolonged screen time or exposure to wind and dust. Without adequate treatment using artificial tears or other ocular medications, prolonged dry eyes can risk corneal damage and potentially impair vision.
- Beyond the mouth and eyes, other areas can be impacted. The skin may become dry, leading to dermatitis or cracking and sensitivity. The nose might experience dryness and frequent crusting or bleeding, and lips often become chapped or cracked. Swelling of glands in the face, especially around the jaw and neck, is also common and results from lymphocytic infiltration and inflammation.
- Systemic symptoms, such as fatigue, joint pain, and muscle aches, are seen in many patients. Sometimes, Sjogren’s Syndrome causes persistent dryness in the throat, making breathing and speaking uncomfortable. Some individuals also report experiencing rashes or skin sensitivity, and in rare cases, organ involvement can lead to complications like kidney problems, liver inflammation, or nerve issues.
Managing Sjogren’s Syndrome involves a multidisciplinary approach aimed at alleviating symptoms, preventing complications, and improving patients' quality of life. Treatment strategies focus on relieving dryness symptoms, controlling inflammation, and protecting affected organs. Although there is no cure for Sjogren’s, ongoing research continues to explore targeted therapies to modulate the immune response and address the underlying causes.
Lifestyle modifications, such as maintaining good oral and ocular hygiene, staying well-hydrated, and avoiding environmental irritants, are essential. Medical interventions include artificial saliva, eye drops, and medications like immunosuppressants or anti-inflammatory drugs for systemic involvement. Regular monitoring by healthcare professionals ensures early detection of potential complications and appropriate management adjustments.
Despite the chronic nature of Sjogren’s Syndrome, many individuals achieve a manageable quality of life with proper care. Awareness of the disease’s symptoms and early intervention remain critical in preventing severe complications and enhancing overall health and well-being. Advances in autoimmunity research hold promise for more effective future therapies, offering hope to those affected.
