Understanding Sjogren’s Syndrome: Causes, Symptoms, and Management
Sjogren’s Syndrome is a chronic autoimmune condition characterized by dryness in the mouth, eyes, and other tissues due to immune system attacking moisture-producing glands. Though its exact cause remains unknown, it often accompanies other autoimmune diseases. Early diagnosis and comprehensive management can alleviate symptoms and prevent complications. This detailed guide explores causes, symptoms, diagnosis, and treatment options, offering essential insights for patients and caregivers to live healthier lives with Sjogren’s Syndrome.
Sjogren’s Syndrome is a chronic autoimmune disorder that primarily targets moisture-producing glands in the body. In this condition, the immune system, which normally defends against infections, mistakenly attacks healthy tissues and glandular cells, leading to significant dryness in various parts of the body. While the exact reasons behind this malfunction are yet to be fully understood, it is clear that Sjogren’s Syndrome often coexists with other autoimmune diseases such as rheumatoid arthritis, lupus, or scleroderma, adding complexity to diagnosis and treatment. Since a complete cure isn’t currently available, managing symptoms and improving quality of life become the primary focus for individuals living with this condition.
Understanding the underlying causes and recognizing the signs early can help in better management and prevent complications. This comprehensive article delves into the origins, typical symptoms, diagnosis, possible treatment options, and lifestyle adaptations necessary for living with Sjogren’s Syndrome. By increasing awareness and knowledge about this condition, patients and caregivers can make informed decisions to cope effectively with this lifelong disease.
What Are the Root Causes of Sjogren’s Syndrome?
Although medical science has yet to pinpoint a definite cause, researchers believe that a combination of genetic, environmental, and hormonal factors may contribute to the development of Sjogren’s Syndrome. It is believed that certain genetic predispositions make some individuals more vulnerable to this autoimmune response. Environmental triggers, such as infections caused by bacteria or viruses, appear to activate the immune system in susceptible individuals, leading to an aberrant immune response.
This abnormal immune activity results in the white blood cells attacking the body’s moisture-producing glands—most notably the salivary glands in the mouth and the lacrimal glands that produce tears. The process can also extend to other organs and tissues, leading to various systemic symptoms. It is hypothesized that these autoimmune responses may stem from molecular mimicry, where pathogens' proteins resemble tissues in the body, confusing the immune system into attacking its own cells.
Despite ongoing research, a comprehensive understanding of why some people develop Sjogren’s Syndrome remains elusive. Scientists continue exploring the role of genetic markers, hormonal influences, and environmental factors in an effort to unlock potential preventive measures and targeted therapies.
Common Symptoms and Signs of Sjogren’s Syndrome
The diverse symptoms of Sjogren’s Syndrome can vary widely among individuals, often making diagnosis challenging. However, certain hallmark signs often signal the presence of this autoimmune disorder. Recognizing these early can lead to prompt medical attention and better management of the disease.
- Dry Mouth (Xerostomia): One of the most characteristic features, dry mouth results from reduced saliva production due to damage to salivary glands. Patients frequently describe a feeling of mouth dryness, a chalky or sticky sensation, and difficulty in chewing or swallowing food. Persistent dryness may also lead to an increased risk of dental decay, mouth infections like candidiasis, and discomfort while speaking.
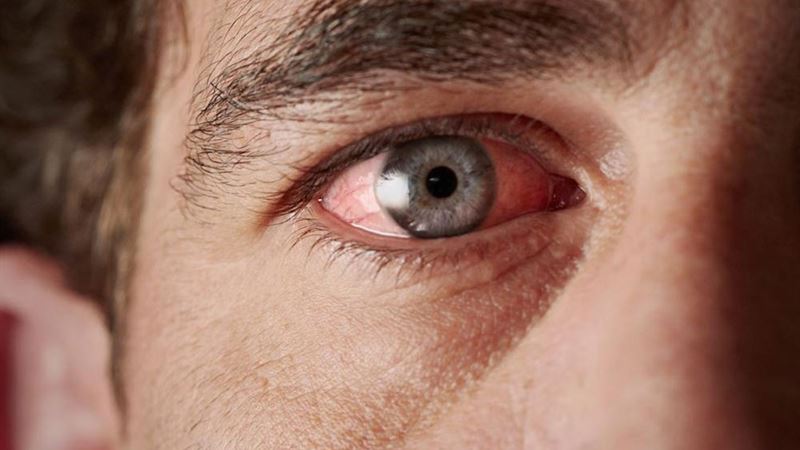
- Dry Eyes (Keratoconjunctivitis Sicca): The impairment of tear production causes eyes to become dry, itchy, and red. Many sufferers report a burning sensation, sensitivity to light, and a gritty sensation reminiscent of having foreign particles in the eyes. If left untreated, dryness can cause damage to the cornea and conjunctiva, potentially leading to vision issues.
- Swelling and Discomfort in Glands: Swelling may occur in glandular areas like the face, neck, and jaw due to inflammation. These swellings often accompany discomfort or tenderness, further indicating glandular involvement.
- Other Systemic Manifestations: Sjogren’s isn’t limited to moisture glands. It can also affect other parts of the body including the throat, lips, nose, and skin. Some individuals experience joint pain, fatigue, and muscle aches, common symptoms shared with other autoimmune diseases. Rarely, internal organs such as kidneys, liver, or lungs may become involved, leading to more serious health complications.
Additional symptoms can include dry skin, persistent cough, difficulty swallowing, and in some cases, neurological issues like numbness or tingling sensations. The severity varies greatly, and some people may experience mild symptoms, while others suffer from significant health challenges.
Diagnosis: How Is Sjogren’s Syndrome Confirmed?
Diagnosing Sjogren’s Syndrome involves a combination of clinical evaluation, laboratory testing, and imaging studies. Since symptoms often resemble those of other conditions, proper diagnosis can be a lengthy process requiring specialized assessments.
- Medical History and Physical Examination: The physician reviews symptom history, focusing on dryness in the mouth and eyes, glandular swelling, and systemic symptoms. Physical examination includes checking the salivary glands and eye health.
- Blood Tests: These tests evaluate indicators of autoimmune activity, including the presence of specific antibodies such as anti-Ro/SSA and anti-La/SSB. Elevated levels of inflammatory markers like ESR and CRP may support the diagnosis.
- Schirmer’s Test and Tear Breakup Time: These ocular tests measure tear production and stability, helping confirm dry eye syndrome.
- Salivary Gland Imaging: Techniques such as ultrasound, sialography, or scintigraphy provide visual confirmation of glandular damage.
- Biopsy: Minor salivary gland biopsies are often performed to identify lymphocytic infiltration and confirm autoimmune involvement.
Management and Treatment Strategies for Sjogren’s Syndrome
While there is no permanent cure for Sjogren’s Syndrome, various approaches aim to relieve symptoms, prevent complications, and improve overall quality of life. A personalized treatment plan often involves a multi-disciplinary team comprising rheumatologists, ophthalmologists, dentists, and primary care providers.
- Symptom Relief: Artificial tears and eye lubricants help manage dry eyes. Saliva substitutes and mouth rinses can alleviate oral dryness. Staying well-hydrated and avoiding irritants like caffeine and tobacco also support symptom management.
- Medications: Prescribed drugs include immunosuppressants, corticosteroids, and disease-modifying anti-rheumatic drugs (DMARDs) to control immune activity. Certain medications like pilocarpine and cevimeline can stimulate saliva production.
- Dental Care: Regular dental check-ups, fluoride treatments, and good oral hygiene are crucial to prevent decay and infections caused by dry mouth.
- Lifestyle and Home Remedies: Adopting a healthy lifestyle, including a balanced diet, stress management, and avoiding environmental triggers, can reduce symptom severity.
- Monitoring and Managing Complications: Regular assessments for systemic involvement ensure early detection of any organ involvement or secondary conditions, such as lymphoma, which although rare, can develop in some cases.
Living with Sjogren’s Syndrome: Tips and Recommendations
Living with a chronic condition like Sjogren’s Syndrome requires ongoing management and lifestyle adaptations. Here are some practical tips to help cope effectively:
- Maintain excellent oral and eye hygiene to prevent infections and damage.
- Use humidifiers at home and work to reduce dryness indoors.
- Stay hydrated by drinking plenty of water throughout the day.
- Avoid environmental factors that worsen dryness, such as wind, smoke, and extreme heat or cold.
- Attend regular medical appointments for monitoring disease progression and adjusting treatments accordingly.
- Join support groups or patient communities to share experiences and gain emotional support.
- Relaxation techniques and stress management can help modulate immune response and improve overall well-being.
Understanding Sjogren’s Syndrome thoroughly can empower patients to manage their condition proactively. While living with this disease can be challenging, effective symptom control, lifestyle modifications, and medical care significantly enhance quality of life and reduce the risk of complications.
