Comprehensive Guide to Rheumatoid Arthritis: Recognizing Symptoms and Identifying Key Healthcare Professionals for Treatment
This comprehensive article explores rheumatoid arthritis, emphasizing immune system involvement, symptoms, potential complications, and the vital roles of various healthcare professionals in managing the disease. Early diagnosis and multidisciplinary treatment are key to controlling RA and maintaining quality of life. Understand the importance of different specialists and recognize early signs to seek timely care, potentially preventing joint damage and systemic complications.
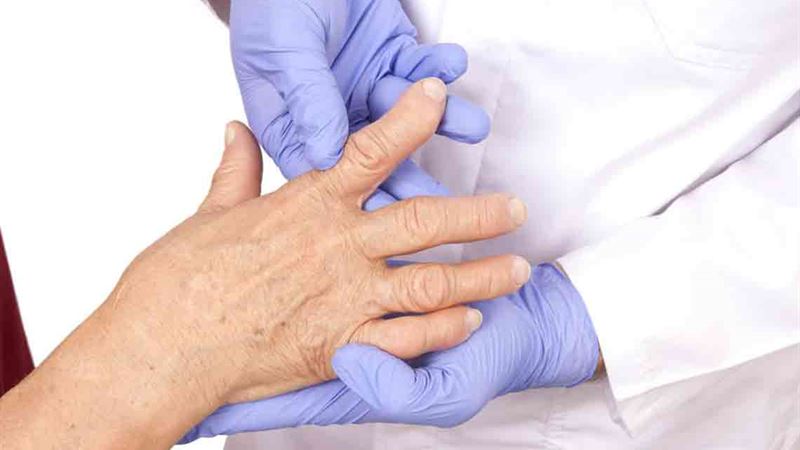
Rheumatoid arthritis (RA) is a chronic autoimmune disorder that affects millions worldwide, leading to joint inflammation, pain, and potential deformities. Research indicates that genetic predisposition plays a significant role in the development of RA, with environmental factors such as smoking tobacco further increasing risk. Understanding this complex disease and the associated risks is crucial for early diagnosis and effective management.
Beyond joint inflammation, rheumatoid arthritis can impact various organs and bodily systems, posing serious health threats if untreated. For example, inflammation of salivary and tear glands can cause significant dryness in the mouth and eyes, impairing vision and increasing the risk of infections. Pulmonary involvement, such as inflammation of lung linings, can lead to respiratory issues like persistent dry cough and breathing difficulties, which can escalate in severity if not properly managed.
One of the most concerning complications for RA patients is the heightened risk of cardiovascular events, including heart attacks. The systemic inflammation associated with RA contributes to accelerated atherosclerosis, increasing the likelihood of cardiovascular disease. This underscores the importance of holistic management strategies and regular monitoring to mitigate such risks.
Diagnosing rheumatoid arthritis can be complex due to its variable symptoms, which may fluctuate over time. Many individuals experience episodes of joint stiffness, swelling, and pain that come and go, making it challenging for laypersons to recognize the disease early. Symptoms such as sudden joint stiffness, persistent fatigue, loss of appetite, and generalized malaise often signal underlying RA activity.
Children can also be affected by juvenile rheumatoid arthritis, exhibiting symptoms like limping, persistent crying, and decreased appetite. Recognizing these signs early is vital for prompt diagnosis and treatment, which can prevent joint damage and improve quality of life.
To accurately diagnose rheumatoid arthritis, healthcare providers conduct comprehensive assessments involving clinical examinations, blood tests (such as rheumatoid factor and anti-CCP antibodies), and imaging studies like X-rays or MRIs. These tests help distinguish RA from other joint conditions and determine disease severity. It's worth noting that joint pain alone is not sufficient for diagnosis, as similar symptoms can arise from other musculoskeletal issues.
Types of Healthcare Professionals Involved in Rheumatoid Arthritis Management
Managing rheumatoid arthritis necessitates a multidisciplinary approach involving various specialists. Understanding the roles of these healthcare providers can help patients seek appropriate treatment early and efficiently.
Primary Care Physician
The first contact for individuals noticing early symptoms of RA should be their primary care physician or family doctor. These doctors have detailed knowledge of the patient’s health history, lifestyle, and risk factors, making them essential for initial assessments. They can perform preliminary examinations, order diagnostic tests, and, crucially, refer patients to specialists such as rheumatologists or orthopedists for advanced care.
Orthopedic Surgeon
Orthopedic surgeons specialize in the diagnosis and treatment of musculoskeletal conditions, including joint disorders and injuries. When rheumatoid arthritis causes severe joint damage or deformity, surgical interventions like joint replacement or repair may be necessary. An orthopedic surgeon evaluates the extent of joint destruction and determines the most appropriate surgical options to restore function and alleviate pain.
Rheumatologist
Rheumatologists are specialists dedicated exclusively to diagnosing and managing autoimmune and systemic inflammatory conditions like RA. They possess in-depth knowledge of immune system abnormalities and use various laboratory and imaging tools to confirm diagnosis. Rheumatologists craft personalized treatment plans, which may include disease-modifying antirheumatic drugs (DMARDs), biologics, and other immunosuppressive therapies aimed at controlling inflammation and preventing joint deterioration.
Physiotherapist
Physical therapists play a crucial role in maintaining joint mobility and muscle strength in RA patients. They develop tailored exercise routines, stretching, and physical activities designed to reduce stiffness and improve joint function. Regular physiotherapy can also help decrease pain, enhance flexibility, and promote overall physical well-being, making daily activities easier and less painful.
Occupational Therapist
Occupational therapists assist individuals in adapting to physical limitations caused by RA to maintain independence in daily tasks. They teach techniques to reduce strain on affected joints, recommend assistive devices, and modify home or work environments to accommodate mobility challenges. These interventions enhance the patient’s quality of life by enabling safer and more comfortable performance of routine activities.
If you suspect you have rheumatoid arthritis, providing a detailed account of your symptoms to your healthcare provider is vital. Accurate information allows for effective diagnosis and the development of a comprehensive treatment plan tailored to your specific needs.
Overall, understanding the roles of these key healthcare providers and recognizing early signs of RA can significantly improve prognosis and quality of life. Early diagnosis, combined with multidisciplinary management, offers the best chance to control disease progression and prevent severe complications.
