The Critical Role of Neutrophils in Immune Defense and Disease Processes
Neutrophils are crucial immune cells originating from the bone marrow, forming nearly half of circulating white blood cells. They defend against bacterial infections through rapid migration, phagocytosis, and NET formation. Low neutrophil levels, or neutropenia, can be caused by genetic disorders, infections, medications, or diseases like leukemia. While essential for infection control, neutrophils can also contribute to autoimmune tissue damage. Understanding their functions and challenges is vital for managing immune-related conditions and autoimmune diseases effectively. This comprehensive review highlights their pivotal role in health and disease.
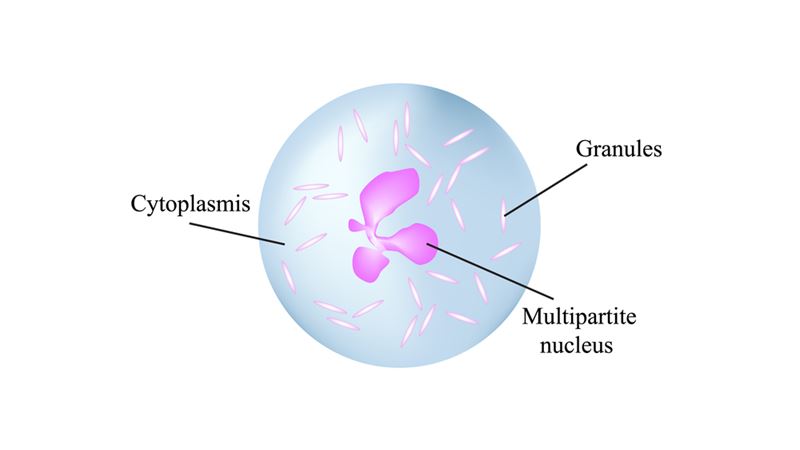
- Among the various types of white blood cells, neutrophils belong to the group known as polymorphonuclear leukocytes because of their lobed nucleus structure, which they share with basophils and eosinophils. These cells are distinguished by their staining properties, which give them a neutral pink hue—hence the name 'neutrophil.'
Understanding Neutropenia: When Neutrophil Levels Drop
- Sometimes, the body experiences a decline in neutrophil numbers—a condition known as neutropenia. This decrease impairs the immune system's ability to fend off bacterial and fungal infections, leaving individuals more susceptible to illnesses.Various medical conditions and external factors can cause neutropenia, leading to increased health risks. Recognizing these causes is vital for diagnosis and treatment planning.
Causes of Neutropenia and Low Neutrophil Counts
- Genetic disorders, such as Kostmann syndrome and myelokathexis, inherently result in decreased neutrophil production. These congenital conditions impair the bone marrow's ability to generate adequate neutrophil levels from birth.
- Medical treatments like chemotherapy and radiation therapy, which target rapidly dividing cells, unintentionally harm neutrophil production, leading to temporary or prolonged neutropenia.
- Infections caused by bacteria, viruses, and parasites can either consume neutrophils rapidly or suppress their production. Diseases such as tuberculosis, typhoid, hepatitis A, B, C, HIV/AIDS, malaria, and deficiencies like vitamin B12 deficiency are notable examples.
- Severe infections, especially sepsis, overwhelm neutrophil reserves by utilizing them faster than they can be replenished, resulting in critically low numbers.
- Blood cancers such as leukemia, along with autoimmune disorders and hypersplenism, can cause destruction or sequestration of neutrophils, reducing their availability in circulation. Certain medications, including antibiotics and other immunosuppressive drugs, can also induce neutropenia.
The Multifaceted Functions of Neutrophils in Immune Defense
- The primary role of neutrophils is to neutralize and eliminate bacterial pathogens swiftly, acting as the body's first line of defense.
- Upon detecting infection, neutrophils migrate from the bloodstream through the endothelial lining of blood vessels into the tissues—a process known as chemotaxis. This migration is highly coordinated and rapid, often occurring within minutes.
- During migration, neutrophils extend pseudopodia—cellular projections resembling amoeba—that probe the environment for chemical signals. These pseudopodia are rich in receptors to detect chemotactic factors released at infection sites, guiding neutrophils precisely where needed.
- Modern research introduces the concept of neutrophil swarming, a sophisticated coordination mechanism where neutrophils communicate with each other and other immune cells to optimize the inflammatory response and pathogen clearance.
Mechanisms of Neutrophil-Mediated Killing of Pathogens
- Neutrophils utilize pseudopodia to surround and engulf bacteria and other pathogens, a process called phagocytosis. This physical barrier facilitates the delivery of potent antimicrobial substances directly to the invaders.
- Degranulation follows phagocytosis, releasing a cocktail of enzymes and reactive oxygen species—such as myeloperoxidase, elastase, and collagenase—that destroy bacteria and decontaminate the infection site.
- An especially intriguing defense mechanism involves the formation of Neutrophil Extracellular Traps (NETs). These nets are composed of chromatin fibers decorated with antimicrobial proteins, creating a physical and chemical barrier that traps and kills bacteria extracellularly.
- NETs serve a dual purpose by immobilizing pathogens and concentrating bactericidal chemicals, making them highly effective against various microbes—even those resistant to standard antibiotics.
Neutrophils and Autoimmune Diseases: Double-Edged Sword
- While neutrophils are essential for fighting infections, their activity can inadvertently contribute to tissue damage in autoimmune diseases. They can release enzymes and inflammatory mediators that degrade host tissues, exacerbating disease progression.
- Research indicates that neutrophils play active roles in promoting inflammation in conditions like rheumatoid arthritis, vasculitis, and systemic lupus erythematosus. They also participate in the development and progression of atherosclerotic plaques by weakening the fibrous cap of arterial lesions, increasing the risk of cardiovascular events.
- Recent findings suggest that neutrophils are a significant source of autoantigens—molecules that trigger autoantibody production—further fueling autoimmune responses and chronic inflammation.
