Comprehensive Guide to Percutaneous Lumbar Laser Disc Decompression: Innovation in Minimally Invasive Spine Therapy
Explore the evolution, clinical effectiveness, and benefits of percutaneous lumbar laser disc decompression (PLDD), a minimally invasive alternative to traditional spinal surgery. Discover how laser technology offers targeted relief for herniated discs and spinal stenosis, with high success rates and quicker recovery times, making it a preferred choice for suitable patients worldwide.
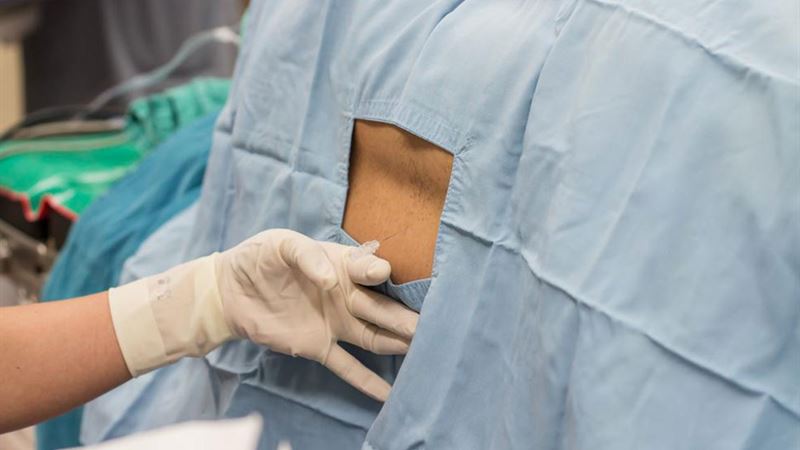
In recent years, advancements in medical technology have revolutionized the way lumbar disc herniations and spinal stenosis are treated, leading to minimally invasive procedures that significantly reduce recovery time and improve patient outcomes. Among these cutting-edge treatments, percutaneous lumbar laser disc decompression (PLDD) stands out as a minimally invasive and effective alternative to traditional open surgeries. This procedure harnesses laser technology to alleviate disc herniation symptoms with minimal tissue disruption, making it increasingly popular worldwide.
Understanding the origins and development of PLDD provides insight into its role within modern spinal surgery. The concept of utilizing laser energy to address herniated discs was first conceived in the early 1980s, during a period of rapid innovation in laser applications across various medical fields. Researchers and clinicians experimented with different laser wavelengths and delivery systems to optimize safety and efficacy. Following extensive laboratory testing, the first percutaneous laser disc decompression procedure was performed, showcasing promising results that prompted further investigation.
By 1991, the FDA (Food and Drug Administration) in the United States had approved the use of specific laser systems for lumbar disc decompression, paving the way for widespread clinical adoption. Since then, laser spine institutes across the U.S. and around the world have adopted PLDD as a standard minimally invasive option for suitable patients suffering from herniated discs and spinal stenosis. The procedure's appeal lies in its ability to target problematic disc tissue precisely while minimizing damage to surrounding structures, reducing patient discomfort, and decreasing hospitalization durations.
Clinical Evidence Supporting PLDD Effectiveness
Numerous studies and clinical trials have demonstrated the safety and efficacy of percutaneous lumbar laser disc decompression. One of the earliest prospective, controlled studies was conducted by Duarte and Costa and published in 2000. This study focused on patients undergoing PLDD under computer tomography (CT) guidance and local anesthesia, emphasizing the importance of precise targeting and minimally invasive techniques. Researchers established clear selection criteria to identify patients most likely to benefit, including specific symptom duration, disc herniation characteristics, and imaging findings.
Utilizing the MacNab criteria, which assess functional recovery, pain relief, and dependency on analgesics, the study found that approximately 67% of patients achieved good results, with an additional 9% attaining acceptable outcomes. This data highlighted the procedure’s potential as a reliable treatment for lumbar disc herniations, especially in carefully selected patients. Over subsequent years, similar observational studies have reinforced these findings, reporting successful outcomes in up to 80% of cases, with patients experiencing significant pain reduction and improved mobility.
In particular, a study published in 2005 by Zhao and colleagues provided further insight into patient selection and treatment success. Their case-control analysis revealed that patients classified as having a “good” indication responded exceptionally well—about 82% achieved either good or excellent results—compared to 56% in those with less classic indications. These findings stress the importance of proper patient selection criteria to maximize the benefits of PLDD.
Overall, the accumulated clinical data suggest that laser disc decompression is a highly effective interventional technique when performed on appropriate candidates. Its minimally invasive nature translates into shorter recovery times, reduced procedural risks, and less post-procedure discomfort, making it an attractive alternative to traditional open surgery for lumbar disc herniation and spinal stenosis.
Today, with ongoing technological advancements and expanding clinical experience, PLDD continues to evolve. It is increasingly employed for various lumbar spine conditions, including discogenic pain and early degenerative disc disease. Physicians worldwide are integrating laser decompression into their treatment algorithms, often combining it with other minimally invasive procedures for comprehensive spinal care.
The adoption of PLDD not only enhances patient outcomes but also reduces healthcare costs by decreasing the need for extensive surgeries and prolonged hospital stays. As research progresses, further innovations are expected to improve procedural precision, safety, and long-term results, solidifying PLDD’s role in the future landscape of spine medicine.
