Understanding Mycosis Fungoides: Beyond a Skin Rash
Mycosis fungoides is a rare skin lymphoma that progresses slowly through distinct stages, from patches to tumors. Often mistaken for benign conditions, early detection is vital. This comprehensive guide explores symptoms, progression, diagnosis, and treatment options for this complex disease, emphasizing the importance of medical consultation for persistent skin abnormalities to ensure timely intervention and better prognosis.
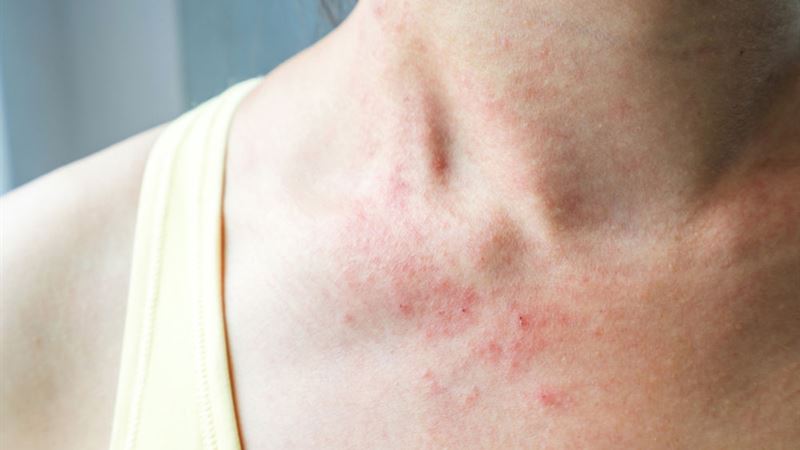
Recognizing Symptoms of Mycosis Fungoides
The progression of this disease is typically slow, making early detection challenging. It advances through distinct stages, with each characterized by specific skin manifestations.
Initial Stage
During the first phase, affected skin often exhibits patches of redness and scaling that are similar to eczema, psoriasis, or dermatitis. These patches tend to appear in areas with limited sun exposure, such as the hips, buttocks, or inner thighs. The redness and scale may persist for months or even years, often causing confusion with benign skin conditions. Some individuals may notice mild itching or irritation, but many remain asymptomatic during this phase.
Second Stage
As the disease progresses, the patches tend to become thicker and more scaly, transforming into raised plaques. These plaques are often irregular in shape and resistant to standard topical treatments, making diagnosis more complex. The skin in these areas may feel firmer and may develop a rougher texture. The persistent nature of these patches warrants close medical attention.
Third Stage
The affected areas may develop raised lesions—red bumps or nodules—that can be tender or painful. Over time, these plaques can evolve into hard, thickened patches known as tumors, indicating more advanced disease. These tumors have the potential to ulcerate or break open, which increases the risk of secondary infections and complicates treatment.
Fourth Stage
At this terminal phase, tumors may enlarge, sometimes forming ulcers or open sores. The cancer can spread beyond the skin via lymphatic systems, reaching lymph nodes and other organs. This dissemination marks a significant escalation in severity; early intervention becomes critical at this point to prevent systemic spread. It is important to recognize that not all patients experience all four stages, and the disease course can vary significantly among individuals.
While many patients keep the disease confined to the skin, there are cases where it advances, affecting internal organs and lymph nodes, which necessitates aggressive treatment approaches. The prognosis depends heavily on the extent of disease spread and response to therapy.
Healthcare providers emphasize the importance of consulting an oncologist or dermatopathologist if persistent, unusual skin changes occur—particularly those resistant to conventional therapies. Early diagnosis and management are key to improving outcomes and quality of life.
