Comprehensive Guide to Advanced Insulin Delivery Systems for Diabetes Management
Explore the latest advancements in insulin pump technology for effective diabetes management. This comprehensive guide covers various pump types, their functionalities, benefits, and how they help improve blood sugar control and quality of life for individuals with diabetes. Learn about the integration with continuous glucose monitoring, differences between tubed and tubeless pumps, and how these devices are transforming patient care and independence.
Managing diabetes effectively requires innovative solutions that enhance quality of life and improve health outcomes. Modern insulin delivery devices, especially insulin pumps, have revolutionized diabetes care by providing precise, adjustable, and user-friendly options. These devices are designed to emulate natural insulin release, offer flexibility, and integrate advanced technology such as continuous glucose monitoring (CGM) systems. This comprehensive guide explores the various types of insulin pumps, their working mechanisms, benefits, and how they represent a significant advancement in diabetes treatment.
Insulin pump technology has progressed tremendously over recent decades, offering a level of control and convenience that traditional insulin injections cannot match. Patients benefit from greater autonomy in their daily routines, with options tailored to different lifestyles and preferences. Whether you are considering starting insulin pump therapy or want to understand the latest developments, this detailed overview provides essential insights into how these devices can transform diabetes management.
Understanding Insulin Pumps: How Do They Work?
At the core, insulin pumps are sophisticated medical devices engineered to deliver insulin in a manner similar to the body's natural production. The primary goal is to maintain optimal blood glucose levels, preventing both hyperglycemia and hypoglycemia. These devices work continuously by administering small, basal doses of insulin throughout the day and night, complemented by larger bolus doses tailored to specific needs such as meals or correction of high blood sugar.
Modern pumps can be programmed fully or partially to depend on real-time data inputs, thanks to embedded CGM systems. This allows for automatic adjustments of insulin delivery based on fluctuations in blood glucose levels, significantly reducing the burden on patients to manually calculate dosages. Patients can also manually set insulin doses after consulting with their healthcare team, ensuring personalized care tailored to their routines and metabolic responses.
Types of Insulin Pumps: A Comparative Overview
Choosing the right insulin pump depends on various factors, including lifestyle, comfort preferences, and medical needs. There are primarily two categories: tubed (or tethered) pumps and tubeless pumps. Each type offers unique benefits and considerations, making it essential to understand their features thoroughly.
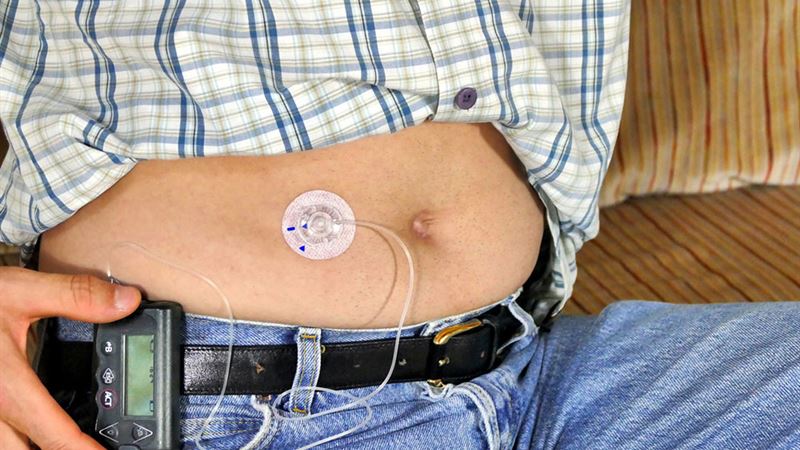
- Traditional Tubed Insulin Pumps: Known as tethered pumps, these devices feature a small, lightweight pump connected via a thin flexible tube to a cannula inserted beneath the skin. The reservoir within the pump holds insulin, typically enough for two to three days of use, depending on individual requirements. The pump’s control interface includes a display screen allowing users to monitor insulin delivery, view glucose readings if integrated with CGM, and input data manually. Batteries or rechargeable power sources keep the device operational.
- Tubeless (Patch) Insulin Pumps: These modern, discreet devices are comprised of a small, single-use pod that adheres directly to the skin, eliminating the need for tubing. The pod contains both the insulin reservoir and the cannula, which is inserted under the skin. Patients control and monitor these devices via a wireless controller or smartphone app. The pod typically lasts two to three days before needing replacement. Its waterproof design allows users to shower, bathe, or swim without disconnection, offering enhanced convenience and freedom.
Both systems have their advantages: tubed pumps tend to offer more customization and longer usage periods, making them suitable for many adults, while tubeless pumps provide greater mobility and discretion, which can be particularly appealing to younger users or those engaged in active lifestyles.
Advantages of Using Insulin Pumps for Diabetes Control
Modern insulin pumps have revolutionized management strategies for diabetes, especially type 1 diabetes, providing significant clinical and lifestyle benefits. Here are some of the most notable advantages:
- Enhanced Precision: Pumps deliver insulin with acute accuracy and can be fine-tuned based on the patient's changing needs, reducing variability and improving overall control.
- Flexibility & Lifestyle Compatibility: With programmable basal rates and bolus dosing, patients can better align insulin delivery with their daily activities, eating habits, and exercise routines.
- Integration with Continuous Glucose Monitors: When combined with CGMs, pumps can automate insulin adjustment through predictive algorithms, minimizing manual calculations and oversight.
- Data Collection & Sharing: Pumps log detailed data on insulin delivery and glucose trends, which can be downloaded, analyzed, and shared with healthcare providers for ongoing treatment optimization.
- Reduced Injection Discomfort: Using a pump minimizes the need for multiple daily injections, improving comfort and compliance.
Furthermore, advancements in sensor technology and artificial intelligence are making insulin pump therapy increasingly adaptive, paving the way for closed-loop systems that adapt in real-time to ongoing glucose fluctuations, further enhancing safety and efficacy.
Who Can Benefit from Insulin Pumps?
While insulin pumps are especially beneficial for type 1 diabetes patients across all age groups, certain individuals with other forms of diabetes may also qualify, such as those with type 2 diabetes who require intensive insulin therapy. Patients experiencing frequent hypoglycemia or wide glucose fluctuations often find significant improvements in their condition through pump therapy. Moreover, highly active individuals, pregnant women with diabetes, or those seeking to improve their glycemic control and quality of life may consider insulin pumps as an optimal treatment modality.
Considerations & Potential Challenges
Despite their benefits, insulin pumps require careful management, patient education, and regular monitoring. Proper insertion, site rotation, device maintenance, and understanding of alarms and malfunctions are essential to maximize benefits. Cost considerations, insurance coverage, and device maintenance can also be barriers for some users. Engaging with healthcare providers to select the appropriate device type and to establish effective training is crucial for successful adoption.
In conclusion, insulin pump technology offers a revolutionary approach to diabetes management, combining precision, flexibility, and convenience. As the field advances with smarter, more integrated systems, patients can look forward to even better control, fewer complications, and an improved quality of life. Whether through tubed or tubeless options, insulin pumps continue to set new standards in personalized diabetes care and management.
