Comprehensive Guide to Various Types of Radiation Therapy for Cancer Treatment
Discover a detailed overview of various radiation therapy techniques used in cancer treatment. This guide explains external and internal radiation methods, their mechanisms, uses, and important considerations for effective and safe cancer management. Learn how these advanced therapies can be tailored to individual patient needs, optimizing outcomes while minimizing side effects. Stay informed about the latest in radiation oncology for improved treatment strategies.
Radiation therapy is a cornerstone in the fight against cancer, offering targeted treatment options that can effectively destroy malignant cells while preserving surrounding healthy tissue. As a critical component in oncology, understanding the different types of radiation therapy available helps patients and clinicians make informed choices tailored to specific cancers and individual health conditions. In this comprehensive guide, we delve into detailed descriptions of external and internal radiation therapies, their mechanisms, applications, and factors influencing treatment decisions.
External Beam Radiation Therapy (EBRT)
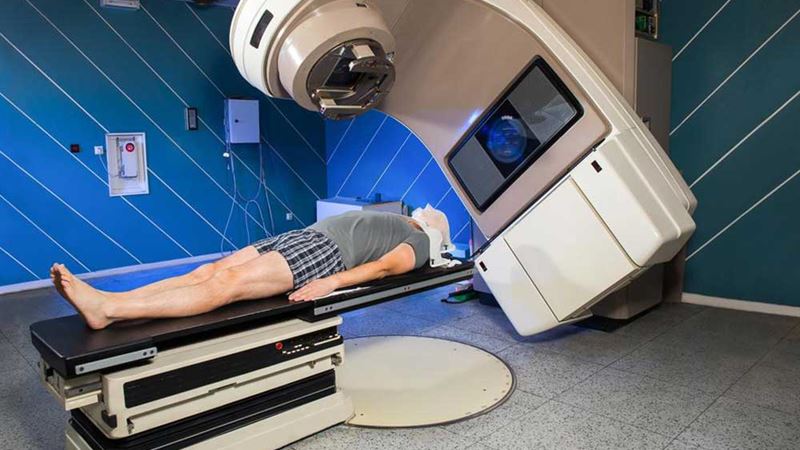
External beam radiation therapy, often abbreviated as EBRT, is a highly localized treatment modality designed to target specific cancerous areas within the body. This technique utilizes focused radiation beams generated by sophisticated machines called linear accelerators, which are capable of delivering precise doses of radiation directly to the tumor site, sparing adjacent normal tissues as much as possible. The radiation beams can consist of various particles, including photons (X-rays), electrons, or protons, chosen based on the type and location of the cancer.
During an EBRT session, the patient lies on a treatment table, and the machine aligns the radiation beam to the exact location of the tumor. The process is generally painless, but the procedure may involve multiple sessions over several days or weeks to achieve optimal therapeutic effects. The intensity, angle, and duration of radiation are meticulously planned using imaging techniques such as CT scans, MRI, or PET scans to ensure precision and safety.
Within external beam radiation therapy, several advanced techniques have been developed to maximize tumor targeting while minimizing side effects:
- 3-D conformal radiation therapy: Uses 3D imaging to shape the radiation beams closely matching the tumor's shape.
- Image-guided radiation therapy (IGRT): Incorporates real-time imaging during treatment to improve accuracy.
- Stereotactic radiosurgery and stereotactic body radiation therapy (SBRT): Deliver high doses of radiation in fewer sessions with extreme precision, often used for small, well-defined tumors.
- Intensity-modulated radiation therapy (IMRT): Modulates the radiation beam’s intensity to conform even more precisely to the tumor shape.
- Tomotherapy: Combines CT imaging with radiation delivery for highly targeted treatment.
The versatility of EBRT makes it suitable for treating a wide range of cancers, including brain, lung, breast, prostate, and more. Its ability to focus radiation on specific areas helps minimize damage to healthy tissue, but the risk of side effects—such as skin irritation, fatigue, and localized tissue damage—requires careful management and supervision by experienced radiation oncologists.
Internal Radiation Therapy (Brachytherapy and Systemic Therapy)
Unlike external radiation, internal radiation therapy involves placing radioactive materials directly inside or very close to the cancerous tissues. This allows for delivering high doses of radiation directly to the tumor with minimal impact on the rest of the body. Internal radiation therapy can be classified into two main categories: systemic therapy and brachytherapy.
Systemic Radiation Therapy
In systemic therapy, radioactive substances such as liquids (radiopharmaceuticals) are introduced into the bloodstream, where they travel throughout the body and selectively accumulate in cancer cells. This form of therapy is commonly used in treating thyroid cancer, neuroendocrine tumors (GEP-NET), and certain advanced prostate cancers. For example, radioactive iodine is a well-known systemic agent used for thyroid malignancies, effectively destroying cancerous thyroid tissue while sparing most healthy tissue.
Systemic radiation therapy offers the advantage of treating widespread disease that cannot be confined to a specific location. The radioactive compounds emit radiation as they decay, targeting cancer cells from within and improving treatment effectiveness for certain tumor types.
Brachytherapy (Solid Source Internal Radiation)
Brachytherapy involves placing radioactive sources directly into or near the tumor through small applicators or implants. This procedure can be performed using various forms, such as wires, pellets, or seeds, depending on the specific treatment plan. Brachytherapy is especially effective for cancers of the cervix, prostate, breast, eye, head, and neck areas.
For example, in prostate cancer, radioactive seeds are implanted into the prostate tissue, delivering high radiation doses directly to the tumor while reducing exposure to surrounding organs like the bladder and rectum. Similarly, in cervical cancer, radioactive applicators are used to target tumors with high precision.
This form of internal radiation is valuable because it minimizes collateral damage and allows for higher localized doses of radiation, leading to potentially better tumor control. However, managing the placement of radioactive materials and minimizing risk to healthcare workers require specialized training and precautions.
Deciding on the Appropriate Radiation Therapy
Selection of the optimal radiation treatment depends on multiple clinical and patient-specific factors. Healthcare professionals evaluate each case meticulously to determine the most effective approach, considering the following elements:
- Tumor size and volume: Larger or more invasive tumors may require different strategies compared to smaller, localized ones.
- Cancer type and histology: Different cancers react differently to specific radiation modalities.
- Location of the tumor: Accessibility and proximity to vital organs influence the choice of therapy.
- Sensitivity of surrounding tissues: Ensuring normal tissues are protected to prevent undue side effects.
- Patient’s overall health and medical history: Age, comorbidities, and previous treatments affect treatment planning.
- Patient preferences and lifestyle considerations: Quality of life and convenience are also important factors.
Because radiation therapy may have side effects, including fatigue, skin reactions, and tissue fibrosis, it is vital that patients undergo these treatments under strict medical supervision. The treatment plan is tailored to maximize efficacy while minimizing adverse effects, with continuous monitoring throughout the course of therapy.
In conclusion, radiation therapy encompasses a broad spectrum of techniques designed to target and eradicate cancer cells effectively. Advances in technology continue to improve precision, reduce side effects, and expand treatment options, giving hope to many patients battling cancers worldwide. Proper selection and management of these therapies can significantly impact treatment outcomes and quality of life for cancer patients.
