Comprehensive Guide to Rheumatoid Arthritis: Causes, Symptoms, and Effective Management
This comprehensive article explores rheumatoid arthritis, covering its causes, symptoms, progression stages, and various management strategies including medication, surgery, lifestyle, and diet. Learn how early intervention and holistic care can improve quality of life for those affected by RA.
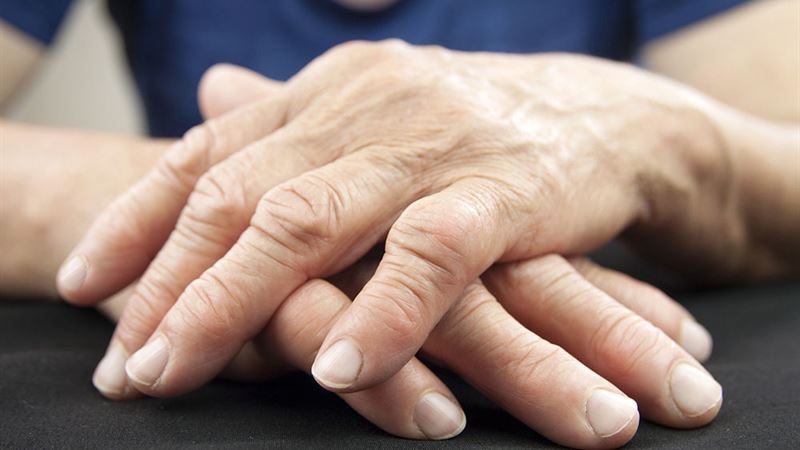
Rheumatoid arthritis (RA) is a chronic autoimmune disorder that primarily affects the joints but can also impact other organs and systems throughout the body. This complex disease involves the immune system mistakenly attacking the body's own tissues, leading to inflammation, pain, swelling, and potential joint destruction if left untreated. Understanding the root causes, recognizing the symptoms early, and exploring various management strategies are crucial steps in controlling this condition and maintaining a good quality of life. Throughout this comprehensive article, we will delve into the causes of RA, its symptoms, the stages of disease progression, and the most effective treatment options available today, including medications, lifestyle adjustments, and dietary recommendations.
**Etiology and Risk Factors of Rheumatoid Arthritis**
Rheumatoid arthritis results from an interplay of genetic, hormonal, environmental, and lifestyle factors. Individuals with a family history of RA are at higher risk, indicating a genetic predisposition. Specific gene variants, such as those in the HLA-DR4 gene, have been linked to increased susceptibility. Moreover, hormonal influences, especially in women, suggest that hormonal imbalances might modulate immune responses, which is why RA is more prevalent among females, particularly during childbearing years.
Environmental triggers also play a significant role. Exposure to certain infectious agents like bacteria and viruses may initiate immune system dysregulation. Additionally, environmental toxins, pollutants, and cigarette smoke are known to increase the risk of developing RA.
Other modifiable risk factors include:
Rheumatoid arthritis results from an interplay of genetic, hormonal, environmental, and lifestyle factors. Individuals with a family history of RA are at higher risk, indicating a genetic predisposition. Specific gene variants, such as those in the HLA-DR4 gene, have been linked to increased susceptibility. Moreover, hormonal influences, especially in women, suggest that hormonal imbalances might modulate immune responses, which is why RA is more prevalent among females, particularly during childbearing years.
Environmental triggers also play a significant role. Exposure to certain infectious agents like bacteria and viruses may initiate immune system dysregulation. Additionally, environmental toxins, pollutants, and cigarette smoke are known to increase the risk of developing RA.
Other modifiable risk factors include:
- Obesity and excess body weight, which can exacerbate joint stress and inflammation
- Physical or emotional trauma that may set off autoimmune responses
- Exposure to environmental toxins such as silica or industrial chemicals
- Lifestyle factors like smoking and sedentary habits
**Recognizing the Symptoms of Rheumatoid Arthritis**
The hallmark of RA is joint inflammation, which manifests through a variety of symptoms. Early signs often include persistent fatigue, mild fever, and generalized discomfort, but the primary focus remains on joint health.
Typical symptoms include:
The hallmark of RA is joint inflammation, which manifests through a variety of symptoms. Early signs often include persistent fatigue, mild fever, and generalized discomfort, but the primary focus remains on joint health.
Typical symptoms include:
- Morning stiffness lasting more than an hour, often improving with activity
- Swelling, tenderness, and warmth around the affected joints
- Symmetrical joint involvement, commonly affecting fingers, wrists, knees, ankles, and sometimes elbows and shoulders
- Limited range of motion and weakened grip strength
- Persistent pain that can fluctuate over time
Autoimmune activity can also extend beyond joints, affecting multiple organs and systems, leading to various systemic symptoms:
- Eye issues such as dryness, redness, sensitivity to light, or even vision disturbances due to inflammation
- Skin lumps called rheumatoid nodules that usually develop over pressure points like elbows or knuckles
- Shortness of breath caused by inflammation in lung tissues or pleura
- Nerve compression resulting in numbness or tingling sensations
- Anemia resulting from chronic inflammation affecting blood cell production
**Progression and Stages of Rheumatoid Arthritis**
Rheumatoid arthritis advances through distinct stages, each characterized by increasing damage to joints and surrounding tissues. Recognizing these stages helps in early intervention and tailored treatment planning.
**Stage 1: Preclinical or Early Stage**
In the initial phase, patients often experience joint pain, mild stiffness, and swelling but without detectable bone or cartilage damage. Inflammation is localized and may fluctuate.
**Stage 2: Inflammatory Stage**
Persistent inflammation leads to synovial hypertrophy—the thickening of the joint lining—potentially damaging cartilage. Symptoms intensify, and joint swelling becomes more pronounced.
**Stage 3: Destructive Stage**
This phase involves significant cartilage erosion and early bone damage. Symptoms are severe, with increased pain, swelling, muscle weakness, and decreased mobility. Irreversible joint changes may begin to occur.
**Stage 4: End-stage or Deformity Stage**
In advanced RA, joint destruction is complete, leading to deformities and loss of function. Bones may fuse (ankylosis), resulting in chronic disability. Damage is permanent, often necessitating surgical intervention.
**Treatment Strategies for Rheumatoid Arthritis**
Managing RA requires a multipronged approach aimed at controlling inflammation, preventing joint destruction, and improving quality of life.
**1. Pharmacological Treatments**
Medications are the cornerstone of RA management. These include:
Rheumatoid arthritis advances through distinct stages, each characterized by increasing damage to joints and surrounding tissues. Recognizing these stages helps in early intervention and tailored treatment planning.
**Stage 1: Preclinical or Early Stage**
In the initial phase, patients often experience joint pain, mild stiffness, and swelling but without detectable bone or cartilage damage. Inflammation is localized and may fluctuate.
**Stage 2: Inflammatory Stage**
Persistent inflammation leads to synovial hypertrophy—the thickening of the joint lining—potentially damaging cartilage. Symptoms intensify, and joint swelling becomes more pronounced.
**Stage 3: Destructive Stage**
This phase involves significant cartilage erosion and early bone damage. Symptoms are severe, with increased pain, swelling, muscle weakness, and decreased mobility. Irreversible joint changes may begin to occur.
**Stage 4: End-stage or Deformity Stage**
In advanced RA, joint destruction is complete, leading to deformities and loss of function. Bones may fuse (ankylosis), resulting in chronic disability. Damage is permanent, often necessitating surgical intervention.
**Treatment Strategies for Rheumatoid Arthritis**
Managing RA requires a multipronged approach aimed at controlling inflammation, preventing joint destruction, and improving quality of life.
**1. Pharmacological Treatments**
Medications are the cornerstone of RA management. These include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs): To reduce pain and inflammation
- Corticosteroids: For rapid control of inflammation, typically used short-term due to side effects
- Disease-modifying antirheumatic drugs (DMARDs): Such as methotrexate, sulfasalazine, and leflunomide, which slow disease progression
- Biologic agents: Targeted therapies like TNF inhibitors (etanercept, infliximab), interleukin inhibitors, and others that modulate immune activity
**2. Surgical Interventions**
In cases where joint damage is severe and unresponsive to medication, surgery may be necessary. Common procedures include joint joint replacement surgeries (arthroplasty) for hips, knees, elbows, wrists, and shoulders, aiming to restore mobility and reduce pain.
**3. Lifestyle Modifications**
Adopting healthy habits can significantly improve disease outcomes:
- Regular low-impact exercise to strengthen muscles and maintain joint flexibility
- Weight management to reduce joint strain
- Adequate rest and stress management strategies
- Physical therapy to improve joint function and reduce stiffness
- Avoiding activities that exacerbate symptoms
**Dietary Recommendations for RA Management**
Nutrition plays a vital role in managing inflammation associated with RA. Foods rich in antioxidants and omega-3 fatty acids have proven beneficial.
**Top Anti-inflammatory Foods:**
- ***Fatty Fish:*** Rich in omega-3 fatty acids, which suppress inflammatory pathways. Examples include salmon, mackerel, sardines, and albacore tuna.
- ***Colorful Fruits and Vegetables:*** Blueberries, strawberries, cherries, spinach, kale, and broccoli contain antioxidants that combat free radicals, reducing inflammation.
- ***Nuts and Seeds:*** Walnuts, flaxseeds, and chia seeds provide healthy fats, protein, and anti-inflammatory compounds.
- ***Legumes:*** Beans, lentils, and chickpeas offer fiber, antioxidants, and essential minerals that support joint health.
- Processed foods high in sugars and trans fats
- Excessive salt, which can promote inflammation
- Red meats with high saturated fat content
- Fried foods and refined carbs
Implementing these dietary changes alongside medical treatment can enhance overall health and reduce disease severity. Always consult with healthcare providers for personalized advice.
Note: This information serves educational purposes only. Always seek professional medical guidance for diagnosis and treatment of rheumatoid arthritis or any other health condition.
