Comprehensive Strategies and Medications for Effective Rheumatoid Arthritis Management
Discover comprehensive management strategies for rheumatoid arthritis, including physical and occupational therapies, advanced surgical options, and effective medications like biologics and corticosteroids. Learn how personalized treatment plans and lifestyle adjustments can help manage symptoms, preserve joint function, and improve quality of life in individuals living with this chronic condition. Expert guidance and early intervention are crucial for optimal outcomes.
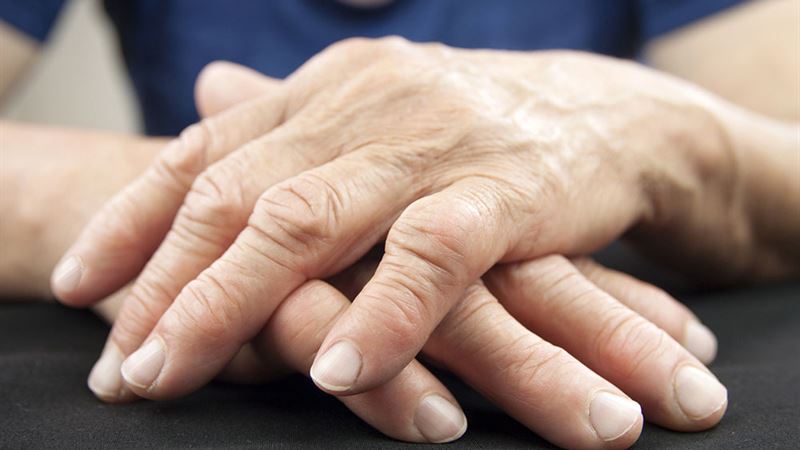
- Physical Therapy Approaches
Maintaining mobility and reducing joint stiffness are essential components of managing rheumatoid arthritis. Physical therapy employs tailored exercises, manual techniques, and movement strategies designed to strengthen muscles, enhance joint flexibility, and alleviate discomfort. Collaborating with a trained physical therapist ensures that exercises are appropriate for individual capabilities and disease progression. Regular sessions can prevent joint deterioration, improve posture, and boost overall physical function, enabling patients to maintain independence and improve quality of life. - Occupational Therapy Interventions
Everyday tasks such as dressing, cooking, and personal hygiene often become challenges due to persistent pain, swelling, and joint deformities. Occupational therapists provide customized solutions to mitigate these difficulties. They recommend assistive devices like ergonomic tools, adaptive equipment, and modifications to the home environment. Such interventions help patients conserve energy, reduce strain, and perform daily activities more comfortably, thereby maintaining autonomy and reducing frustration associated with rheumatoid arthritis.
When conservative therapies fail to manage symptoms or prevent joint damage, surgical interventions may be necessary. Surgery aims to repair or replace severely damaged joints, correct deformities, and alleviate persistent pain. Common procedures include joint replacement (arthroplasty), synovectomy (removal of inflamed synovial tissue), and joint fusion. While these surgeries can significantly improve functionality and comfort, they are considered final options after exhausting non-invasive options. A thorough evaluation by an orthopedic specialist helps determine the most suitable surgical approach based on the individual's condition and overall health.
Medications for Rheumatoid Arthritis
Various pharmaceutical treatments are vital in controlling inflammation, preventing joint destruction, and managing symptoms. It’s important to work closely with a healthcare provider to find the most effective medication plan tailored to your disease severity and personal health profile. Some of the most commonly prescribed drugs include:
- H.P. Acthar® (Corticotropin)
This hormone-based treatment is used to reduce inflammation and symptom severity. While it effectively relieves pain and swelling, it does not cure rheumatoid arthritis. It’s typically reserved for cases where other medications have failed and is administered under strict medical supervision. - CUPRIMINE® (Mitomycin)
Used in severe, refractory rheumatoid cases, this potent immunosuppressive drug helps slow disease progression. Due to its strength and potential side effects, it is usually not recommended for juvenile rheumatoid arthritis. Regular monitoring is essential during therapy. - Remicade® (Infliximab)
As a biological agent, Remicade inhibits specific inflammatory pathways by targeting tumor necrosis factor-alpha (TNF-α). It is often prescribed when traditional disease-modifying drugs are ineffective. Infusion sessions are typically scheduled through healthcare providers. - Humira® (Adalimumab)
This TNF inhibitor reduces inflammation and joint damage by blocking the actions of inflammatory cytokines. Given its immunosuppressive effects, patients are at increased risk of infections. Regular screenings and medical follow-ups are vital during treatment. - Enbrel® (Etanercept)
Similar to Humira, Enbrel is used to decrease inflammation by inhibiting TNF-α. It's also approved for treating plaque psoriasis in pediatric and adult patients aged 4 and above. Proper dosing and routine laboratory tests are essential to monitor side effects. - SIMPONI® (Golimumab)
Another TNF-blocking biologic, often used in conjunction with methotrexate, it helps control disease activity. Its immunosuppressive nature demands careful infection monitoring and regular medical assessments.
While medication forms the backbone of rheumatoid arthritis management, other strategies and lifestyle modifications contribute significantly to disease control. Patients should always seek professional medical advice before starting or changing treatments. Home remedies and self-care can complement medical therapy but should never replace professional guidance. Continual management, early intervention, and adherence to prescribed treatments enable individuals to lead active, fulfilling lives despite the condition. Remember, although rheumatoid arthritis cannot be cured completely, proactive management can substantially improve your health outcomes and quality of life. Stay vigilant, informed, and in close contact with your healthcare team to optimize your treatment plan.
