Comprehensive Guide to Eczematous Dermatitis: Types, Symptoms, and Treatments
This comprehensive article explores the various types of eczematous dermatitis, detailing their unique symptoms, causes, and treatment options. Understanding these differences helps in effective management and relief from discomfort. From atopic dermatitis to seborrheic eczema, learn how to identify and address each condition with professional advice and self-care tips.
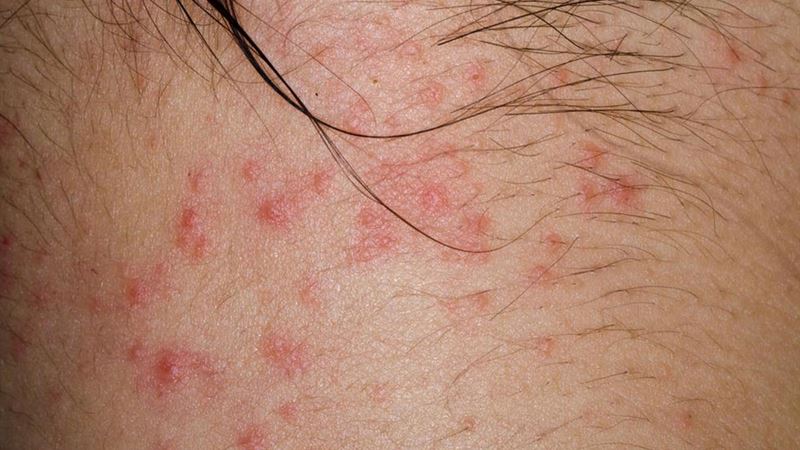
Eczema, also known as dermatitis, is a prevalent skin disorder characterized by inflammation, redness, itching, and sometimes weeping sores. This condition can significantly affect quality of life due to discomfort and aesthetic concerns. Understanding the various types of eczematous dermatitis, their distinct symptoms, causes, and treatment options is crucial for effective management. Eczema manifests differently depending on its type, severity, and underlying causes, making personalized diagnosis and treatment essential.
In this comprehensive guide, we'll explore each major form of eczema, including their specific symptoms, triggers, and available therapies. Whether you're a patient seeking more information or a caregiver aiming to understand the condition better, this article offers in-depth insights into one of dermatology's most common skin troubles.
What Is Eczematous Dermatitis?
Eczematous dermatitis refers to a group of inflammatory skin conditions presenting with similarities such as redness, swelling, and irritation. These skin reactions can appear anywhere on the body and are often associated with allergic reactions, irritant exposures, or genetic predispositions. The condition can be acute or chronic, with symptoms ranging from mild dryness to severe blistering and weeping sores.
While eczema can affect anyone, it is notably common among children and individuals with a history of allergies or asthma. The underlying pathology involves immune system dysregulation, skin barrier dysfunction, and environmental influences, all contributing to the development of various eczema subtypes.
Major Types of Eczematous Dermatitis
Understanding the different forms of eczema is fundamental to proper treatment and management. Each type has specific features, triggers, and affected areas, which can guide both patients and healthcare professionals in diagnosis and therapy planning.
Atopic Dermatitis
Atopic dermatitis (AD) is the most common form of eczema, especially in children. It is a chronic, inflammatory condition often linked to genetic factors and immune system abnormalities. AD frequently runs in families with histories of allergies, hay fever, and asthma. It typically presents with dry, itchy skin that tends to worsen periodical flare-ups.
Children might develop AD as early as within the first six months after birth. In infants, the rash commonly appears on the face, especially around the cheeks and chin. As children grow, the affected areas often shift to the insides of elbows, behind knees, and on the neck.
Although the precise cause of AD remains unclear, it is associated with a defective skin barrier making skin more susceptible to irritants and allergens. External triggers like soap, harsh detergents, certain fabrics, and environmental allergens can exacerbate symptoms. The immune system's hyper-reactivity leads to inflammation and the characteristic symptoms.
Symptoms of Atopic Dermatitis
- Persistent dry skin
- Scaly patches and rough skin
- Intense itching, which may worsen at night
- Redness and inflammation
- Cracks and fissures in the skin
- Rash appearing on flexural areas such as elbows and knees
- Weeping or oozing sores during flare-ups
Contact Dermatitis
Contact dermatitis occurs when the skin reacts directly to irritants or allergenic substances. It often affects areas in contact with the causative agents, such as the hands, wrists, or face. The reaction is usually localized and results in inflammation, redness, itching, and sometimes blistering.
It is subdivided into allergic contact dermatitis and irritant contact dermatitis. Allergic contact dermatitis is triggered by immune responses to specific substances like nickel, fragrances, or certain plants. Irritant contact dermatitis results from exposure to harsh chemicals or physical irritants.
Common Triggers
- Detergents and soaps
- Industrial chemicals and solvents
- Tobacco smoke and fumes
- Bleach, paints, and VOCs
- Wool, synthetic fibers, or certain clothing materials
- Skin care products containing alcohol or fragrances
- Certain foods like acidic or spicy items
- Plants like poison ivy or poison oak
Symptoms
- Area-specific redness and swelling
- Itching and burning sensations
- Presence of blisters or weeping sores
- Skin discoloration or hyperpigmentation after healing
Dyshidrotic Eczema
This form primarily affects the palms of the hands, soles of the feet, and sometimes the fingers and toes. It manifests with tiny, itchy blisters that can cause discomfort and cracking of the skin. Stress, exposure to moisture, and certain metals like nickel can increase susceptibility.
Symptoms
- Itchy, small blisters on the edges of fingers, palms, and soles
- Redness and swelling
- Cracking and scaling of the skin
- Pain or burning sensation during flare-ups
Hand Eczema
Often referred to as hand dermatitis, this is a prevalent form affecting a significant portion of the population. It results from frequent exposure to irritants such as detergents, chemicals, or environmental allergens. Both internal factors like genetics and external factors contribute to this chronic condition.
Hand eczema presents with redness, dryness, cracking, and sometimes blistering, impacting daily activities and work performance. Proper hygiene and protective measures are essential in management.
Symptoms
- Persistent itching and discomfort
- Dry, cracked skin on palms and fingers
- Redness and swelling
- Blisters or oozing sores during acute episodes
Neurodermatitis or Lichen Simplex Chronicus
This form is characterized by thickened, scaly patches resulting from repeated scratching or rubbing. Often associated with stress or psychological factors, neurodermatitis involves localized areas commonly on the neck, wrists, or scalp.
Symptoms
- Thickened, leathery patches
- Scaly or rough skin
- Persistent itching leading to repeated trauma
- Discoloration or hyperpigmentation
Nummular Eczema
Also called discoid eczema, this type features round or coin-shaped lesions that are intensely itchy. It can occur at any age and is often triggered by insect bites, dry skin, or skin inflammation. The lesions may ooze or crust as part of the healing process.
Symptoms
- Distinct round, coin-shaped patches
- Itching and discomfort
- Dry, scaly, or cracked skin
- Possible oozing or crusting
Seborrheic Dermatitis
This chronic, oily skin condition predominantly affects areas rich in sebaceous glands, such as the scalp, face, especially around the nose, and upper chest. It is characterized by flaky scales, redness, and sometimes dandruff in scalp areas. The underlying cause involves an overgrowth of yeast (Malassezia), hormonal influences, and genetic predisposition. Unlike allergic eczema, seborrheic dermatitis is driven by microbial imbalance and skin oil production.
Symptoms
- Persistent dandruff or flaky scalp
- Oily, red patches on the face or scalp
- Itching and discomfort
- Cradle cap in infants
Proper diagnosis of each eczema type involves clinical examination, patient history, and sometimes skin tests to identify triggers. Treatment options include topical corticosteroids, moisturizers, antihistamines, and lifestyle modifications to reduce exposure to irritants and allergens. In some cases, light therapy or systemic medications are necessary for severe cases.
Conclusion
Recognizing the different types of eczematous dermatitis is essential for effective management and relief. Each form has unique features, triggers, and treatment strategies. If you suspect you have eczema, consult a dermatologist for accurate diagnosis and personalized treatment plans. With proper care and lifestyle adjustments, managing eczema symptoms and improving skin health is achievable.
