Comprehensive Guide to Recognizing and Managing Dupuytren’s Contracture
This comprehensive article explores Dupuytren’s contracture, detailing its symptoms, risk factors, diagnostic procedures, and modern treatment options. Early detection and intervention are emphasized to prevent lasting hand impairment. The guide covers minimally invasive techniques like needling and enzyme injections, along with surgical solutions when necessary. Understanding the disease process helps individuals seek timely care, maintaining hand mobility and quality of life. Aimed at patients and healthcare providers alike, this detailed overview enhances awareness and management strategies for Dupuytren’s contracture.
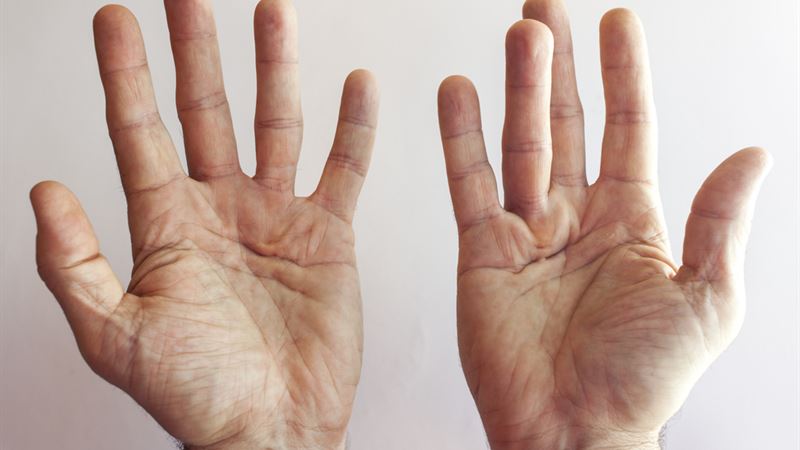
Dupuytren’s contracture is a condition where the tissues beneath the skin of the palm become thickened and contracted, leading to permanent bending of the fingers. Understanding how this disease manifests and progresses is essential for early intervention and effective management. The primary tissues affected are known as the fascia, a layer of connective tissue that runs just beneath the skin and connects to the fingers via fibrous cords. When these cords tighten, they pull the fingers into a bent position, impairing hand function and mobility.
Visual illustrations of Dupuytren’s contracture show characteristic deformities of the palm, with nodules and cords that cause the fingers to curl. The affected fascia appears inflamed microscopically, showing signs of tissue repair attempts similar to those observed in chronic injuries or certain cancers. This inflammatory process stimulates excessive collagen production, leading to the formation of thickened bands that shrink over time, pulling the fingers inward.
- The key pathology involves the fascia—the connective tissue that supports the skin and fingers. As collagen fibers within this tissue alter and proliferate abnormally, they form hardened cords that contract, restricting finger extension. This leads to the characteristic flexion deformity seen in patients.
- Inflammation and tissue remodeling characterize the early stages, where microscopic examination may reveal signs of chronic inflammation often associated with ongoing tissue repair or injury. Recognizing these signs can help with early diagnosis and intervention.
Understanding the symptoms and risk factors associated with Dupuytren’s contracture is crucial for timely diagnosis. If you notice certain signs, seeing a healthcare professional promptly can prevent further deterioration of hand function.
Identifying Early Signs of Dupuytren’s Contracture
- Medical consultation is the first step. Sharing personal and family medical history can shed light on potential genetic or acquired risk factors. For example, individuals taking certain medications for epilepsy or those with diabetes have a higher susceptibility. A positive family history significantly increases the risk, highlighting the hereditary nature of the disease.
- Lifestyle factors such as smoking and alcohol consumption are also linked to the development and progression of Dupuytren’s contracture. Certain comorbidities, like epilepsy or liver disease, further influence risk profiles.
- The initial presentation often involves a small lump forming on the palm, usually near the base of the fingers. This lump resembles a scar or thickened tissue and gradually extends towards the fingers. As the disease advances, patients notice the affected fingers pulled inward, resulting in a bent or flexed position—most commonly affecting the ring and pinky fingers. Pain may be minimal or absent, but the deformity progressively worsens, impairing hand function and gripping ability.
- The bilateral nature of the disease means both hands may be affected, but one hand often shows more severe symptoms. Early detection is vital because if left untreated, the condition can limit finger mobility permanently, significantly impacting daily activities.
Diagnosis of Dupuytren’s Contracture
- Diagnosis largely depends on a clinical examination. Experienced physicians can identify the characteristic nodules and cords by visual inspection and palpation. In most cases, no additional tests are required.
- The doctor may have the patient place their hand flat on a smooth surface to assess the extent of finger flexion. The inability to fully extend fingers or the presence of palpable thickened cords confirms the diagnosis.
Available Treatment Options for Dupuytren’s Contracture
Management strategies depend on the severity and progression rate of the disease. Mild cases may be monitored for progression, while more advanced cases require targeted interventions. The goal of treatment is to break or remove the fibrous cords that restrict finger movement, restoring hand function. The options include:
- Needling Therapy – This minimally invasive technique involves inserting a fine needle beneath the skin to mechanically sever the contracted cords. It is performed under local anesthesia, often on multiple fingers, with minimal discomfort and recovery time. Multiple sessions may be necessary as recurrence can happen.
- Enzymatic Collagenase Injection – Certain enzymes are injected directly into the thickened cords to weaken their collagen fibers. After enzyme action, the physician manipulates the fingers to break the cords, allowing the fingers to straighten. This outpatient procedure is effective and has a comparable success rate to needling.
- Surgical Intervention – When conservative methods fail or in severe cases, surgical removal of the diseased tissue—known as fasciectomy—is performed. Surgery offers a permanent solution by excising the problematic fascia. While recovery takes longer and involves postoperative therapy, the results are often durable, significantly improving hand function.
In conclusion, early recognition of symptoms and timely treatment of Dupuytren’s contracture are crucial for preserving hand mobility. Advances in minimally invasive techniques have made management more effective and less burdensome for patients. If you notice early signs such as lumps or finger deformity, consult a hand specialist for proper evaluation and personalized treatment planning.
