Understanding Hyperhidrosis: Symptoms, Causes, and Management Strategies
Hyperhidrosis is a condition characterized by excessive sweating that exceeds normal needs, often leading to skin problems, social anxiety, and emotional distress. This comprehensive guide explains the symptoms, underlying causes—including genetic, psychological, metabolic, and external factors—and discusses available treatment options. Recognizing the signs and understanding the triggers can help individuals manage the condition more effectively, improving their quality of life and social interactions. Seeking medical advice is crucial for proper diagnosis and tailored treatment strategies to control hyperhidrosis symptoms.
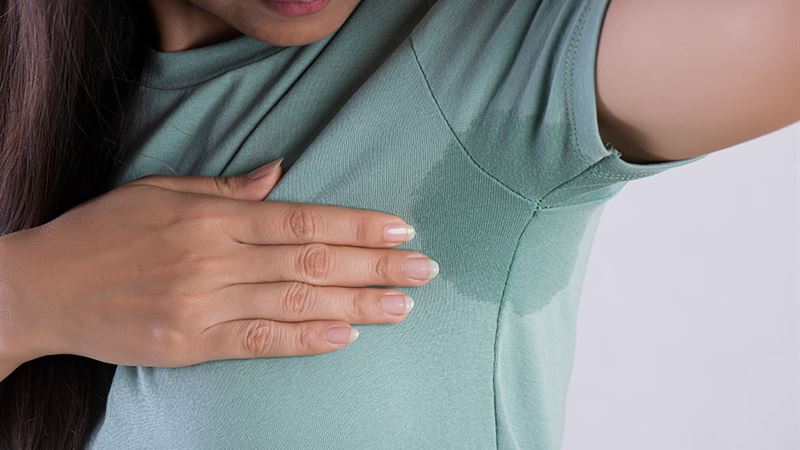
- Persistent Body Odor - One of the most noticeable signs of hyperhidrosis is an unpleasant body odor resulting from sweat interacting with bacteria on the skin. Sweat itself is odorless; however, bacterial activity can produce foul smells, which often cause embarrassment and social discomfort. Managing hygiene and using specialized antiperspirants are common strategies to mitigate this symptom.
- Various Skin Issues - Excessive sweating can lead to a constellation of skin problems. Bacterial infections, skin cracks, wrinkles, and discoloration are prevalent. Maceration, the softening and whitening of skin tissues, often occurs on the feet's soles due to prolonged moisture exposure. These skin issues can sometimes require medical attention, especially if infections develop or if skin damage becomes chronic.
- Inflammation and Itching - Many individuals with hyperhidrosis report increased skin irritation, persistent itching, and inflammation. The constant moisture can break down the skin’s natural barrier, making it more susceptible to irritants and infections. Treating these symptoms involves both managing sweating and maintaining skin health through topical treatments and hygiene practices.
- Social and Emotional Challenges - Visible sweating and related skin changes can lead to significant social anxiety and embarrassment. People affected may feel reluctant to engage in close physical interactions or participate in social gatherings, which can result in feelings of isolation and depression. Addressing the emotional impact is an integral part of comprehensive treatment plans.
Primary Causes of Hyperhidrosis
The main mechanism behind hyperhidrosis is the hyperactivity of sweat glands, which results in excessive perspiration. The condition can be triggered or aggravated by various factors, including psychological, genetic, metabolic, environmental, and health-related influences:
- Psychological Factors - Anxiety, mental stress, and nervousness can stimulate the sympathetic nervous system, leading to increased activity of sweat glands. Emotional responses are often closely linked to episodes of excessive sweating, especially in social settings.
- Genetic Predisposition - A family history often indicates a hereditary component. Individuals with relatives suffering from hyperhidrosis are at higher risk of developing similar symptoms, suggesting a genetic link that influences sweat gland regulation.
- Metabolic Conditions - Certain systemic diseases significantly contribute to hyperhidrosis. Conditions like diabetes mellitus, gout, thyroid disorders, and diseases of the pituitary gland can disrupt normal metabolic and hormonal balances, leading to overactive sweat response.
- Environmental and External Triggers - External stimuli such as physical activity, hot weather, high humidity, consumption of alcohol, or spicy foods can provoke excessive sweating episodes. These factors may act as triggers in individuals already predisposed to the condition.
- Associated Diseases and Health Issues - Heart diseases, certain cancers, respiratory conditions, and side effects from specific medications have been linked to secondary hyperhidrosis. Identifying and managing these underlying conditions are vital components of treatment.
Understanding the multifaceted nature of hyperhidrosis enables better management of the condition. A thorough evaluation by healthcare professionals can help differentiate between primary hyperhidrosis (a standalone disorder) and secondary hyperhidrosis (linked to other medical issues). Appropriate diagnoses often involve physical examinations, history assessments, and sometimes laboratory tests. Therapeutic options vary from topical treatments, medications, and lifestyle modifications to advanced interventions like Botox injections or even surgical procedures in severe cases.
