Comprehensive Guide to Managing Psoriatic Arthritis and Its Most Effective Treatment Strategies
This comprehensive guide explores various effective treatments for psoriatic arthritis, emphasizing lifestyle changes, medication options, and advanced therapies. It aims to empower patients with knowledge to manage their condition better, prevent joint damage, and maintain a good quality of life through personalized treatment strategies and ongoing medical support.
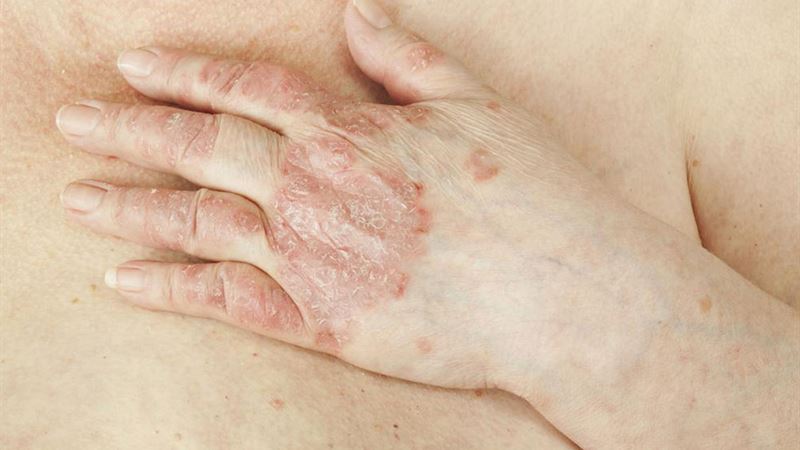
Living with psoriatic arthritis can significantly impact your daily life, causing persistent joint pain, stiffness, and inflammation. Fortunately, there are various treatment options designed to alleviate symptoms, improve mobility, and prevent irreversible joint damage. A combination of lifestyle modifications, medications, and supportive therapies forms the backbone of effective management. Understanding the most effective treatment possibilities empowers patients to make informed decisions and work closely with healthcare providers to craft personalized treatment plans.
One of the foundational approaches to managing psoriatic arthritis involves regular physical activity. Engaging in targeted exercises can help in reducing joint stiffness, maintaining or improving range of motion, and strengthening the muscles surrounding affected joints. It is advisable to consult with a physiotherapist or a trained healthcare professional who can develop a tailored exercise regimen suited to individual needs. Such routines are primarily aimed at enhancing joint function, reducing pain levels, and preventing further deterioration.
In addition to exercise, lifestyle adjustments and home remedies play a pivotal role. Applying cold packs or ice treatments over inflamed areas can effectively diminish swelling, reduce pain, and alleviate discomfort caused by inflammation. Adequate rest is crucial in allowing the body to recover and cope with symptoms. Managing stress is equally vital because psychological stress can exacerbate psoriatic symptoms and flare-ups. Incorporating relaxation techniques, mindfulness practices, or yoga can help in maintaining emotional equilibrium, which in turn benefits physical health.
Complementing physical and lifestyle interventions are several medications tailored to different severity levels and individual responses. Non-steroidal anti-inflammatory drugs (NSAIDs) are frequently prescribed during the early stages of the disease to alleviate pain and reduce inflammation. These medications are effective but should be used judiciously, as prolonged use might lead to gastrointestinal issues or other side effects. It is essential to follow medical advice regarding dosage and duration.
For more severe cases, corticosteroids may be prescribed. These potent anti-inflammatory agents can provide rapid symptom relief; however, their long-term use requires careful monitoring due to potential side effects, including skin thinning, weight gain, and osteoporosis. Doctors usually reserve corticosteroids for short-term use or flare-ups, adjusting the treatment plan based on patient response and any adverse reactions.
Beyond symptomatic relief, systemic medications are often employed to control disease progression and limit joint damage. One such drug is Cyclosporine, an immunosuppressant that effectively slows the advancement of psoriatic arthritis. While it offers significant benefits, it carries risks such as kidney toxicity, necessitating regular blood tests to monitor kidney function and drug levels. Other biologic agents and disease-modifying antirheumatic drugs (DMARDs) may also be prescribed, targeting specific immune pathways involved in the disease process and providing sustained control over symptoms.
Advanced therapeutic options, including biologics like TNF-alpha inhibitors, IL-17 inhibitors, and IL-12/23 inhibitors, have revolutionized treatment by offering targeted action and improved quality of life for many patients. These drugs are often considered when conventional therapies fail or when symptoms are particularly severe. They work by modulating immune responses to reduce inflammation and prevent joint destruction, significantly improving mobility and decreasing pain.
Moreover, ongoing research into new medications and combination therapies continues to expand the arsenal against psoriatic arthritis. It is crucial for patients to maintain regular follow-ups with their healthcare providers, undergo routine blood tests, and adjust treatment protocols as needed. Early diagnosis and integrated management are key to preventing long-term disability, improving overall health, and ensuring a better quality of life for those affected.
In summary, managing psoriatic arthritis requires a multifaceted approach that combines physical activity, lifestyle modifications, and pharmacotherapy. Patients should work closely with their healthcare team to develop a personalized treatment plan. With advancements in medicine, many individuals can achieve symptom control, preserve joint function, and lead active, fulfilling lives despite this chronic condition. Staying informed about new treatment options and adhering to prescribed therapies are essential steps toward effective disease management and improved health outcomes.
