Effective Strategies for Managing Psoriatic Arthritis: A Comprehensive Guide
Discover in-depth insights on psoriatic arthritis including its symptoms, causes, diagnostic methods, and a wide array of treatment options—both medical and natural. This comprehensive guide offers practical advice to effectively manage this autoimmune condition, improve quality of life, and maintain joint and skin health through lifestyle modifications and advanced therapies. Whether you're seeking conventional approaches or natural remedies, learn how to take proactive steps toward better health and disease control with expert-backed information and strategies.
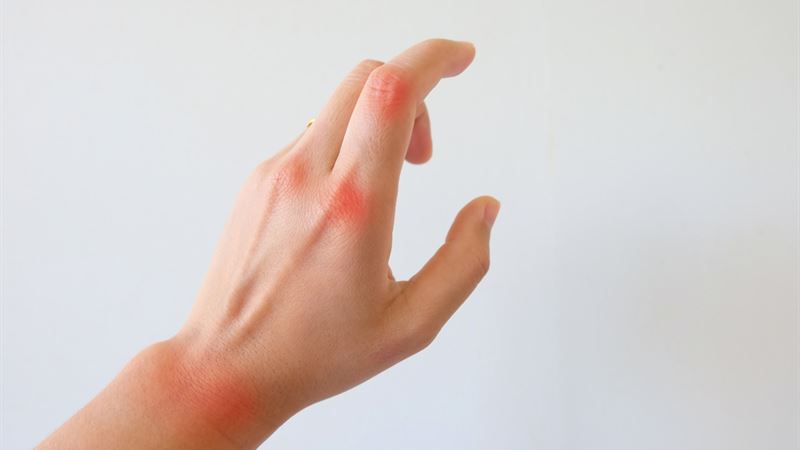
Psoriatic arthritis is a complex and often misunderstood autoimmune condition that affects a significant number of individuals worldwide. Its symptoms can be quite diverse and sometimes challenging to recognize early on, as they frequently resemble other forms of inflammatory joint diseases. Understanding the nuances of psoriatic arthritis—its symptoms, causes, diagnosis, and various treatment options—is essential for effective management and improved quality of life. This extensive guide delves into all these aspects, providing valuable insights and practical advice to those affected or concerned about this condition.
Psoriatic arthritis is a chronic inflammatory disease that primarily impacts the joints and skin, often manifesting in people who already have psoriasis. Its presentation can vary widely among individuals, making early diagnosis challenging. However, as the disease progresses, symptoms become more pronounced and recognizable. Recognizing the initial signs is crucial in managing the disease effectively. This guide aims to shed light on the key symptoms, underlying causes, diagnostic procedures, and the comprehensive range of treatment options—including traditional and natural remedies—that can help manage psoriatic arthritis effectively.
Understanding the Symptoms of Psoriatic Arthritis
The symptoms of psoriatic arthritis are diverse, affecting different joints and skin areas in varying degrees among patients. While some may experience mild discomfort, others may face severe pain and disability if not diagnosed and treated promptly. Here are some of the most common symptoms associated with psoriatic arthritis:
- Often described as looking like sausages, this characteristic swelling results from inflammation of the tendons and joints, causing pain, stiffness, and deformity if left unmanaged.
- Indented, pitted, or crumbling nails are hallmark signs. These nail alterations occur due to inflammation affecting the fingernails and toenails.
- Thickened, reddened, and scaly patches of skin—typical psoriasis—may worsen concurrently with joint inflammation, indicating disease activity.
- Joint Stiffness and Pain: Morning stiffness lasting more than an hour is common, along with persistent joint soreness, swelling, and reduced mobility.
- Enthesitis: Discomfort and tenderness at entheses—the sites where tendons and ligaments attach to bones—are distinctive features of psoriatic arthritis.
- Tiredness: Chronic fatigue is frequently reported, impacting daily functioning and overall wellbeing.
- Eye Problems: Symptoms such as soreness, irritation, blurred vision, or conjunctivitis may occur, requiring ophthalmological attention.
The Causes and Risk Factors of Psoriatic Arthritis
The exact cause of psoriatic arthritis remains elusive, but it’s believed to result from a combination of genetic, immune, and environmental factors. Individuals with psoriasis are at a higher risk of developing this form of arthritis, as their immune systems erroneously attack healthy cells in the skin and joints. Several phenomena contribute to disease onset:
- Genetic Predisposition: A family history of psoriasis or psoriatic arthritis increases susceptibility, with certain gene variants identified as risk factors.
- Autoimmune Response: An abnormal immune response leads the body to attack its own tissues, triggering inflammation in the joints and skin.
- Environmental Triggers: Factors such as infections, trauma, stress, or exposure to certain medications can precipitate disease flare-ups.
- Age and Gender: While psoriatic arthritis can occur at any age, it is more common in adults between 30 and 50 years old, with a slightly higher prevalence in males.
Diagnostic Approaches for Psoriatic Arthritis
Since symptoms can mimic other joint disorders, accurate diagnosis is essential for effective treatment. Doctors typically rely on a combination of clinical examination, patient history, and diagnostic tests, including:
- Physical Examination: Assessing joint swelling, tenderness, skin lesions, and nail health.
- Blood Tests: To rule out other conditions like rheumatoid arthritis, tests such as ESR, CRP, and rheumatoid factor are conducted.
- Imaging Studies: X-rays, MRI, or ultrasound help identify joint damage, inflammation, and bone erosion characteristic of psoriatic arthritis.
- Skin Biopsy: Confirming psoriasis or ruling out other skin conditions.
Conventional and Modern Treatment Options
Managing psoriatic arthritis involves a multifaceted approach tailored to the severity of symptoms, extent of joint damage, and overall health of the patient. Treatment aims to reduce inflammation, relieve pain, prevent joint deformity, and improve quality of life. Key treatment modalities include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These drugs—available over the counter or via prescription—help decrease pain, swelling, and stiffness. They can be administered orally or topically, depending on the affected areas.
- Topical Treatments: Corticosteroid creams, ointments, or medicated shampoos soothe skin lesions, reduce redness, and alleviate itching.
- Corticosteroids: Injectable or oral steroids are used to manage severe inflammation and pain during flare-ups, but long-term use requires careful supervision due to potential side effects.
- DMARDs (Disease-Modifying Antirheumatic Drugs): These drugs—such as methotrexate or ciclosporin—act on the immune system to slow disease progression and prevent joint damage.
- Biologic Agents: Targeted therapies that inhibit specific immune pathways, such as TNF inhibitors, offer relief for moderate to severe cases resistant to conventional treatments.
- Light Therapy: Controlled exposure to ultraviolet light can reduce skin psoriasis severity, often used alongside other therapies under medical supervision.
Natural and Complementary Therapies
In addition to pharmaceutical options, many individuals seek natural remedies to support their treatment plan and reduce symptoms. While these methods should complement conventional therapies, they can enhance overall wellbeing when used appropriately:
- Dietary Adjustments: An anti-inflammatory diet rich in omega-3 fatty acids, fruits, vegetables, and whole grains can help diminish systemic inflammation. Limiting processed foods, sugar, and saturated fats is recommended.
- Stress Reduction Techniques: Since stress can exacerbate symptoms, practices like yoga, meditation, deep-breathing exercises, and engaging in hobbies are beneficial.
- Skincare Regimen: Keeping skin moisturized with organic, fragrance-free products helps reduce itchiness and prevent flare-ups. Wearing loose, breathable clothing minimizes skin irritation.
- Supplements and Herbal Remedies: Certain supplements like turmeric, omega-3 fatty acids, and supplements with anti-inflammatory properties may provide additional support. Always consult a healthcare provider before starting any supplement.
- Physical Activity: Low-impact exercises such as swimming, cycling, and walking maintain joint mobility and strengthen muscles, reducing stiffness and pain.
Living Well with Psoriatic Arthritis
Living with psoriatic arthritis requires ongoing management and lifestyle adjustments. Creating a supportive environment, maintaining regular medical consultations, and adhering to prescribed treatment plans are pivotal. Furthermore, engaging with support groups can provide emotional relief and practical advice from others experiencing similar challenges. Early intervention and consistent care significantly improve long-term outcomes, preventing joint deformities and enhancing overall quality of life.
Understanding the importance of a holistic approach, which includes medical, nutritional, and psychological strategies, empowers patients to take charge of their health and wellbeing. Remember, each individual’s experience is unique, and therefore, treatment plans should always be personalized in collaboration with healthcare professionals.
