Comprehensive Approaches to Managing and Treating Varicose Veins
Discover comprehensive strategies for treating varicose veins, including minimally invasive procedures and lifestyle changes. Learn how to manage symptoms, prevent progression, and improve vascular health through advanced treatments like sclerotherapy, laser therapy, and proper self-care practices. Early intervention can greatly reduce discomfort and prevent severe complications, ensuring better quality of life. This detailed guide offers insights into effective management options and practical tips for maintaining healthy veins, making it a valuable resource for those affected by varicose veins or seeking preventive measures.
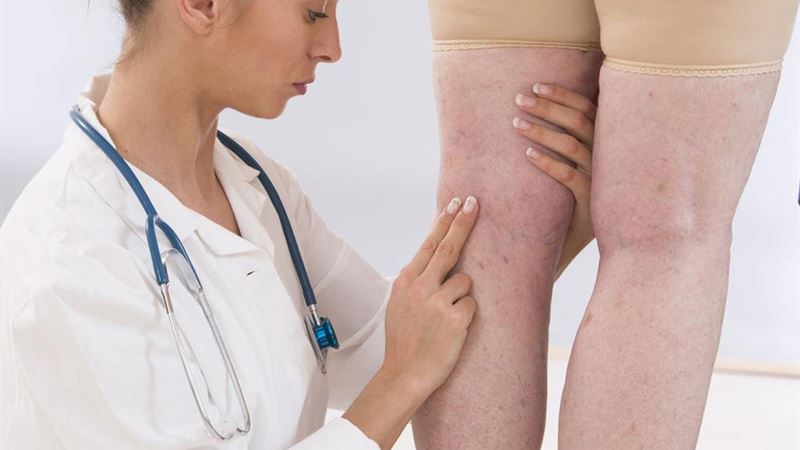
Varicose veins are a common vascular condition characterized by enlarged, twisted, and bulging veins that often appear on the legs and feet. While many individuals may experience minimal discomfort, others suffer from significant pain, swelling, skin discoloration, and, in severe cases, ulcers. Understanding the various causes, risk factors, and treatment options for varicose veins is essential for effective management and improved quality of life.
The development of varicose veins is influenced by multiple factors. Hormonal fluctuations are a significant contributor, especially in women. The use of combined oral contraceptives, hormonal changes during puberty, pregnancy, menopause, and the intake of estrogen and progesterone can weaken the walls and valves of veins, leading to blood pooling and vein expansion. These hormonal influences increase the susceptibility to vein dilation and varicose vein formation.
Pregnancy is a notable risk factor due to increased blood volume and hormonal alterations. During pregnancy, blood circulation is augmented to supply oxygen and nutrients to both mother and fetus, which increases pressure in the leg veins. This pressure causes veins to become enlarged and more prominent. Additionally, the enlarging uterus exerts pressure on the pelvic veins, impeding blood flow back to the heart. Many pregnant women experience varicose veins, particularly in the legs, and these often tend to regress within a few months postpartum. However, in some cases, they may persist or worsen without intervention.
Other significant contributors include prolonged standing or sitting for extended periods, which hampers proper venous return. Aging naturally causes vein walls and valves to weaken, fostering the development of varicose veins. Excess weight or obesity places additional pressure on leg veins, accelerating vein dilation and failure. Genetic predisposition also plays a crucial role; if a family member has varicose veins, the likelihood of developing them is higher.
Fortunately, multiple treatment modalities are available to address varicose veins effectively. The advances in minimally invasive procedures have revolutionized treatment, allowing patients to undergo therapy with reduced recovery times, less discomfort, and no need for prolonged hospital stays.
Below, we elaborate on the most recognized and effective treatment options for varicose veins:
- Sclerotherapy: This procedure involves injecting a special sclerosing solution directly into the affected veins. This solution causes the vein walls to collapse and stick together, leading to the eventual fading and disappearance of the veins within a few weeks. Sclerotherapy is generally painless and can be performed without anesthesia, making it suitable for outpatient settings.
- Foam Sclerotherapy: An enhanced version of traditional sclerotherapy, this technique employs a foam form of the sclerosant, allowing for treatment of larger veins. The foam displaces blood within the vein, improving contact with the vessel lining, and promoting rapid closure of the problematic vein.
- Vein Stripping and Ligation: Often performed as an outpatient procedure, this method involves tying off the affected vein (ligation) to prevent blood flow into the varicose vein, followed by removing the vein (stripping) through small incisions. This technique is effective for severe cases where other treatments are insufficient. Because the larger veins are responsible for blood return, removing a small superficial vein usually does not compromise circulation.
- Catheter-assisted Ablation: This minimally invasive technique uses a thin catheter inserted into the affected vein. Using heat from laser energy or radiofrequency waves, the vein is closed from within. The catheter is gradually withdrawn, and the heat causes the vein to collapse and seal shut, rerouting blood flow through healthier veins.
- Endoscopic Vein Surgery: Suitable for advanced cases, particularly those with skin ulcers or infected veins, this method involves inserting a tiny camera (endoscope) into the leg to visualize the affected veins. Surgeons then remove or seal the problematic veins through small incisions, providing an effective solution when other treatments are insufficient.
- Laser Surgery: Using concentrated laser beams directed onto the affected veins, this procedure gradually causes the veins to fade and disappear heat minimally or not at all with incisions, reducing discomfort and scarring. It is highly effective for both spider veins and larger varicose veins.
- Ambulatory Phlebectomy: This outpatient procedure involves making tiny punctures in the skin to remove superficial varicose veins. The area is numbed beforehand, and no stitches or scarring usually occur. It is an excellent choice for small to medium-sized varicose veins.
Beyond these medical interventions, lifestyle modifications can significantly ease symptoms and prevent progression:
- Regular Physical Activity: Engaging in consistent exercise improves blood circulation and strengthens leg muscles. Activities such as walking, cycling, swimming, yoga, and stretching facilitate the upward movement of blood, reducing pressure on veins.
- Proper Self-Care: Avoid wearing tight clothing around the waist, groin, or legs. Elevate your legs periodically to encourage blood flow back to the heart, especially after long periods of standing or sitting. Maintaining a healthy weight also lessens the strain on leg veins.
- Use of Compression Stockings: Specialized compression stockings provide gentle squeezing of the leg muscles, assisting veins in blood return. Wearing compression stockings regularly can alleviate symptoms and prevent vein worsening. They are available in various compression levels tailored to individual needs.
- Diet and Nutrition: A balanced diet rich in fiber and potassium supports vascular health. Foods high in fiber—like oats, whole grains, beans, vegetables, and fruits—aid digestion and reduce straining during bowel movements, which can increase venous pressure. Incorporate potassium-rich foods such as bananas, sweet potatoes, spinach, and yogurt to prevent water retention and reduce swelling.
- Flavonoid-Rich Foods: Consuming fruits and vegetables high in flavonoids, such as apples, onions, spinach, and cocoa, helps maintain vein elasticity and function, aiding in the management of varicose veins.
Early detection and prompt intervention are crucial. Recognizing symptoms like visible enlarged veins, leg heaviness, aching, swelling, and skin changes allows for timely treatment. Consulting with a vascular specialist ensures personalized care and the selection of the most suitable treatment approach. Managing risk factors through lifestyle modifications is an effective way to prevent or reduce the severity of varicose veins.
In conclusion, varicose veins can significantly impact an individual's comfort and mobility, but with the wide array of modern treatment options, relief and improvement are achievable. Combining medical procedures with healthy habits can enhance venous health, reduce symptoms, and prevent future complications. If you notice early signs of varicose veins, seek professional advice promptly to explore the best treatment pathway tailored to your needs.
