Comprehensive Guide to Toenail Fungus: Recognizing Symptoms and Effective Treatment Options
This comprehensive guide explores toenail fungus symptoms, risk factors, and an array of treatment options including medications, topical agents, surgical procedures, and home remedies. Early diagnosis is key to effective management, preventing complications and promoting healthy nail growth. Learn how to protect your feet and choose the right treatment plan for lasting results. Expert advice emphasizes hygiene, lifestyle modifications, and medical interventions to effectively eliminate fungal infections and restore nail health. Prevention and prompt care are crucial for maintaining healthy, fungus-free nails.
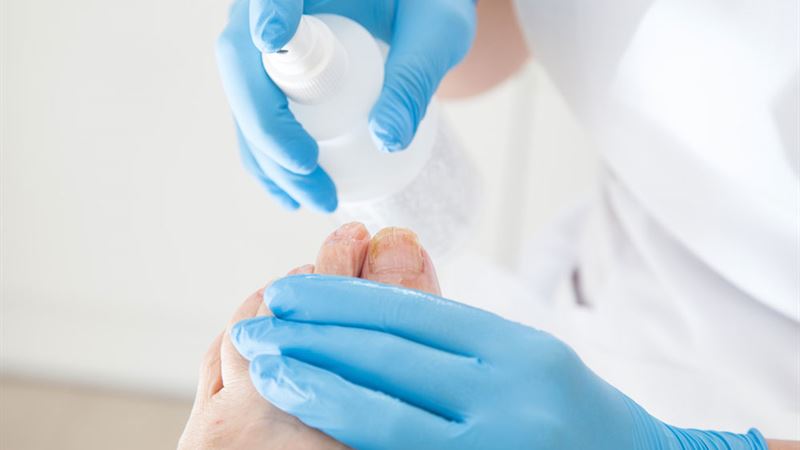
Understanding Toenail Fungus: Symptoms and Prevention
Toenail fungus, medically known as onychomycosis, is a common condition affecting many individuals worldwide. While it predominantly targets toenails, fingernails can also be affected. This fungal infection occurs when abnormal fungi invade the nail bed, leading to various undesirable changes in the nail's appearance and structure. Recognizing the early signs of toenail fungus and understanding the available treatment options are crucial steps in preventing its progression and avoiding complications.
Most toenail infections are caused by dermatophytes, but yeasts and molds can also be culprits. Factors such as humid environments, poor foot hygiene, wearing tight or damp shoes, and having minor nail injuries can increase susceptibility. People with compromised immune systems, diabetes, or circulatory issues need to be especially vigilant because fungal infections can become more severe or persistent in these populations.
Common symptoms of toenail fungus include thickened nails, discoloration ranging from white to yellowish-brown, brittleness, crumbling edges, and distorted nail shapes. Debris may accumulate underneath the nail, further darkening its appearance. Often, the infection is painless initially, but as it advances, discomfort, unpleasant odors, or even pain can occur, especially if the infection spreads or causes nail separation from the nail bed.
Preventing toenail fungus involves maintaining good foot hygiene, keeping feet dry, wearing breathable footwear, and avoiding walking barefoot in communal areas such as gyms or swimming pools. Regularly disinfecting shoes and avoiding sharing nail tools can also diminish risk.
Understanding when to seek medical intervention is vital. If you observe persistent discoloration, thickening, or changes in your nails, consult a healthcare provider to confirm diagnosis and begin appropriate treatment. Early intervention can significantly increase the likelihood of successful resolution and prevent complications like secondary bacterial infections.
Comprehensive Treatment Strategies for Toenail Fungus
Getting rid of toenail fungus involves multiple treatment options tailored to the severity of the infection, patient health, and specific circumstances. Approaches range from topical remedies to systemic medications and surgical interventions. Combining therapies may offer the best results, especially in stubborn cases.
- Prescription Antifungal Medications
- Topical Antifungal Treatments
- Nail Thinning and Removal Procedures
- Home Remedies and Lifestyle Changes
Oral antifungal drugs are often regarded as the most effective treatment for toenail fungus. They work by stimulating the growth of new, healthy nails, gradually replacing the infected portions. Common oral medications include terbinafine and itraconazole. Treatment duration typically ranges from 6 to 12 weeks, but visible improvement may take several months, depending on nail growth rates.
While oral antifungals can clear infections more efficiently, they also carry potential side effects. These can include skin rashes, liver toxicity, and interactions with other medications. Blood tests are usually recommended during treatment to monitor liver function and overall health. Patients with liver disease or heart failure are advised to avoid these medications or use them under strict medical supervision.
Topical applications like medicated nail polishes or creams are a preferred treatment for mild to moderate infections. Antifungal nail lacquers are painted onto the affected nails once daily, then cleaned off with alcohol before reapplication. Continuous use over several months, often up to a year, is necessary to see noticeable results. These treatments are generally safe, with minimal side effects, but they require patience and consistency.
In cases where the nail becomes excessively thick or unmanageable, doctors may recommend thinning the nail with medicated solutions or mechanical filing to enhance treatment penetration. If the infection is severe or unresponsive to other therapies, partial or complete removal of the nail may be necessary. Post-removal, topical antifungal agents can be applied directly to the nail bed to eliminate remaining fungi. Sometimes, surgical removal is done to prevent further spread and restore nail health.
Alongside medical treatments, certain home remedies can aid in managing toenail fungus. These include using over-the-counter antifungal creams, soaking feet in antifungal solutions such as tea tree oil or vinegar, and keeping nails trimmed and filed to reduce fungal load. Applying urea-based lotions can soften thickened nails, facilitating better medicament absorption.
Maintaining good foot hygiene is essential. Always keep feet dry by drying thoroughly after showers or swimming, and change socks regularly. Avoid sharing shoes, socks, or nail tools to prevent cross-contamination. Wearing moisture-wicking socks and breathable footwear helps reduce humidity—an environment conducive to fungal growth.
In addition, adopting a healthy lifestyle—managing blood sugar levels if diabetic, boosting immune health, and avoiding trauma to toenails—can significantly reduce the risk of reinfection.
Early diagnosis and consistent adherence to treatment regimens increase the probability of complete recovery. Be patient, as fungal nails can take several months to fully regenerate healthy tissue, and even then, some risk of recurrence exists. Regular follow-ups with healthcare providers ensure the infection is fully cleared and help detect any relapse early.
Remember, persistent or recurrent toenail fungus should never be ignored, as it can lead to further complications such as secondary bacterial infections or spread to other nails or skin areas. Effective management combined with preventive measures can restore nail health and improve overall foot comfort and appearance.
