Comprehensive Guide to Toenail Fungus: Causes, Symptoms, Prevention, and Effective Treatments
This detailed guide provides an in-depth understanding of toenail fungus, covering its causes, symptoms, prevention strategies, and natural treatment options. Early recognition and comprehensive care can prevent it from worsening and ensure healthy, fungus-free nails. Adopt proper foot hygiene, stay vigilant about risk factors, and explore effective remedies to keep your nails strong and healthy.
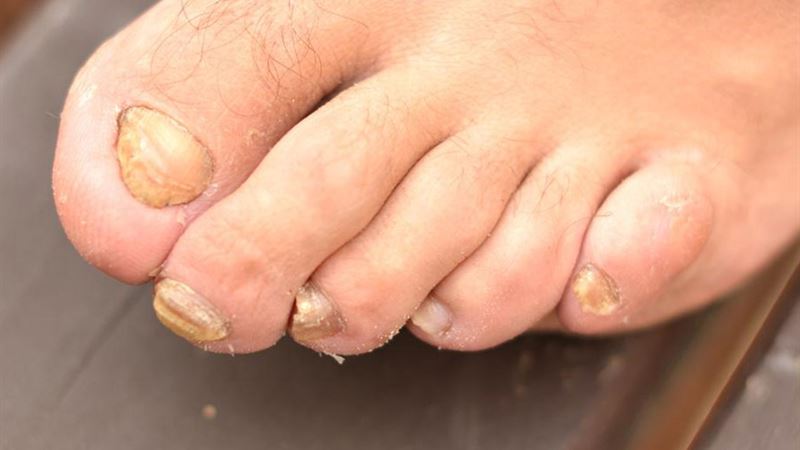
Toenail fungus, scientifically known as onychomycosis, is a common condition impacting millions worldwide. It manifests through various symptoms and can lead to discomfort, pain, and aesthetic concerns if left untreated. Understanding the root causes, recognizing the symptoms early, and adopting effective prevention strategies are essential steps toward managing this condition effectively. This extensive guide explores in detail the causes of toenail fungus, the common symptoms to watch for, risk factors, and practical treatment options, including both medical and natural remedies.
Ever experienced thickened, discolored, or crumbly nails? You might be dealing with toenail fungus. This infection predominantly affects toenails but can sometimes involve fingernails. It is caused by fungi, bacteria, or yeasts that invade the nail bed and keratin, leading to various structural and cosmetic changes. Factors like poor foot hygiene, moisture retention, and compromised immunity significantly contribute to its development. By understanding these elements, you can better prevent or control the spread of the infection.
Understanding the Causes of Toenail Fungus
The development of toenail fungus is typically due to fungal invasion, which occurs under specific conditions that favor fungal growth. Fungi thrive in warm, moist environments, making shoes, socks, and public wet areas common breeding grounds. Below are some primary causes and contributing factors:
- Existing fungal infections: Conditions like athlete’s foot often precede toenail fungus because the fungi can spread from the skin to the nails.
- Poor blood circulation: Insufficient blood flow, especially in older adults, hampers immune response and delays healing, increasing susceptibility.
- Contaminated footwear and shared spaces: Wearing shoes or socks previously used by an infected person, or frequenting communal facilities like swimming pools, gyms, and locker rooms, can lead to infection.
- Fungal spores in the environment: Fungal spores are prevalent in humid and damp environments—public showers, swimming pools, and locker rooms are typical contamination sites.
- Compromised immune system: Diseases such as diabetes, HIV/AIDS, or ongoing treatments like chemotherapy weaken immunity, making fungal infections more common.
- Physical trauma or injury to nails: Nail damage from injuries or repetitive trauma creates entry points for fungi.
- Other skin conditions: Disorders like psoriasis can alter nail structure, making them more vulnerable to fungal invasion.
- Footwear and hygiene habits: Tight shoes, non-breathable materials, excessive sweating, and neglecting foot hygiene create ideal conditions for fungi to flourish.
Recognizing the Symptoms of Toenail Fungus
Early detection of toenail fungus can prevent progression and complications. The symptoms vary, but common signs include:
- Thickening of the nail: A prominent symptom is the increased thickness, making trimming difficult.
- Discoloration: The affected nail often turns white, yellow, or brown, signaling fungal presence.
- Brittle and crumbly nails: Fungal infection weakens the nail's integrity, leading to breakage and crumbling edges.
- Shape distortion: The nail may become ragged, deformed, or distorted in shape.
- Debris accumulation: Dark debris or buildup under the nail and around the nails can discolor the nail bed.
- Odor: A foul smell might emanate from severely infected nails due to bacterial activity.
- Scaling and hyperkeratosis: Thickened, scaly skin or nail plate under or around the infected area.
- White or yellow streaks: Lateral onychomycosis presents as streaks across the nail surface.
- Yellow spots at the base: Proximal onychomycosis shows as yellow or white spots near the nail root.
- Nail detachment: When the infection advances, the nail can loosen and separate from the nail bed (onycholysis), potentially falling off.
Who Is at Risk of Developing Toenail Fungus?
While anyone can contract toenail fungus, some groups are more susceptible than others. Research indicates a higher prevalence among men than women, potentially due to differences in hygiene practices and footwear choices. Older adults face increased risk due to diminished blood circulation and slower nail regeneration processes. Diabetic individuals are particularly vulnerable because of impaired immune response and poor blood flow, which hinder healing and defense mechanisms.
Additionally, people with weakened immune systems, such as those undergoing chemotherapy or with autoimmune conditions, are more prone. Lifestyle choices like smoking also contribute to risk by impairing circulation and immune function. Athletes, swimmers, and individuals who frequently use public pools or gym facilities must exercise extra caution, as these environments are hotspots for fungal spores. Wearing improperly fitting shoes, which restricts airflow and promotes perspiration, further heightens vulnerability. Regular foot hygiene, dry feet, and proper footwear are crucial preventive measures.
Preventative Measures and Hygiene Tips
Preventing toenail fungus involves adopting good foot hygiene and vigilant practices. Here are some essential tips to reduce your risk:
- Keep feet dry and clean: Wash your feet daily, especially between toes, and dry them thoroughly to eliminate moisture that fosters fungal growth.
- Choose breathable footwear: Wear shoes made of materials that allow air circulation, and avoid tight-fitting shoes that cause sweating.
- Use moisture-wicking socks: Select socks that absorb sweat and change them regularly, particularly after physical activity.
- Avoid walking barefoot in public spaces: Use flip-flops or shower shoes in communal showers, pools, or locker rooms.
- Maintain good nail hygiene: Trim nails straight across, avoid over-trimming, and keep them clean to prevent fungal colonization.
- Disinfect shoes and footwear: Regularly treat shoes with antifungal powders or sprays, especially if someone in the household is affected.
- Limit sharing personal items: Do not share towels, shoes, or nail clippers to prevent cross-contamination.
- Monitor and manage health conditions: Keep blood sugar levels under control if diabetic, and consult your doctor for tailored health management.
Effective Home Remedies for Toenail Fungus
When it comes to mild cases, several natural remedies can assist in controlling and eliminating toenail fungal infections. These methods are cost-effective and generally safe but should be used consistently over time. If symptoms worsen or persist beyond a few weeks, consult a healthcare professional for proper diagnosis and treatment.
- Coconut oil: Known for its antifungal and antibacterial properties, coconut oil can be applied directly to the infected nails three to four times daily. Its lauric acid content helps in fighting fungal growth effectively.
- Baking soda: Baking soda’s alkaline nature alters the pH balance around the nail, creating an environment hostile to fungi. Apply a paste or soak your feet in a baking soda solution regularly to inhibit fungal development.
- Apple cider vinegar: Rich in acetic acid, apple cider vinegar helps acidify the environment of the affected area, preventing fungal colonies from thriving. Soaking feet in a mixture of vinegar and water for 15-20 minutes daily can yield positive results.
- Tea tree oil: This essential oil contains potent antifungal compounds. Dilute a few drops in a carrier oil and apply directly to the affected nails twice daily. It can help reduce infection and promote healthier nails. Lavender oil can be a suitable alternative if you prefer milder options.
- Garlic: Garlic contains allicin and ajoene, natural antifungal agents. Crush fresh garlic cloves, mix with white vinegar, and apply the mixture to the infected nails. Cover the area with a clean cloth and leave it on for a few hours each day for best results.
While home remedies are beneficial, persistent or severe infections require medical intervention. Consulting a dermatologist ensures an accurate diagnosis and inclusion of antifungal medications or other advanced treatments if necessary. Early intervention increases the likelihood of complete recovery and prevents complications such as nail loss or spread to other nails.
