Comprehensive Guide to Eczema: Symptoms, Causes, Types, and Effective Treatment Strategies
This detailed guide explores eczema in-depth, covering its symptoms, causes, various types, and effective treatment options. Learn how to manage flare-ups, identify triggers, and improve skin health. Empower yourself with knowledge to live comfortably with eczema and prevent complications through expert advice and proven strategies.
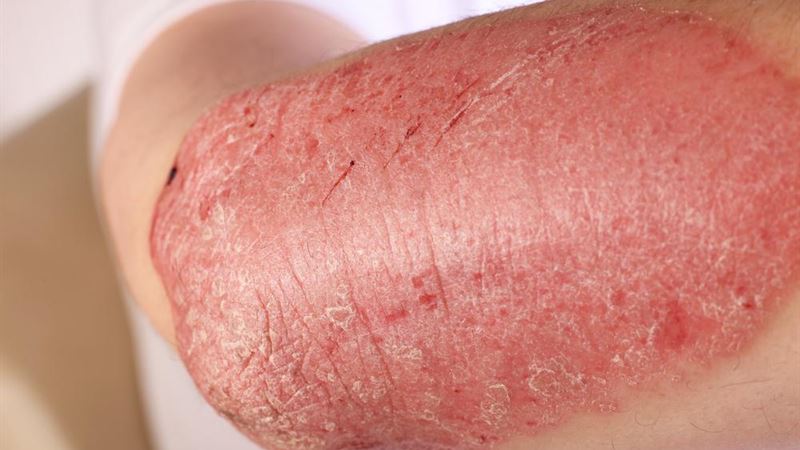
Eczema, also known as dermatitis, is a common skin disorder that affects millions worldwide. It manifests primarily through itchy, inflamed, and often dry skin patches, which can vary in appearance and severity depending on the individual. This chronic condition can surface at any age but tends to be especially prevalent in children and young adults. Its impact stretches beyond the physical symptoms, often affecting emotional well-being and daily activities. Because of its unpredictable nature, understanding eczema thoroughly is vital for proper control and symptom relief.
Recognizing the Symptoms of Eczema
Eczema presents through a range of symptoms primarily involving the skin’s surface. While the specific appearance can depend on the type and location, many signs are common across different forms. Recognizing these symptoms early on can aid in prompt management and prevent complications such as infections or chronic skin damage.
- Intense Itching: One of the hallmark symptoms, itching is often severe and persistent, prompting scratching that can exacerbate the condition.
- Inflamed Skin: Affected areas typically become red and swollen, indicating inflammation and immune response activity.
- Dryness and Scaling: The skin may become dry, flaky, and develop a scaly texture, especially in chronic cases.
- Thickened Skin: Continued scratching can lead to lichenification—thick, leathery patches resulting from skin thickening.
- Blistering and Oozing: In some instances, skin blisters form, burst, and crust over, risking secondary infection.
- Color Changes: In lighter skin tones, erythema (redness) is prominent; in darker skin, affected areas might look darker or lighter than surrounding skin.
Additional symptoms can include burning sensations or rawness in affected areas, especially when skin is broken or infected. These symptoms tend to fluctuate, with periods of flare-ups and remission, complicating management and daily life.
What Are the Underlying Causes of Eczema?
The exact cause of eczema remains complex and multifactorial. It generally involves a malfunction of the skin's protective barrier along with immune system dysregulation. Several factors can act as triggers, activating or worsening the condition.
Primarily, eczema is linked to an overactive immune response to environmental allergens or irritants. For example, exposure to allergens like pet dander, pollen, or dust mites, or contact with irritants such as harsh soaps, detergents, or rough fabrics, can provoke flare-ups. Additionally, environmental factors like extreme temperatures—cold or hot weather—can exacerbate symptoms.
Other contributing factors include:
- Genetic predisposition: A family history of eczema, allergies, or asthma increases risk.
- Skin barrier dysfunction: Defects in the skins’ protective layer make it more permeable to irritants and allergens.
- Stress: Emotional stress can trigger or worsen eczema episodes.
- Environmental pollutants: Exposure to pollution and chemicals can aggravate the condition.
- Hormonal changes: Fluctuations, especially in women, can influence eczema severity.
It’s vital to emphasize that eczema is not contagious. You cannot catch it from someone else, although individuals with eczema are often more sensitive and may develop other allergic conditions.
Different Categories and Types of Eczema
Eczema encompasses various forms, each with unique characteristics, common locations, and triggers. Understanding these differences is essential for targeted management.
- Atopic Dermatitis: The most prevalent form, typically beginning in childhood. It’s associated with allergic conditions like asthma and hay fever. Usually affecting the face, neck, elbows, and knees, it tends to have a chronic, relapsing course with periods of flare-ups and remission.
- Stasis Dermatitis: Primarily seen in individuals with venous insufficiency. Usually affecting the lower legs, this form stems from poor circulation leading to fluid build-up and skin inflammation.
- Scabies: Caused by microscopic mites, the symptoms resemble eczema but are characterized by intense itching, especially at night, and require specific antiparasitic treatment.
- Fungal Dermatitis: Fungal infections, such as ringworm, can mimic eczema. Skin scraping under a microscope reveals fungal elements, leading to precise diagnosis and treatment with antifungals.
- Pompholyx (Dyshidrotic Eczema): Characterized by small, itchy blisters on palms, soles, or sides of fingers and toes. It often worsens with stress or heat.
- Nummular Eczema: Appears as round, coin-shaped patches of dry, scaly skin, often in older adults, mainly on the lower legs or arms.
- Lichen Simplex Chronicus: Causes thickened, leathery patches resulting from persistent scratching, typically on the neck or shins.
- Seborrheic Dermatitis: Affects oily areas such as the scalp, face, and chest, leading to greasy, flaky patches. In infants, it may present as cradle cap.
- Xerotic Eczema: Known for causing severely dry, cracking skin that may ooze or bleed.
- Allergic Contact Dermatitis: Develops after repeated exposure to an allergen, with symptoms confined to contact areas, such as jewelry, cosmetics, or chemicals.
Effective Treatment Approaches for Eczema
Managing eczema effectively hinges on controlling symptoms, preventing flare-ups, and addressing underlying triggers. Since dryness and itchiness are hallmark features, skincare routines focusing on hydration are fundamental.
Key strategies include:
- Regular Moisturization: Use emollients, ointments, or creams frequently throughout the day to restore and maintain the skin barrier.
- Gentle Skin Care: Avoid harsh soaps and detergents. Opt for mild, fragrance-free cleansers that preserve skin integrity.
- Medication: Topical corticosteroids are the frontline treatment to reduce inflammation, used as prescribed. In severe cases, doctors may recommend topical calcineurin inhibitors or oral medications.
- Antihistamines: Oral antihistamines can reduce itching, especially during sleep.
- Infection Control: If bacterial infection occurs, antibiotics may be prescribed. Proper wound care helps prevent further infection.
- Oozing and Blister Care: For leaking blisters, gentle cleaning with diluted vinegar solution or lukewarm water helps, followed by air exposure. Once dry, topical steroids can accelerate healing.
- Phototherapy and Light Therapy: Controlled exposure to ultraviolet light can lessen inflammation and is used under medical supervision.
- Immunosuppressants: In refractory cases, drugs like cyclosporine or newer biologics can be considered under specialist guidance.
It's also essential to identify and avoid personal triggers. Keeping a detailed diary of flare-ups can help recognize specific irritants or allergens.
Living Well with Eczema: Tips and Tricks
While eczema can be challenging and sometimes uncomfortable, the right management strategies can significantly enhance quality of life. Recognizing early signs and triggers is critical to prevent severe flare-ups.
Practical tips include:
- Wear soft, breathable fabrics like cotton, avoiding rough or woolen materials that irritate sensitive skin.
- Maintain a consistent skincare routine with moisturizers after bathing and multiple times during the day.
- Avoid known irritants such as harsh soaps, strong chemicals, or environmental pollutants.
- Manage stress through relaxation techniques, as stress often worsens symptoms.
- Keep nails short to minimize skin damage from scratching.
- Control environmental factors—use humidifiers in dry climates, keep rooms cool, and avoid extreme temperatures.
- Stay vigilant about food allergies, especially if eczema is linked to dietary triggers.
Collaborate closely with healthcare providers to develop a personalized management plan. Regular follow-ups can help adjust treatments and keep symptoms under control.
In conclusion, understanding eczema comprehensively—its symptoms, causes, types, and treatment options—is vital for effective management. With proper care, trigger avoidance, and medical intervention, individuals with eczema can lead comfortable, fulfilled lives despite this chronic condition.
