Comprehensive Guide to Recognizing and Managing Different Types of Eczema Symptoms
This comprehensive guide offers detailed insights into the symptoms, causes, and treatments of various eczema types. Understanding these aspects helps in early diagnosis and effective management, reducing discomfort and preventing complications. Learn how to identify triggers, choose appropriate skincare routines, and work with healthcare professionals to control eczema and improve skin health long-term.
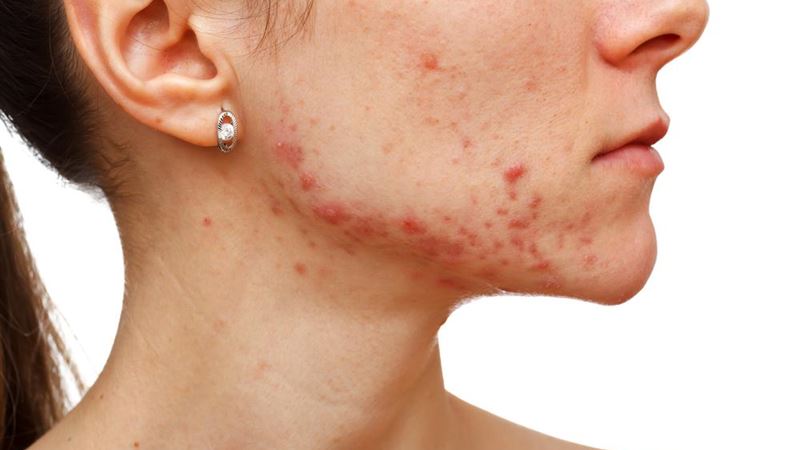
At its core, eczema begins with an intense urge to scratch a localized area. Initially, you may notice a sensation of restless itching that often intensifies. As the skin reacts, it develops redness and becomes dry, crusty, and thickened. The affected regions typically look flaky, scaly, or leathery, and the severity can range from mild discomfort to debilitating pain and irritation. For individuals with fair skin, the signs tend to manifest as striking red patches. However, for those with darker skin tones, the lesions might be less conspicuous, appearing as lighter or darker patches, which can sometimes make diagnosis challenging.
Scratching or rubbing these lesions can worsen the condition, often leading to the formation of blisters that may ooze or crust over. This progression increases the risk of local infections, especially if the skin breach becomes contaminated by bacteria. Recognizing these common symptoms early and understanding their variations across different skin types is essential for prompt and effective treatment.
Common Symptoms of Eczema
- Persistent redness and inflammation
- Dry, itchy, and flaky skin
- Darkened patches of thick, scaly skin
- Leathery, hardened skin patches
- Blisters that ooze, crust, or flake
- Intense itching that disrupts daily activities
Different Types of Eczema and Their Specific Signs and Symptoms
- Atopic Dermatitis:
This is the most widespread form of eczema, often associated with hereditary allergic conditions such as asthma and hay fever. It predominantly affects infants and young children but can persist into adulthood. The rash typically appears on the face, neck, wrists, behind the elbows, behind the knees, and around the mouth. Early signs include dry patches, redness, and sometimes oozing blisters that crust over. Itchiness is usually severe, leading to scratching that exacerbates the rash. The skin often becomes thickened and leathery over time due to chronic rubbing.
- Stasis Dermatitis:
This particular type primarily affects individuals with circulatory issues, especially those with chronic venous insufficiency. It manifests in the lower legs, especially around the ankles, with symptoms like swelling, dryness, scaling, and pigmentation changes. The skin may appear discolored, reddish-brown, or darkish, with areas prone to ulceration if left untreated.
- Scabies:
- Fungal Dermatitis:
This form mimics eczema with its red, itchy, and scaly patches. Microscope examination of skin scrapings can identify fungal elements, differentiating it from other eczema types. Proper antifungal treatment is necessary for resolution.
- Pompholyx (Dyshidrosis):
This condition causes clusters of tiny blisters, often on the palms, soles, sides of fingers, or toes. It is associated with itching and may be triggered by stress, heat, or moisture exposure.
- Nummular Eczema:
Typically affecting adults, this form appears as round, coin-shaped patches of itchy, scaly skin usually on the lower legs and arms. These patches can be persistent and challenging to treat.
- Lichen Simplex Chronicus:
It develops as a thickened, leathery plaque resulting from repeated scratching or rubbing, often found on the neck, wrists, and shins.
- Seborrheic Dermatitis:
This type predominantly affects oily areas of the skin, including the scalp, face, ears, and mid-chest. In infants, it presents as cradle cap or widespread scaly patches, sometimes oozing or crusting.
- Xerotic Eczema:
This dry skin variant results in cracked, fissured skin that can ooze or bleed. It often occurs in cold, dry environments and requires intensive moisturization.
- Allergic Contact Dermatitis:
This occurs after repeated exposure to specific allergens such as nickel, fragrances, or certain chemicals. It causes localized redness, swelling, blistering, and scaling at contact points, with symptoms worsening upon re-exposure.
What Causes Eczema?
Eczema is generally rooted in an overactive immune response, but various factors influence its manifestation. While breaches in the skin barrier can predispose individuals to infections or irritants, common triggers include contact with rough fabrics like wool or synthetic textiles that abrade or irritate the skin. Environmental factors such as extreme heat, cold, or humidity can also provoke symptoms. Allergens like pet dander, pollen, or certain foods may heighten sensitivity. Contact with harsh soaps, detergents, scented products, and chemicals can disturb the skin's integrity, leading to irritation. Stress and hormonal changes are additional contributors, often exacerbating existing eczema. Importantly, eczema is not contagious and cannot be transmitted from person to person.
How to Manage and Treat Eczema Effectively
The cornerstone of eczema management is maintaining healthy, moisturized skin to prevent dryness and cracking. Regularly applying emollients or barrier creams helps strengthen the skin and reduces flare-ups. Gentle cleansing with lukewarm water and mild, fragrance-free cleansers minimizes irritation. For itching and inflammation, topical corticosteroids are commonly prescribed; their judicious use can reduce redness, swelling, and itching. If bacterial infections develop, antibiotics may be necessary, applied topically or orally.
In cases where blisters ooze, cleaning the affected area gently with a diluted vinegar solution or plain water followed by air-drying assists in minimizing infection risks. Once the skin is dry, corticosteroid ointments can accelerate healing.
Antihistamines can help alleviate severe itchiness, especially at night, improving sleep quality. Phototherapy, involving controlled exposure to ultraviolet light, may be recommended for stubborn cases. Additionally, topical or systemic immune-suppressing medications like cyclosporine might be used when conventional treatments fail.
Living with eczema involves recognizing personal triggers and avoiding exposure whenever possible. For example, choosing clothing made from soft, natural fibers like cotton or silk, and avoiding wool or coarse materials, reduces irritation. Protecting skin from extreme temperatures, using gentle skin-care products, and avoiding known allergens are essential strategies. Stress management techniques such as yoga or meditation can also be beneficial in reducing flare-ups. Regular consultation with dermatologists or allergists ensures tailored treatment plans and effective management of the condition, enabling sufferers to lead comfortable, symptom-free lives.
