Understanding the Impact of Shingles on Nerve Health and Recovery Strategies
Discover comprehensive strategies for managing nerve damage caused by shingles. Understand the causes of persistent nerve pain, explore treatment options including medication, diet, and alternative therapies like acupuncture, and learn how a holistic approach can enhance recovery. Early intervention and lifestyle adjustments are key to preventing long-term nerve damage and improving quality of life post-shingles.
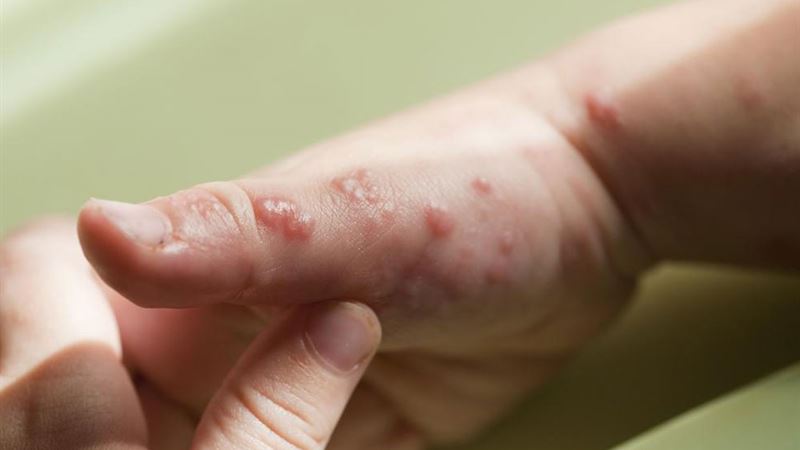
Shingles, medically known as herpes zoster, is a painful condition caused by the reactivation of the Varicella-zoster virus—the same virus responsible for chickenpox. After an individual recovers from chickenpox, this virus does not get eliminated from the body but remains dormant within nerve tissue for years. Typically, the immune system keeps the virus inactive, but various factors, including weakened immunity, stress, illness, or aging, can trigger its reactivation, leading to shingles. This condition manifests as a painful rash often accompanied by burning sensations, numbness, and tingling. While shingles is generally treatable if addressed early, it can sometimes result in more severe nerve damage and long-lasting complications if not managed promptly. Recognizing the importance of early intervention can prevent serious long-term effects on nerve health and overall quality of life.
The hallmark of shingles is its impact on the nerves, which can lead to persistent nerve pain even after the rash has healed. This enduring nerve pain is known as postherpetic neuralgia (PHN), and it poses a significant challenge for many patients. Understanding the relationship between shingles and nerve damage is crucial for effective management and recovery. Postherpetic neuralgia occurs when the nerves have been damaged during the viral reactivation process, causing abnormal nerve signals that result in chronic pain. This condition can affect any part of the body but is most common around the torso and face.
One of the key concerns following shingles is the possibility of nerve pain lingering for months or even years, which can severely impair daily activities and overall well-being. It is vital to differentiate nerve pain caused by shingles from other health issues, such as heart disease, appendicitis, or neurological disorders, to ensure appropriate treatment. The identification of nerve pain as a symptom related to shingles helps healthcare providers develop targeted treatment plans, which may include medications, physical therapy, and lifestyle modifications.
When nerve pain persists long after the initial shingles outbreak, it is classified as postherpetic neuralgia (PHN) or neuropathy. Neuropathy, in this context, refers to nerve damage caused by the viral infection, leading to disrupted nerve function. Managing this condition involves a multi-faceted approach that combines pharmacological treatments, nutritional support, and complementary therapies.
Medications such as anticonvulsants, antidepressants, and topical agents are commonly prescribed to alleviate nerve pain. However, adopting a comprehensive approach to health—building a robust immune system and maintaining overall well-being—plays a vital role in nerve recovery. Consuming a balanced diet rich in essential vitamins and nutrients supports nerve regeneration and reduces inflammation. Consulting with healthcare providers about appropriate supplements and dietary adjustments can be highly beneficial in this regard.
In addition to conventional medicine, alternative healing practices like acupuncture and herbal therapies have shown promise in managing nerve pain. Acupuncture, a traditional Chinese medicine technique, involves inserting fine needles into specific points on the body to stimulate nerve repair and reduce pain. While healing progress may be gradual, patience and persistence are crucial during treatment. Stress management is equally important, as heightened stress levels can hinder nerve healing and prolong discomfort.
Overall, recovering from shingles-induced nerve damage requires a holistic approach that emphasizes both medical intervention and lifestyle modifications. Proper diagnosis, timely treatment, good nutrition, and stress reduction strategies can significantly improve outcomes. Ensuring that individuals are well-informed about their condition can empower them to take proactive steps toward healing and nerve restoration. If nerve pain persists or worsens, seeking specialized medical advice is essential to avoid chronic complications and achieve optimal recovery.
