Understanding Shingles: Symptoms, Causes, and Prevention Strategies
Shingles, caused by reactivation of the varicella-zoster virus, primarily affects older adults and immunocompromised individuals. Early recognition of symptoms like pain, rash, and tingling, coupled with prompt treatment, can prevent serious complications. Vaccination remains a key preventive tool. Understanding the causes and risk factors enhances awareness, leading to better management and improved quality of life for those at risk of this painful condition.
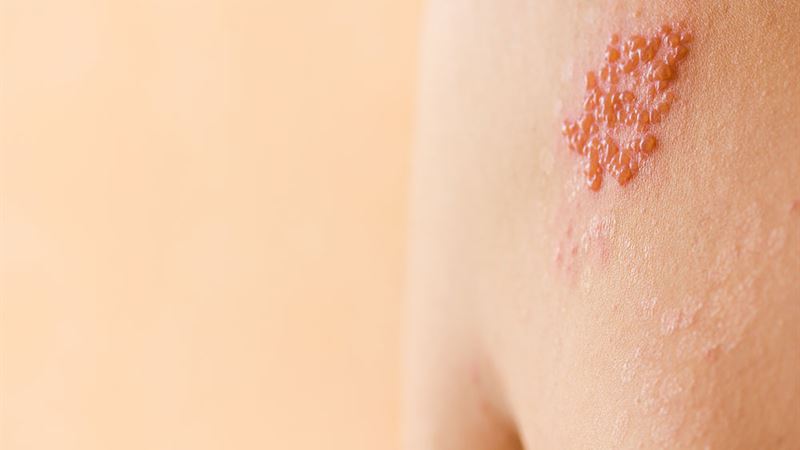
Shingles, also known as herpes zoster, is a condition that manifests through a variety of symptoms, predominantly affecting one specific side of the body. Recognizing these early signs is crucial for prompt diagnosis and effective treatment. Initial symptoms often include heightened skin sensitivity, sharp pain, tingling sensations, burning feelings, and numbness. These discomforts tend to precede visible skin changes and can often be mistaken for other conditions, making awareness vital.
As the disease progresses, a distinctive rash typically appears. This rash generally manifests as a band or strip of red patches accompanied by blisters filled with clear or slightly cloudy fluid. It commonly appears on one side of the torso, but can also affect areas around the face, especially near the eyes or on the cheeks, as well as on the neck or other parts of the body. Itching, swelling, and discomfort often accompany the rash. In some cases, the blisters may become infected, leading to pus formation.
Besides the skin symptoms, shingles can cause systemic symptoms such as fever, fatigue, headache, and heightened light sensitivity. These signs indicate the body's immune response to the viral reactivation.
Pain is typically the earliest and most pronounced symptom of shingles. Its severity can vary widely among individuals—from mild to debilitating. The pain often persists even after the rash has healed, a condition known as postherpetic neuralgia, which can last for months or even years, significantly impacting quality of life.
Correct diagnosis hinges on recognizing characteristic signs—particularly the localized rash and nerve pain. However, in atypical presentations, especially in immunocompromised individuals, the symptoms may be less specific, requiring laboratory tests such as skin scrapings or PCR testing for confirmation.
What Causes Shingles?
Although the precise trigger for shingles remains somewhat elusive, it is well-established that the condition results from reactivation of the varicella-zoster virus, the same virus responsible for chickenpox. After recovering from chickenpox, the virus does not completely leave the body; instead, it remains dormant in nerve tissue near the spinal cord and brain.
This dormant virus can reactivate years later, traveling along nerve pathways to reach the skin, where it causes the characteristic rash. The exact reasons why reactivation occurs are not fully understood. However, certain factors are known to increase the likelihood of outbreak, including weakened immune defenses, stress, aging, and other health conditions.
Individuals with compromised immune systems—such as those undergoing cancer treatments, organ transplant recipients, people with HIV/AIDS, or those taking immunosuppressive drugs—are at higher risk. Additionally, aging is a significant risk factor, with most cases occurring in people over the age of 50.
Link Between Chickenpox and Shingles
The connection between chickenpox and shingles is fundamental to understanding the disease. After a person has recovered from chickenpox, the virus remains latent in the nerve roots. It can stay dormant for decades without causing any symptoms. However, under certain circumstances—like immune system weakening—the virus can reactivate, leading to shingles.
This reactivation isn't contagious in the conventional sense; however, individuals with active shingles can transmit the virus to others who have never had chickenpox or been vaccinated against it. In such cases, the new person may develop chickenpox, not shingles.
Risk Factors Influencing Shingles Development
- Age: The older the individual, the greater the risk of reactivation.
- Immune suppression: Conditions or treatments that weaken the immune system increase risk.
- Stress and emotional strain: Prolonged stress can impair immune function, facilitating viral reactivation.
- Chronic illnesses: Diseases like diabetes or autoimmune disorders may elevate vulnerability.
- Lack of varicella vaccination: Vaccination significantly reduces the risk of developing shingles.
Preventive Measures and Treatment Options
While it's impossible to completely prevent shingles, certain measures can significantly reduce risk. The shingles vaccine is highly effective, especially in older adults, and can decrease both the incidence and severity of outbreaks. Consulting with a healthcare provider to determine if vaccination is appropriate is advised.
For those who develop shingles, early treatment is crucial. Antiviral medications like acyclovir, valacyclovir, or famciclovir are most effective when administered within 72 hours of symptom onset. These drugs can shorten the duration of the outbreak, reduce pain, and decrease the risk of complications such as postherpetic neuralgia.
Symptomatic treatments include pain relievers, corticosteroids, and topical agents to ease discomfort. Proper skin care is essential to prevent secondary bacterial infections. In cases of severe pain, nerve blocks or other nerve-targeted therapies may be considered.
Managing stress, maintaining a balanced diet, and supporting overall immune health can help prevent reactivation. For immunocompromised patients, regular medical follow-ups and possibly prophylactic antiviral therapy might be recommended to mitigate risks.
Complications of Shingles
Aside from the discomfort caused by the rash and nerve pain, shingles can lead to significant complications. Postherpetic neuralgia is the most common, characterized by lingering nerve pain long after the skin lesions have healed. This condition can be difficult to treat and greatly affect daily life.
Other complications include vision loss if the shingles involve the eye area (ophthalmic shingles), neurological problems such as encephalitis or meningitis, bacterial skin infections, and, rarely, hearing problems when the infection affects the ear nerve.
Conclusion: The Importance of Awareness and Early Intervention
Understanding the symptoms and causes of shingles is vital for early detection and effective management. Recognizing the initial signs can lead to prompt treatment, reducing the risk of long-term complications. Especially for older adults and immunocompromised individuals, vaccination and preventive strategies play key roles in reducing disease burden. Maintaining overall health, managing stress, and being vigilant about skin changes can make a significant difference in outcomes.
