Effective Strategies for Managing and Treating Shingles Outbreaks
Explore comprehensive strategies for managing shingles, including early signs, effective treatments, home remedies, and when to seek medical care to prevent complications and promote recovery. Learn how antiviral drugs, symptom relief tips, and preventive measures can help you handle shingles efficiently and minimize discomfort.
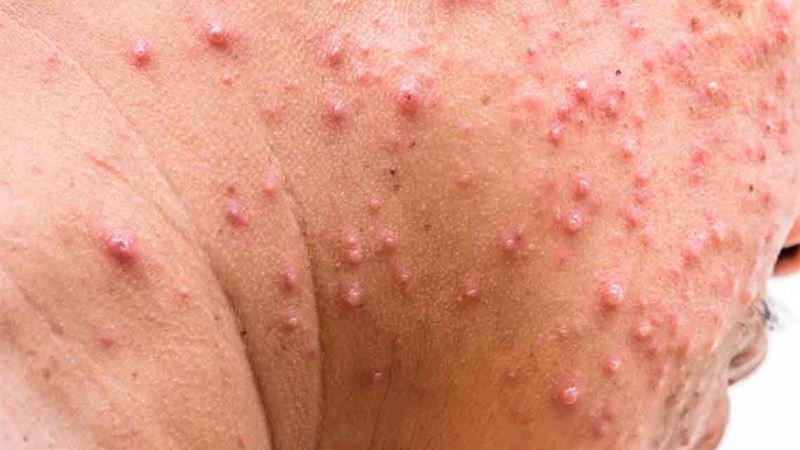
Shingles, medically known as herpes zoster, predominantly affects individuals over the age of 50, although it can occur at any age with a compromised immune system. People with weakened immunity due to stress, previous injuries, cancer treatments, or ongoing steroid therapy are more susceptible to this painful condition. If you had chickenpox during childhood, you harbor the varicella-zoster virus in a dormant state within nerve tissues, which can reactivate later in life as shingles. Pregnant women who experienced chickenpox can also transmit the virus to their unborn child, making early diagnosis and management vital. While recovering from shingles is often possible, recurrence is not uncommon, especially for those with ongoing health issues.
Early signs of shingles often include symptoms like headaches, heightened sensitivity to light, fatigue, and mild feverish feelings, often preceding the appearance of the rash itself. Recognizing these indicators early can lead to prompt treatment, potentially reducing the severity of symptoms and preventing complications. The hallmark of shingles is a painful rash that typically manifests in a specific nerve distribution on the face or body, often appearing as a band or strip of blisters. These blisters initially fill with fluid, eventually crusting over as they heal. The pain associated with the rash can range from mild discomfort to severe, debilitating sensations, often described as burning or stabbing. Despite its unpleasantness, shingles is generally not life-threatening, but it can result in long-term issues if left untreated.
Untreated shingles can lead to severe complications, especially for vulnerable populations. These may include partial or complete loss of vision if the rash develops near the eyes, facial paralysis, hearing loss, or even brain infections such as encephalitis. Recognizing these risks emphasizes the importance of early medical intervention. If shingles is suspected, especially in immunocompromised individuals or when the rash appears around sensitive areas like the eyes or nose, seeking immediate medical attention is critical. Proper diagnosis and treatment can significantly reduce the likelihood of irreversible damage. Self-medicating without professional guidance is discouraged, as incorrect treatment may worsen the condition or delay healing. Accurate diagnosis often involves visual examination and sometimes laboratory testing, especially in recurrent or atypical cases. Health professionals might take tissue cultures to confirm the presence of the virus, particularly if the rash persists or recurs. Immediate consultation is essential to prevent potential complications.
Although there is no definitive cure for shingles once it occurs, effective management focuses on alleviating symptoms, shortening the duration, and preventing complications. Antiviral medications, such as acyclovir, valacyclovir, and famciclovir, are the cornerstone of treatment if administered within 72 hours of rash appearance, boosting recovery rates and reducing pain severity. Complementary therapies include pain relievers, antidepressants for nerve pain, and corticosteroids to reduce inflammation. Topical creams, including those containing capsaicin or calamine lotion, can provide symptom relief. Early intervention within the first three days of rash onset is crucial for minimizing severity and preventing long-term consequences like postherpetic neuralgia—a persistent neuralgia pain after rash resolution. Always consult your healthcare provider before starting any medication regimen.
While shingles usually resolves with appropriate treatment, managing the pain and discomfort during the course remains a priority. The primary goal of medication is to suppress viral activity and soothe nerve pain, diminishing the overall distress caused by the rash. Most cases can be managed at home, provided there are no severe complications or immune system impairments requiring hospitalization. Hospitalization may be necessary for immunosuppressed patients or those with severe spread of the rash, especially involving critical areas such as the eyes or face. Proper rest, hydration, and adherence to prescribed medication are vital for optimal recovery. Understanding that shingles is contagious during the blistering phase underscores the importance of hygiene and isolation to prevent spread to others, particularly those who have not had chickenpox or are immunocompromised.
Home Care Tips to Accelerate Recovery from Shingles
- Avoid scratching or picking at blisters to prevent secondary bacterial infection and scarring.
- Apply a cool, moist compress or cloth to the affected areas to ease pain and reduce inflammation. Following this with calamine lotion can help soothe the skin.
- Use natural remedies such as cornstarch or baking soda paste on the sores to promote drying and healing, which may also decrease discomfort.
- To clean crusted lesions, soak the area in lukewarm water or a solution like Burrow’s, which helps reduce oozing and soothe irritated skin.
- Consult your healthcare provider for suitable topical creams or ointments to mitigate inflammation and discomfort.
- If signs of secondary infection, such as increased redness, pus, or swelling, appear, contact your doctor for antibiotic ointments for effective treatment.
In cases where symptoms worsen or if severe infection develops, seeking urgent medical advice is recommended to prevent further health deterioration.
