Comprehensive Guide to Managing Shingles: Symptoms, Treatments, and Prevention Strategies
This comprehensive article explores shingles, covering symptoms, causes, treatment options, and preventive measures like vaccination. It emphasizes early medical intervention and lifestyle strategies to manage and prevent this painful condition effectively. Clear guidance helps individuals understand how to act swiftly, reduce complications, and safeguard their health against shingles-related risks.
Understanding the risk factors associated with shingles can help individuals take proactive measures. People with weakened immune systems, older adults, or those under significant stress are more susceptible to the virus reactivating. Certain medications, such as immunosuppressants and chemotherapy drugs, can also increase vulnerability. Interestingly, the reactivation is not caused by new exposure to the virus but from the dormant virus within the body becoming active again. It is important to note that shingles cannot be transmitted from one person to another in the same way contagious diseases spread; however, the virus can be passed from a person with shingles to someone who has never had chickenpox, potentially resulting in chickenpox, not shingles.
There is currently no cure for shingles, but several treatments are available to relieve symptoms, reduce severity, and minimize complications. Early intervention is key to managing this condition effectively. Medical treatments include antiviral medications, pain management strategies, and preventive vaccines that significantly lower the risk of developing shingles or experiencing its severe consequences. Vaccination plays a vital role, especially for older adults, by boosting immune response and reducing the chances of reactivation. Moreover, additional supportive therapies such as topical creams and home remedies can expedite recovery and ease discomfort.
Recognizing the Symptoms of Shingles
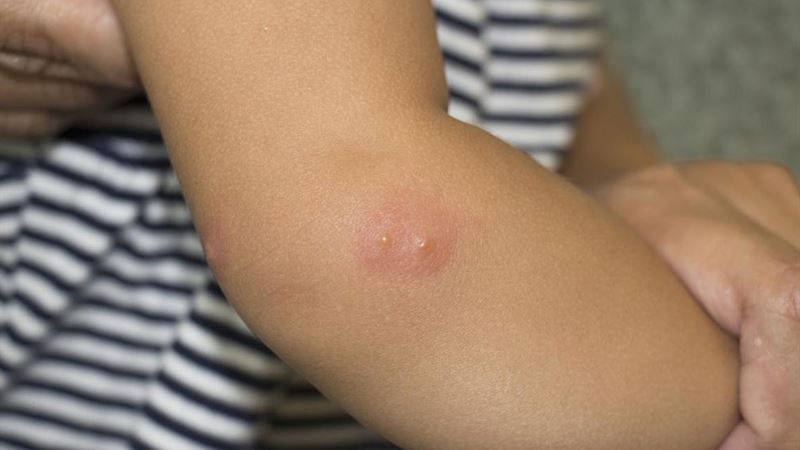
The symptomatology of shingles is diverse and progresses through various stages. Initially, individuals may experience prodromal symptoms such as headaches, fatigue, and heightened sensitivity to light—often mistaken for simpler ailments like the flu. Some people report mild feverish sensations, although high fever is less common. As the condition advances, the hallmark sign appears: a band of tingling, itching, or burning sensations localized to one side of the body, typically corresponding to a nerve pathway. Several days later, a rash develops—starting as small red patches that evolve into clusters of fluid-filled blisters. These blisters are generally painful, and as they crust over, they provide a visual indication of healing. During this phase, some patients may experience dizziness, weakness, or heightened sensitivity, which can vary in intensity.
The distribution of rashes often follows the dermatomal route—meaning it aligns with nerve pathways. The most concerning presentation involves the eye area, as rash extension into the ophthalmic nerve branch can jeopardize vision and lead to permanent eye damage. Since early symptoms can resemble other conditions, prompt consultation with a healthcare provider is essential once these signs appear. An accurate diagnosis enables timely treatment, which can significantly alter the illness trajectory and decrease risk of complications.
Effective Treatment Options for Shingles Pain
Prompt medical intervention can dramatically change the course of shingles. The cornerstone of treatment involves antiviral drugs, which are most effective when administered within 72 hours of rash onset. These medications—such as acyclovir, valacyclovir, and famciclovir—work by inhibiting viral replication, thereby reducing pain duration, rash severity, and postherpetic neuralgia risk. Besides antivirals, over-the-counter analgesics like acetaminophen or NSAIDs can provide immediate pain relief, but in severe cases, doctors may prescribe stronger pain relievers.
In addition to antiviral therapy, several other treatment options aim to relieve discomfort and prevent long-term complications:
- Antiviral medications such as acyclovir, valacyclovir, and famciclovir
- Pain relievers including opioids or neuropathic pain medications
- Antidepressants like amitriptyline or nortriptyline, which help manage nerve pain
- Topical agents such as capsaicin creams or lidocaine patches
Complementing medication, simple home remedies also support recovery. Keeping affected skin clean reduces risk of secondary infections, while applying cool, damp compresses can soothe irritated skin. Staying well-hydrated and maintaining a nutritious diet rich in anti-inflammatory foods can also speed up healing.
Persistent pain even after rash resolution is common, known as postherpetic neuralgia (PHN). This nerve pain can linger from months to years after the initial episode, impacting quality of life. Managing PHN involves additional medications, including anticonvulsants, opioids, or topical agents, and sometimes corticosteroids, under medical supervision.
Prevention Strategies and Vaccination
An essential component of shingles management is prevention. The shingles vaccine, recommended for adults over 50, has proven effective in reducing the incidence and severity of shingles. The two primary vaccines—Zostavax and Shingrix—boost immunity against the varicella-zoster virus, significantly lowering the chances of reactivation. Notably, Shingrix has shown superior efficacy and is preferred in most healthcare settings. Vaccination not only diminishes the occurrence but also helps lessen the intensity and duration of symptoms if shingles does develop.
Other preventive measures include maintaining a healthy immune system through regular exercise, balanced nutrition, sufficient sleep, and stress management. Avoiding exposure to ill individuals with active shingles lesions also minimizes the risk of transmitting the virus (for those without prior chickenpox). For immunocompromised individuals, consulting healthcare providers about vaccination timing and additional protection methods is crucial.
While shingles generally manifests in older populations, younger individuals with compromised immune systems should remain vigilant as well. An integrated approach combining vaccination and healthy lifestyle choices offers the best shield against this painful disease.
In summary, shingles is a manageable condition with proper medical treatment, timely vaccination, and lifestyle adjustments. Recognizing early symptoms and seeking immediate care are vital steps toward reducing pain, preventing complications, and maintaining a good quality of life. If you suspect shingles or experience nerve pain and rash, consult your healthcare provider promptly for personalized advice and treatment options.
