Comprehensive Guide to Shingles: Symptoms, Causes, and Treatments
This comprehensive guide explores shingles, its causes, symptoms, treatments, and prevention strategies. Learn how to identify early signs, understand risk factors, and discover effective medical and home remedies to manage the disease. Protect yourself from complications with timely intervention and vaccination. Whether you're seeking knowledge for personal health or caring for a loved one, this detailed article offers valuable insights into one of the most common nerve-related skin conditions, ensuring you stay informed and prepared.
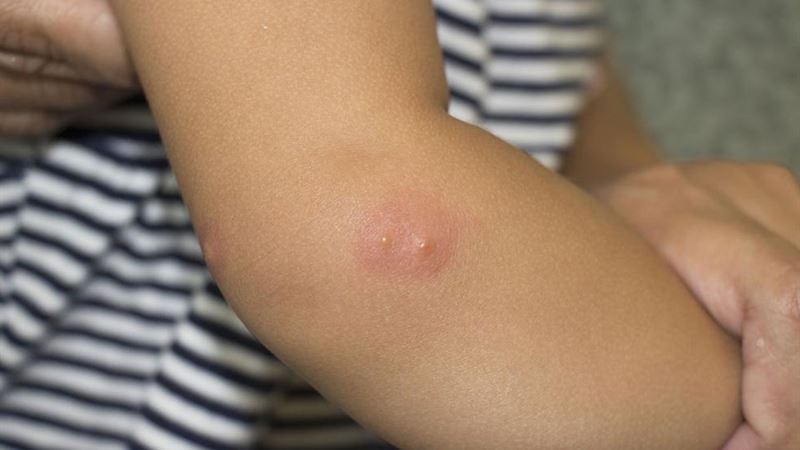
Shingles, also known as herpes zoster, is a painful skin condition caused by the reactivation of the varicella-zoster virus—the same virus responsible for chickenpox. Medical professionals often attribute the reactivation of this virus to a compromised immune system, which can be triggered by various factors. As individuals age or experience stress, their immune defenses weaken, increasing the likelihood of virus activation. Additionally, underlying health conditions such as cancer, HIV/AIDS, or other immune-compromising illnesses can heighten the risk. Even psychological stress, emotional upheavals, or physical exhaustion can act as catalysts for the virus's reemergence. Public awareness about the contagious nature of shingles is vital, especially for those with weakened immunity, as the disease can spread through direct contact with active lesions.
It is crucial to maintain caution and distance from individuals exhibiting shingles symptoms to prevent transmission. People who have previously had chickenpox remain susceptible to developing shingles later in life, especially if their immune system becomes compromised. The clinical diagnosis of shingles involves visual examination by a healthcare professional, who looks for characteristic rash patterns and associated symptoms. Treatment primarily involves antiviral medications such as acyclovir, valacyclovir, or famciclovir, which are most effective when administered early in the outbreak. Pain management is also essential; doctors often prescribe analgesics or recommend topical ointments that provide numbing relief from intense itching and discomfort. Complementary therapies, such as bathing with neem leaves or applying soothing herbs, can help alleviate symptoms and reduce post-infection scarring.
Preventive measures include vaccination, especially for older adults or those with risk factors, which can significantly reduce the severity and duration of shingles episodes. Patients are advised to avoid scratching the affected area to minimize scarring. An important aspect of managing shingles involves understanding the progression of symptoms, which typically develop gradually. The initial stage often manifests as general malaise, fatigue, and body aches, signifying the body's early response to viral reactivation. Early detection and prompt medical intervention can lessen the severity of subsequent symptoms and prevent complications such as postherpetic neuralgia—the lingering nerve pain that persists even after skin healing.
- Localized Pain and Redness: Initially, individuals may experience sharp, burning pain and redness confined to a specific body region. This discomfort often occurs days before a visible rash appears, signaling early shingles onset.
- Emergence of Rash: Within 2 to 5 days, a rash resembling chickenpox develops, characterized by small red patches that quickly evolve into fluid-filled blisters surrounded by inflamed skin.
- Blistering and Itching: The blisters can be intensely itchy and may rupture, releasing fluid. This stage often accompanies a throbbing or stabbing sensation, which can be excruciating for some patients.
- Additional Symptoms: Headaches, sensitivity to light and sun exposure, tearing eyes, and facial discomfort are common. Many sufferers report persistent tingling or prickling sensations around the rash, indicating nerve involvement.
- Systemic Manifestations: Some individuals experience general symptoms such as fever, chills, weakness, dizziness, nausea, and muscle aches, indicating the body's response to the infection.
- Facial and Eye Involvement: When shingles affects the face, it can involve critical areas such as the eyes, mouth, and ears. Eye involvement may lead to conjunctivitis, inflammation, or vision problems, highlighting the need for urgent ophthalmologic consultation.
- Spread and Complications: If untreated, shingles can lead to complications like postherpetic neuralgia, bacterial skin infections, and, in severe cases, neurological issues such as nerve damage or hearing loss.
- Approach to Treatment: Besides antivirals, supportive care includes resting, keeping the rash clean and dry, and using cool compresses to reduce pain and swelling. Some medications target nerve pain specifically, while corticosteroids may be prescribed to decrease inflammation. Vaccination has also proven effective in preventing severe shingles episodes and reducing complication rates.
- Duration and Recovery: The course of shingles typically spans about three weeks. The first week and a half are usually the most intense, characterized by severe pain, fever, and visibility of blisters. As healing progresses, symptoms gradually diminish, but some individuals may experience persistent pain or residual scars. Ensuring proper medical care during this period can help minimize long-term effects and promote faster recovery.
