Explore an in-depth overview of chronic psoriasis, including its various types, symptoms, and current treatment options. Learn how personalized therapies can help manage flare-ups, improve skin health, and enhance quality of life. This comprehensive guide offers valuable insights for patients and healthcare providers aiming to effectively control psoriasis and prevent complications.
Chronic psoriasis is a persistent autoimmune skin disorder characterized by abnormal immune responses that lead to the rapid buildup of skin cells. This condition manifests in various forms, each with distinct symptoms and severity levels, requiring tailored treatment strategies. Managing psoriasis involves understanding its different types, recognizing specific symptoms, and applying appropriate therapies to control flare-ups and improve quality of life.
Living with psoriasis can be challenging, but advances in dermatology have provided numerous treatment options to help patients manage the condition effectively. The severity of psoriasis varies among individuals, ranging from minor patches to widespread plaques that significantly impact daily functioning. Proper diagnosis and understanding of the specific psoriasis type are crucial for selecting the most effective treatment plan.
This comprehensive guide explores the various types of chronic psoriasis, their characteristic symptoms, common triggers, and the latest treatment modalities. Whether you are newly diagnosed or seeking to understand your condition better, this article provides detailed insights into managing psoriasis effectively and improving overall skin health.
Let's begin by understanding what psoriasis is and how it develops beneath the skin, often without immediate visible signs. This knowledge is key to grasping the complexity of the disease and the importance of personalized treatment approaches.
Understanding Psoriasis: Causes and Symptoms
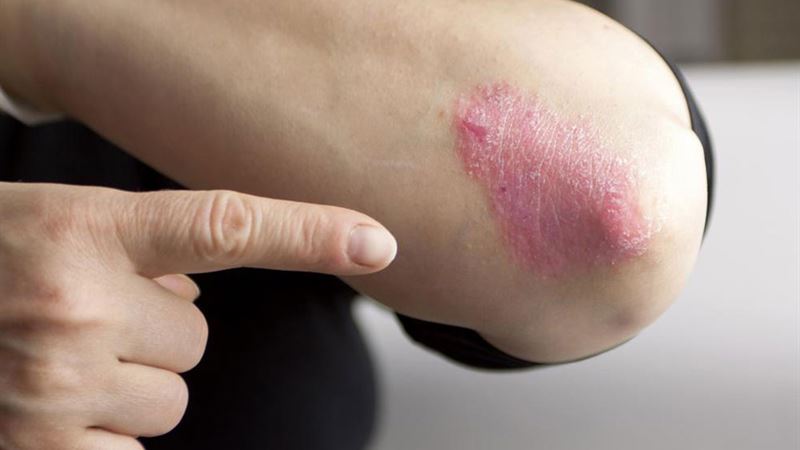
- Inflamed, red patches on the skin
- Presence of silvery, scaly patches on affected areas
- Persistent itchiness and discomfort
- Swelling, stiffness, or pain in joints (in cases of psoriatic arthritis)
The symptoms of psoriasis are highly variable, depending substantially on its type. Some may experience mild itching, while others could face painful lesions affecting their daily activities. Recognizing these symptoms early is essential for prompt treatment and preventing complications.
The Different Types of Chronic Psoriasis
Psoriasis is not a one-size-fits-all condition. It encompasses distinct types, each with unique features and triggers. Understanding these classifications can help in customizing treatment plans for better management and symptom control. Sometimes, individuals experience multiple types simultaneously or develop new variants over time, especially triggered by environmental or internal factors.
There are approximately seven recognized types of psoriasis, outlined as follows:
- Plaque Psoriasis (Psoriasis Vulgaris): This is the most prevalent form. It presents as raised, inflamed skin patches covered with silvery-white scales, often occurring on elbows, knees, scalp, and lower back. These plaques can be itchy, tender, and sometimes crack or bleed, leading to discomfort.
- Guttate Psoriasis: Predominantly affecting children and young adults, this type appears as small, drop-shaped, pink-red spots mainly on the trunk, arms, thighs, and scalp. Common triggers include infections, stress, or certain medications. It may resolve spontaneously or develop into other psoriasis types.
- Pustular Psoriasis: An uncommon but severe form characterized by white, pus-filled bumps (pustules) surrounded by inflamed skin. It can be localized or generalized, with widespread pustular psoriasis demanding urgent medical attention due to risks of infection and systemic symptoms.
- Inverse Psoriasis: Also called flexural psoriasis, it affects skin folds such as underarms, groin, or around the genitals, presenting as shiny, bright red patches without the typical scales. This type worsens with friction, sweating, or scratching, causing significant irritation.
- Erythrodermic Psoriasis: A rare but life-threatening form involving widespread redness, peeling, and severe inflammation covering most of the body, often accompanied by fever and chills. Its management requires hospitalization and emergency intervention to prevent complications like dehydration or infection.
- Nail Psoriasis: Affecting nail beds and surfaces, it causes pitting, ridging, discoloration, and separation of nails from the nail bed. Nail psoriasis often occurs with other psoriasis types and can significantly impair hand and foot function.
- Psoriatic Arthritis: This form combines skin psoriatic lesions with joint inflammation, leading to pain, swelling, and stiffness. It can mimic other forms of arthritis but is distinguished by its association with psoriatic skin changes and possible deformities.
Effective Treatments Tailored to Psoriasis Types
Managing psoriasis requires personalized approaches depending on its type, severity, and patient-specific factors. While the root cause—an overactive immune response—cannot be entirely cured, symptoms can be effectively controlled using various treatment modalities.
Plaque Psoriasis Treatments: Topical corticosteroids, moisturizers, and vitamin D analogs are standard first-line therapies. Light therapy (phototherapy), such as UVB, is often combined for more resistant cases, especially involving scalp and large plaques.
Guttate Psoriasis Management: Addressing underlying infections is crucial, often supplemented with topical steroids, ultraviolet light therapy, and systemic medications when necessary. Avoiding triggers like stress and medications linked to outbreaks can help prevent recurrence.
Inverse Psoriasis Care: Topical steroid creams are commonly prescribed, alongside adjunct treatments like calcineurin inhibitors. Maintaining dry, cool skin and avoiding friction are essential for symptom relief.
Pustular Psoriasis Treatment: Localized pustules respond to topical corticosteroids and soothing emollients. Extensive pustular psoriasis may require systemic medications like retinoids, immunosuppressants, or biologic agents.
Erythrodermic Psoriasis Management: Emergency intervention, hospitalization, and systemic therapies—such as intravenous fluids, corticosteroids, and immunosuppressants—are necessary to stabilize the patient and prevent fatal complications.
Nail Psoriasis Approaches: Treatments include topical steroids, vitamin D analogs, and occasionally systemic therapies, especially when nail disease is severe or associated with joint involvement.
Psoriatic Arthritis Care: A combination of NSAIDs, disease-modifying antirheumatic drugs (DMARDs), biologics, and physical therapy aims to reduce joint pain and prevent deformities.
While current treatments can help manage symptoms and improve quality of life, ongoing research continues to develop targeted therapies. Advances in biologic agents have revolutionized psoriasis care, especially for moderate to severe cases, offering longer-lasting remission and fewer side effects.
Early diagnosis and tailored treatment strategies are crucial to controlling this chronic condition. Patients should work closely with dermatologists to identify triggers, establish effective management plans, and monitor progress regularly.

