Understanding the Common Causes and Risk Factors of Atopic Dermatitis
Atopic dermatitis is a common chronic skin condition influenced by genetics, environmental factors, and allergic tendencies. It often appears alongside asthma and hay fever, with family history playing a significant role. Managing this condition involves identifying triggers and following personalized treatment plans to reduce flare-ups and improve skin health.
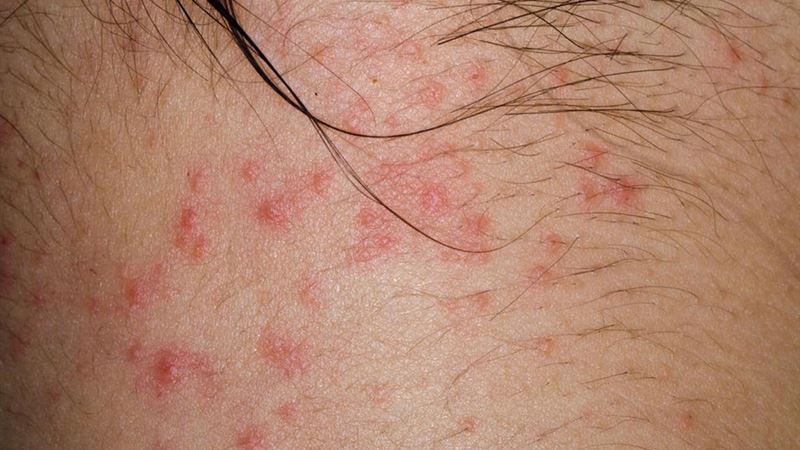
Despite extensive research, the precise etiology of atopic dermatitis remains elusive. It is widely considered a complex interplay of genetic predispositions, immune system responses, and environmental influences. The condition frequently coexists with other allergic conditions such as asthma and hay fever, suggesting a shared underlying allergic pathway. Family medical history plays a crucial role in assessing risk; individuals with relatives who have asthma, hay fever, or other allergic diseases are more susceptible to developing atopic dermatitis themselves.
Genetic factors are believed to contribute significantly to the development of this condition. Studies have shown that if one parent has atopic dermatitis, asthma, or hay fever, there is approximately a 50% chance that their child will inherit the tendency to develop these allergic responses. This hereditary aspect underscores the importance of family history in diagnosing and predicting the risk of atopic dermatitis. When both parents have one or more of these allergic conditions, the probability increases substantially, making genetic predisposition a pivotal element in disease manifestation.
Environmental triggers also play a vital role in exacerbating or triggering flare-ups of atopic dermatitis. External allergens such as pollen, pet dander, dust mites, and certain foods can provoke skin reactions, leading to inflammation, itching, and redness. Seasonal changes and climate conditions, including dry air and exposure to harsh soaps or chemicals, can further aggravate the condition. Identifying and minimizing exposure to these triggers are critical steps in managing atopic dermatitis effectively.
In managing atopic dermatitis, dermatologists often recommend a combination of lifestyle modifications, skincare routines, and medications. Topical steroids and moisturizers are commonly used to reduce inflammation and soothe the skin, while antihistamines may be prescribed to control itching. In some cases, immunotherapy or other advanced treatments may be necessary, especially when traditional therapies do not produce adequate relief. An individualized treatment plan based on medical history and severity is crucial for optimal disease management.
