Understanding How Baby Eczema Changes with Age and the Role of Steroid Therapy
Discover how baby eczema varies with age, from infants to toddlers, and learn about safe steroid treatments. This comprehensive guide provides insights into symptoms, management strategies, and tips for caregivers to effectively control eczema in young children over time, ensuring comfort and healthier skin development.
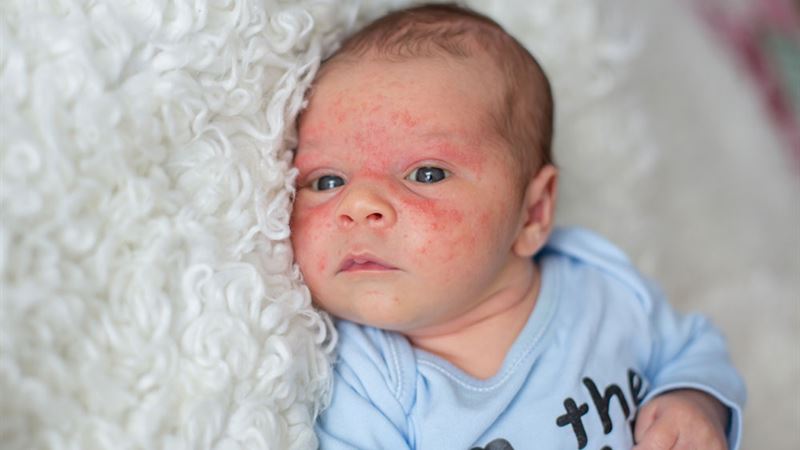
Baby eczema, medically known as atopic dermatitis, manifests differently as a child grows, influenced by age, skin development, and environmental factors. Recognizing these variations is crucial for effective management and treatment. From infancy through early childhood, eczema can present with distinct characteristics, requiring tailored approaches at each stage of development. This comprehensive guide explores the evolution of eczema in young children, explains common symptoms, highlights effective treatment options including topical steroids, and provides practical advice for parents and caregivers to manage the condition safely and effectively over time.
In infants aged 6 to 12 months, eczema typically appears on areas that are easily accessible and prone to scratching, such as the elbows and knees. These regions are often the first to develop rashes because babies frequently manipulate these parts, leading to irritation and potential infection. The skin may develop pus-filled bumps if bacterial infection occurs, which complicates the condition further. During this stage, eczema might be quite noticeable, with redness, roughness, and itching disturbing the baby’s comfort and sleep patterns.
As children transition into toddlerhood, aged 2 to 5 years, eczema often progresses into a more chronic form. One hallmark of this phase is the development of lichenification—a thickening of the skin characterized by rough, scaly patches with deeper lines or ridges. This occurs due to persistent scratching and rubbing, which causes the skin to become leathery. The affected areas typically include the creases behind the knees, inside elbows, and around the wrists, hands, and ankles. Eczema can also appear around the face, especially around the mouth and eyelids, indicating that the disease affects not only the flexural areas but also more delicate parts of the face.
Management of eczema in children involves a combination of topical treatments, skin care routines, and sometimes systemic medications. Among the most commonly prescribed therapies are steroid creams and ointments, combined with emollients to restore skin hydration. These topical steroids are potent anti-inflammatory agents that help reduce redness, swelling, and itching. When used correctly under medical supervision, they are considered safe and effective for controlling flare-ups.
It's important to understand that topical steroids have potential side effects, the most notable being skin thinning if overused or applied for prolonged periods. However, there is no evidence to suggest that such effects are permanent if treatment is discontinued appropriately. To ensure safety, parents should adhere strictly to the dosage and duration prescribed by their child's healthcare provider—usually applying the steroid only on affected areas and no more than twice daily. Combining steroid use with regular application of emollients enhances skin barrier repair and reduces flare-ups.
In severe cases, where itching is intense and persistent, oral antihistamines might be recommended to alleviate discomfort, although they are used less frequently. These medications can help reduce itching and improve sleep quality. Alongside pharmacological treatment, identifying and avoiding eczema triggers such as allergens, irritants, and environmental factors like harsh soaps or extreme weather changes is essential for long-term management.
Beyond medication, daily skin care routines play a pivotal role. Bathing in lukewarm water with gentle, fragrance-free cleansers, followed by immediate moisturizing with thick emollients, helps maintain skin hydration and prevent flare-ups. Wearing soft, breathable clothing, and avoiding scratchy fabrics can also minimize skin irritation. Families should keep a close watch for signs of infection, such as increased redness, warmth, swelling, or pus, and seek medical attention promptly if these occur.
In summary, eczema in babies and young children evolves with age, necessitating an understanding of its distinct manifestations at each stage. With proper medical treatment—including the cautious use of topical steroids—alongside diligent skin care practices, affected children can experience significant relief and improved quality of life. Education of parents and caregivers about safe medication use and skin management strategies is crucial in preventing complications and promoting healthy skin development as the child grows.
