Comprehensive Guide to HIV-Related Skin Rashes: Causes, Symptoms, and Treatments
This comprehensive guide offers detailed insights into HIV-related skin rashes, including their causes, symptoms, triggers, and treatments. Understanding these skin conditions helps in early detection and effective management of HIV. The article covers common rashes like seroconversion, herpes, cellulitis, and fungal infections, emphasizing the importance of medical consultation for proper care. Stay informed about HIV skin manifestations to maintain skin health and overall well-being with expert advice and practical tips.
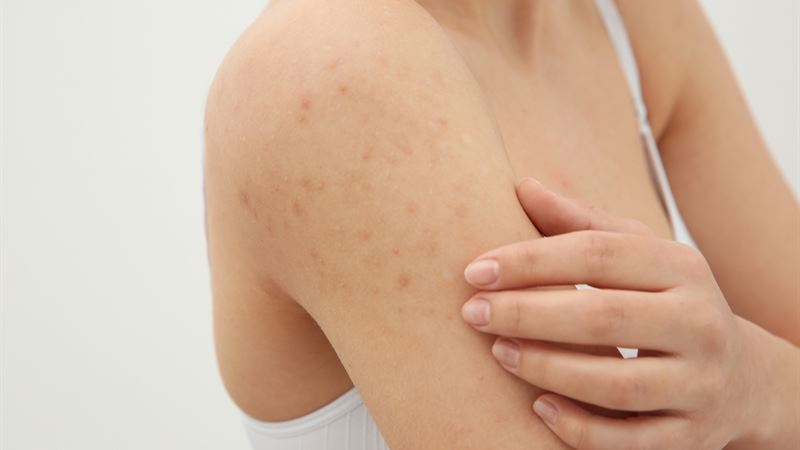
What Causes HIV Skin Rashes?
- The origin of HIV-associated rashes can be multifaceted. They may directly result from the immune system's response to the virus or as side effects of antiretroviral therapy (ART) medication. Allergic reactions to drugs are also common triggers.
Factors That May Worsen HIV Rashes
Because the precise trigger for an HIV rash is often uncertain, it is essential to avoid self-medicating or making significant lifestyle changes without consulting a healthcare professional. Several elements can exacerbate skin rashes in HIV-positive individuals, including:
- Exposure to infections, allergies, or illnesses that compromise the immune response can intensify skin issues.
- Use of certain medications, especially new drugs or antibiotics, may aggravate skin reactions.
- Prolonged exposure to direct sunlight can worsen rashes, leading to further discomfort.
- Changes in diet or eating habits might influence skin condition.
- Frequent switching of skincare or personal hygiene products can trigger adverse reactions.
- Temperature extremes or hot showers can inflame the skin further.
Understanding Seroconversion Rashes
- One of the early signs post-HIV infection is the appearance of a seroconversion rash. This occurs within weeks of contracting the virus, as the body begins producing HIV antibodies. The rash is often accompanied by flu-like symptoms, swollen lymph nodes, and other signs of acute infection.
- Typically, the seroconversion rash appears as flat red patches on the chest or back, and unlike other rashes, it usually does not itch.
Cellulitis and Its Impact on HIV Patients
- Cellulitis is a sudden and severe bacterial skin infection that penetrates deep into the skin layers, causing swelling, redness, and pain.
- This condition often begins with a minor cut or injury but can occur without any apparent skin breach, especially in immunocompromised individuals like those with HIV.
- The inflamed area becomes hot upon touch, and if untreated, the infection can spread rapidly, forming streaks of redness extending from the primary site.
- High fever and systemic symptoms are common with cellulitis, potentially leading to serious complications if ignored.
Herpes Rash and Its Manifestations in HIV-Positive Patients
- HIV-positive individuals are more prone to severe herpes infections due to weakened immunity. Herpes simplex viruses (HSV-1 and HSV-2) commonly cause painful blisters on the mouth and genital areas.
- Herpes lesions are crusty, tender, and contagious, necessitating medical intervention.
- Herpes zoster, otherwise known as shingles, usually presents as a one-sided rash in healthy people. However, in those with HIV, shingles can involve both sides of the body, leading to more extensive discomfort and difficulty in management.
Ringworm and Fungal Skin Infections
- Among common fungal skin conditions, ringworm (tinea corporis) is prevalent in HIV-positive individuals. It appears as ring-shaped, itchy patches with clear centers and scaly borders.
- Because the immune defenses are compromised, HIV patients are more susceptible to developing and spreading fungal infections like ringworm.
Understanding and managing skin rashes in HIV-positive individuals require a comprehensive approach, including medical diagnosis, appropriate treatments, and lifestyle modifications. Early detection of skin manifestations can lead to better disease management and improved quality of life for affected individuals.
