Comprehensive Guide to Insulin Types and Delivery Methods for Diabetes Management
This comprehensive guide explores various insulin types and delivery methods for effective diabetes management. Learn about rapid, short, intermediate, and long-acting insulins, as well as innovative inhaled options and user-friendly pens. Proper understanding ensures better glucose control and improved quality of life for diabetics. Stay informed on modern treatments and techniques to optimize your health and prevent complications.
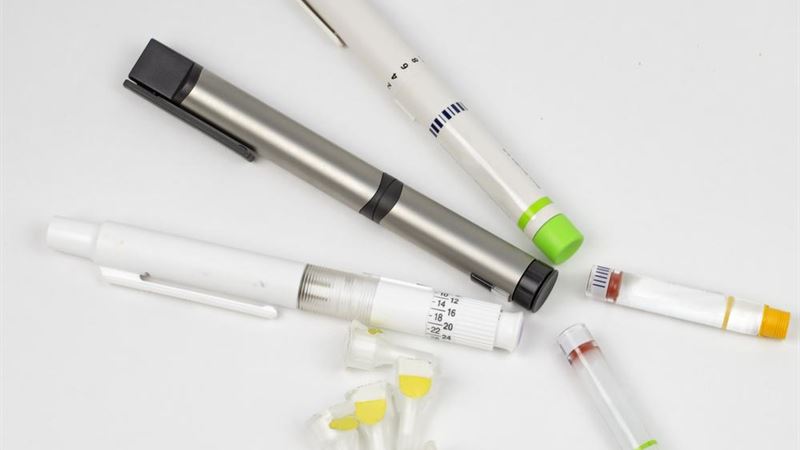
Types of Insulin Used in Diabetes Treatment
Rapid-acting insulins are designed to start working swiftly after injection, making them ideal for controlling blood sugar spikes during meals. Examples include Insulin Glulisine (marketed as Apidra), Insulin Lispro (Humalog), and Insulin Aspart (NovoLog). These insulins typically begin to lower blood glucose levels within 15 minutes. Their peak effect usually occurs around one hour post-injection, and they remain effective for approximately 2 to 4 hours. Due to their quick action, these insulins are often administered immediately before or shortly after eating, providing flexibility and better post-meal blood sugar control.
Regular insulin, also known as short-acting insulin, includes brands such as Humulin R and Novolin R. These insulins generally take about 30 minutes to start working after injection. They reach their peak effect between 2 to 3 hours and continue to work effectively for about 3 to 4 hours. This type of insulin is often used around meal times and can be prescribed in combination with other insulins to achieve optimal blood sugar management. Its predictable onset and duration make it suitable for scheduled dosing, especially for individuals who prefer injections before meals.
Intermediate-acting insulins like NPH (which stands for Neutral Protamine Hagedorn) include brands such as Humulin N and Novolin N. These insulins typically start to act within 2 to 4 hours after injection, with their peak effect occurring between 4 and 12 hours. They have a duration of action of approximately 12 to 18 hours, making them useful for basal insulin coverage—providing a steady background level of insulin throughout the day and night. NPH insulin is often administered once or twice daily, sometimes in combination with rapid or short-acting insulins to provide comprehensive blood sugar control.
For consistent and prolonged insulin coverage, long-acting insulins such as Insulin Detemir (marketed as Levemir) and Insulin Glargine (Lantus) are preferred. These insulins usually begin acting several hours after injection and tend to release insulin gradually and evenly over a 24-hour period. They are often chosen to mimic the body's natural baseline insulin secretion, helping to maintain stable blood glucose levels throughout the day and night. Long-acting insulins require less frequent injections and are usually administered once daily, offering convenience and better adherence to treatment plans.
Inhaled insulin, such as the Technosphere insulin-inhalation system (brand name Afrezza), offers a non-invasive alternative to injections. It begins acting within 12 to 15 minutes, reaching its peak effect after about 30 minutes, and exits the system approximately 3 hours post-inhalation. This method provides a quick onset of action, suitable for mealtime glucose control, and is particularly appealing to patients who prefer to avoid injections. However, not all individuals are suitable candidates for inhaled insulin, especially those with lung conditions like asthma or COPD. Regular monitoring and consultation with healthcare providers are essential when using inhaled insulins.
Insulin delivery is not limited to injections alone; insulin pens are widely used for their convenience and ease of use. These devices contain either a cartridge of insulin that can be inserted into the pen or are pre-filled and disposable. The dose of insulin can be precisely adjusted using a dial, ensuring accurate dosing tailored to individual needs. The needle attached to the pen is small and sharp, enabling less painful injections compared to traditional syringes. Insulin pens have revolutionized diabetes management, making injections quicker, more discreet, and more comfortable.
Proper management of diabetes involves regular monitoring of blood glucose and diligent administration of insulin. It is essential to keep an eye on diabetic supplies, including test strips, insulin pens, and syringes, to prevent unexpected health issues. Patient education and consistent adherence to prescribed treatment plans are crucial for maintaining stable blood glucose levels and minimizing the risk of complications such as neuropathy, nephropathy, and cardiovascular disease. With advancements in insulin formulations and delivery systems, managing diabetes continues to become safer and more convenient for millions worldwide.
