Understanding Sleep Apnea: Causes, Symptoms, Diagnosis, and Effective Treatments
Sleep apnea is a common yet serious sleep disorder caused by airway blockage or neurological issues. Recognizing the symptoms such as loud snoring and daytime fatigue is crucial. Diagnosis involves sleep studies like polysomnography or home testing. Treatment options include CPAP therapy, dental devices, lifestyle changes, and surgery. Lifestyle modifications like weight loss, positional therapy, and avoiding alcohol and smoking can greatly improve symptoms. Early detection and tailored treatment plans are essential for managing sleep apnea effectively and enhancing quality of life.
Exploring the Origins of Sleep Apnea
Sleep apnea is a prevalent sleep disorder characterized by interruptions in breathing during sleep. The two primary forms are obstructive sleep apnea (OSA), which is more common, and central sleep apnea (CSA). OSA occurs when the airway is physically blocked, often due to relaxed tissue or excess fat deposits, leading to breathing pauses and loud snoring. In contrast, CSA involves a failure of brain signals to instruct the muscles to breathe, with the airway remaining open but breathing ceasing due to neurological issues. Understanding the distinct causes of these types is essential for effective diagnosis and treatment.
The primary factors contributing to airway obstruction or collapse in sleep apnea include:
- Neurological control mechanisms
In CSA, the central nervous system's regulation of respiratory functions is impaired. Faulty brain signals can cause irregular breathing rhythms, which are often linked to medical conditions such as strokes, heart failure, or neurological disorders. Altitude changes and medication use, especially opioids and sedatives, can also influence respiratory control, increasing the risk of CSA. - Muscular relaxation during sleep
During sleep, the muscles responsible for maintaining airway openness naturally relax. When this relaxation becomes excessive or occurs in individuals with predispositions, it can cause airway narrowing. The tongue and throat muscles' relaxation can obstruct airflow, leading to breathing interruptions characteristic of sleep apnea. - Physical obstructions and tissue buildup
The presence of enlarged tonsils, adenoids, or excess fatty tissue around the neck can physically block the airway. This obstruction causes loud snoring and pauses in breathing during sleep, predominantly seen in OSA. Additionally, individuals with a large neck circumference or obesity are at heightened risk due to increased tissue mass exerting pressure on the airway.
Additional risk factors include:
- Obesity and excess weight
- Sleeping on the back (supine position)
- Large neck circumference
- Hormonal changes during menopause
- Recent significant weight gain
- Use of tobacco and smoking habits
- Genetic predispositions, such as family history
- Structural abnormalities like a recessed chin or prominent overbite
- Congenital conditions like Down syndrome
- Large tonsils or adenoids in children
Recognizing the Symptoms of Sleep Apnea
Detecting sleep apnea early significantly improves treatment outcomes. Recognizable symptoms often overlap between obstructive and central types, making diagnosis challenging. Common signs include:
- Gasping or choking sensations during sleep
- Persistent loud snoring
- Breathing pauses or stops witnessed during sleep
- Morning headaches and dry mouth upon waking
- Excessive daytime sleepiness or fatigue (hypersomnia)
- Difficulty maintaining sleep or insomnia
- Irritability, mood swings, and cognitive difficulties
- Impaired concentration and attention issues
**How Sleep Apnea is Diagnosed**
Clinical evaluation begins with detailed medical history and sleep questionnaires. Healthcare providers may refer patients to sleep centers for comprehensive testing. Diagnostic procedures include:
- Polysomnography (Sleep Study)
This overnight test records multiple body functions, including brain waves, heart activity, oxygen saturation, airflow, respiratory effort, and limb movements. Equipment is attached to monitor real-time physiological changes, offering definitive diagnosis of sleep apnea severity and type. - Home Sleep Testing
Less invasive and more convenient, home sleep tests measure airflow, blood oxygen levels, breathing patterns, and heart rate. While less comprehensive than lab studies, they effectively identify moderate to severe sleep apnea in suitable patients.
**Effective Strategies for Managing Sleep Apnea**
Once diagnosed, treatment approaches depend on severity, individual health factors, and patient preferences. Mild cases can often be managed with lifestyle modifications, whereas moderate to severe cases might require medical devices or surgical intervention.
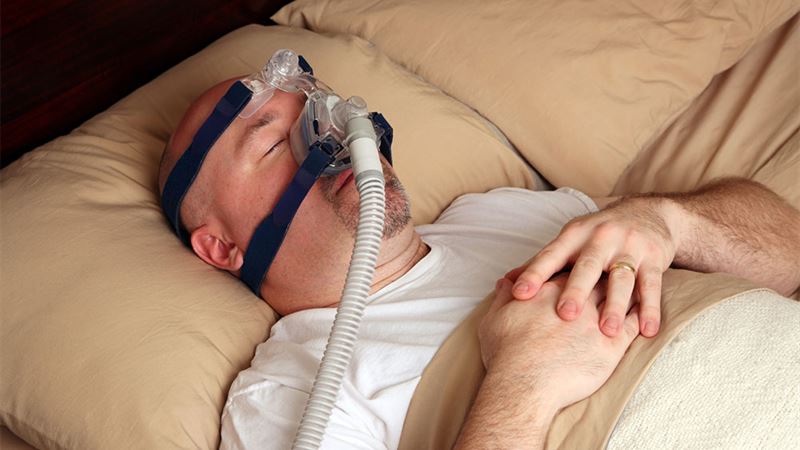
- Utilization of Continuous Positive Airway Pressure (CPAP)
The most common and effective treatment, CPAP involves a machine that delivers pressurized air through a mask, keeping the airway open throughout sleep. It’s particularly beneficial for moderate to severe sleep apnea, effectively reducing snoring and breathing interruptions. Ensuring proper fit and comfort can improve adherence to therapy. - Oral Appliances and Dental Devices
Custom-made dental devices can hold the jaw in a forward position, preventing airway collapse. They are suitable for mild to moderate cases and are favored for their non-invasive nature. - Adaptive Pressure Devices
These advanced machines automatically adjust air pressure based on real-time breathing patterns, providing comfort for users who find traditional CPAP uncomfortable. - Surgical Options
Surgery is generally considered when non-invasive treatments fail. Procedures include tissue removal or reduction (uvulopalatopharyngoplasty), jaw repositioning (maxillomandibular osteotomy), nerve stimulation, and in extreme cases, tracheostomy. Candidate selection is crucial for optimal outcomes.
**Lifestyle Adjustments for Long-Term Management**
Making specific lifestyle changes can significantly reduce sleep apnea severity and improve overall health:
- Weight Management
Losing excess weight is among the most effective strategies, as obesity directly contributes to airway obstruction. Combining a healthy diet with regular exercise can lead to substantial improvements. - Practicing Yoga and Breathing Techniques
Certain yoga routines can boost respiratory strength, improve oxygen intake, and decrease sleep interruptions. Breathing exercises can also enhance airway stability. - Sleeping Position Optimization
Sleeping on one's side or stomach rather than the back can decrease airway collapse and snoring. Consulting with healthcare providers for positional therapy can be beneficial. - Eliminating Alcohol and Smoking
Alcohol relaxes throat muscles and inflames airways, worsening obstructive sleep apnea. Likewise, smoking causes inflammation and swelling, further obstructing airflow. Quitting both habits can markedly reduce symptoms and improve sleep quality.
This article is intended for informational purposes. Always consult with a qualified healthcare professional for diagnosis and treatment of sleep disorders.
