Comprehensive Guide to Spider Vein Removal: Effective Treatments for Achieving Smooth, Clear Skin
Explore comprehensive strategies for treating spider veins, including minimally invasive procedures like sclerotherapy, laser therapy, and advanced treatments such as EVLT and RFA. Learn about causes, symptoms, prevention tips, and how lifestyle changes can reduce the risk, helping you regain smooth, flawless skin. Consult healthcare professionals to determine the best personalized treatment plan for visible superficial veins and enjoy renewed confidence with modern vascular solutions.
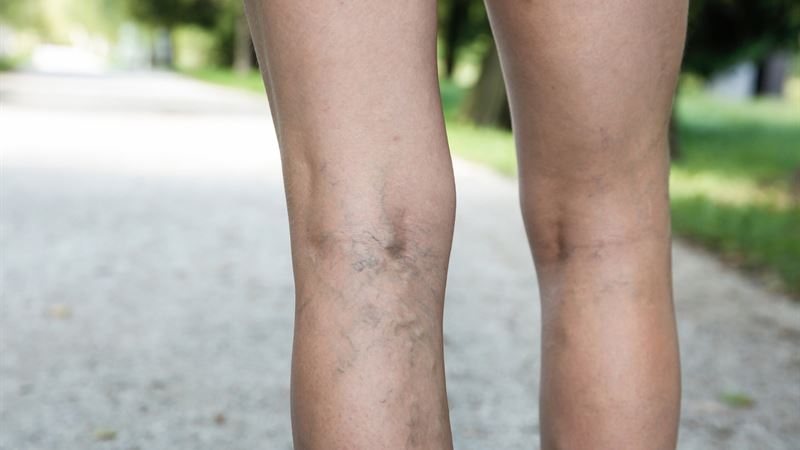
Spider veins, also known as telangiectasias, are small, dilated blood vessels that appear just beneath the surface of the skin, creating a web-like pattern. While they are often harmless, many individuals seek treatment due to cosmetic concerns or discomfort. Understanding the causes, symptoms, diagnostic procedures, and available treatment options can empower you to make informed decisions about managing this common vascular issue. This comprehensive guide explores the various factors contributing to spider veins, their detection, and the most effective therapies to achieve smooth, blemish-free skin.
Age plays a significant role in spider vein development. As we grow older, the walls of our veins and valves tend to weaken, leading to blood pooling and vein dilation. This process makes older adults more prone to developing visible spider veins, especially in the legs and face.
Hormonal fluctuations are another contributing factor. Changes during pregnancy, menopause, or the use of hormonal therapies can alter blood vessel integrity and circulation, thus facilitating the formation of spider veins. Women are generally more affected than men, partly due to hormonal influences.
Prolonged periods of standing or sitting can exert pressure on the veins, impairing efficient blood flow. Occupations that require long durations of standing—such as retail workers or teachers—or extended sitting—like office jobs—can increase the risk of developing spider veins, particularly in the lower limbs.
Obesity adds an additional layer of pressure on veins, especially in the legs, causing the veins to stretch and become more visible. Maintaining a healthy weight can significantly reduce the likelihood of spider vein formation.
Sun exposure is also a key factor, especially for facial spider veins. Ultraviolet (UV) rays damage the skin and underlying blood vessels, weakening vessel walls and leading to visible redness and broken capillaries on the face.
Recognizing Symptoms and Underlying Conditions
Most spider veins are diagnosed based on their appearance—fine, web-like, reddish or bluish veins visible just beneath the skin. Though primarily a cosmetic issue, some individuals experience symptoms such as aching, burning sensations, throbbing, or swelling in affected areas, particularly in the legs. Persistent or worsening symptoms may warrant further examination.
To confirm the diagnosis and rule out other vascular conditions, healthcare professionals often perform a physical examination. In some cases, a Doppler ultrasound is used to assess blood flow within the veins, determine the presence of venous reflux, and evaluate whether more severe conditions like varicose veins are involved.
Modern Treatment Options for Spider Veins
Advances in medical technology have expanded the treatments available for spider veins. Depending on the size, location, severity, and cosmetic concerns, your doctor can recommend the most suitable procedure. Below are some of the most effective and widely utilized treatments.
- Sclerotherapy: This is arguably the most common treatment method for spider veins. It involves injecting a specialized sclerosing solution directly into the targeted veins, causing irritation and subsequent collapse of the vessel walls. Over time, these veins are reabsorbed by the body, leading to a significant improvement in appearance.
- Procedure: The procedure involves using a fine needle to inject the solution under local anesthesia or topical numbing agents. The process is quick, minimally painful, and usually performed on an outpatient basis. Multiple sessions might be necessary depending on the extent of veins needing treatment.
- Pros:
- – Non-invasive with no need for general anesthesia.
- – Fast recovery with minimal downtime.
- – Highly effective for superficial small and medium-sized veins.
- Cons:
- – Multiple sessions may be required to achieve desired results.
- – Potential side effects include swelling, bruising, skin discoloration, or, rarely, blood clots.
- Laser Therapy: Laser treatment is preferred for smaller spider veins, especially on the face. It uses focused light energy to target and heat the vessel, causing it to collapse and be absorbed naturally.
Procedure: A handheld laser device directs pulses of light directly onto the skin surface. The heat generated damages the vein lining without affecting surrounding tissue. Patients often experience a warming sensation or mild discomfort during the procedure.
Pros:
- – Non-invasive, needle-free option.
- – Suitable for facial veins and smaller vascular lesions.
- Cons:
- – Multiple sessions might be necessary for optimal results.
- – Minor side effects such as temporary skin redness or pigmentation changes can occur.
- Endovenous Laser Therapy (EVLT): EVLT is primarily used for larger or deeper veins that cause more noticeable symptoms than superficial spider veins.
Procedure: A small laser fiber is inserted into the affected vein through a tiny incision, emitting laser energy that causes the vein to close off. The body gradually reroutes blood through healthier veins, reducing symptoms and appearance.
Pros:
- – Minimally invasive, outpatient procedure.
- – Effective for larger, problematic veins.
- – Quick recovery, often within a few days.
- Cons:
- – More invasive than surface laser treatments.
- – Possible side effects include mild bruising and swelling.
- Radiofrequency Ablation (RFA): RFA techniques utilize radiofrequency energy to generate heat, causing targeted veins to collapse and close naturally.
Procedure: A catheter is inserted into the vein, where radiofrequency energy is applied to heat and seal the vessel walls. This process effectively prevents blood flow through the treated vein, encouraging rerouting through healthier vessels.
Pros:
- – Highly effective with high success rates.
- – Short recovery times, often performed in outpatient clinics.
- Cons:
- – Potential side effects include temporary numbness, bruising, or skin discolorations.
- – May require local anesthesia.
- Compression Therapy: As a non-invasive management option, compression stockings serve to support blood flow and minimize symptoms without eliminating existing veins.
- Usage: These specially designed elastic stockings exert graduated pressure on the legs, aiding in the movement of blood from superficial to deep veins and reducing vein distension.
- Pros:
- – Easy to use, comfortable, and drug-free.
- – Acts as a preventive measure against new spider veins.
- Cons:
- – Does not remove or treat existing spider veins.
- – Wearing for long periods may be uncomfortable for some individuals.
Preventative Measures and Lifestyle Changes
While some risk factors for spider veins are unavoidable, adopting healthier lifestyle habits can significantly reduce their development and progression. A proactive approach includes:
- Regular Exercise: Engaging in physical activities such as walking, swimming, or cycling improves circulation, strengthens leg muscles, and supports vascular health.
- Maintaining a Healthy Weight: Excess body weight exerts additional pressure on leg veins, increasing the chances of vein dilation and spider vein formation. Achieving and sustaining a healthy weight alleviates this pressure and promotes overall vascular health.
- Leg Elevation: Elevating your legs above heart level when resting or sleeping promotes blood flow back to the heart and reduces venous pressure, preventing the formation or worsening of spider veins.
- Use of Compression Stockings: For those predisposed or in early stages, wearing compression stockings can support blood flow and reduce symptoms.
- Avoid Prolonged Standing or Sitting: Taking regular breaks, stretching, and moving around during long periods of immobility helps maintain healthy blood circulation within the legs.
In conclusion, while spider veins are a common vascular concern mostly deemed cosmetic, they can be effectively treated through various medical procedures. From minimally invasive options like sclerotherapy and laser therapy to more advanced interventions such as EVLT and RFA, there is a suitable treatment for different types of veins and aesthetic goals. Early diagnosis and consultation with a vascular specialist are vital to determine the most effective approach tailored to individual needs. With modern technological advancements and proper lifestyle modifications, achieving clearer, healthier skin with minimal or no visible veins is increasingly accessible, boosting confidence and overall vascular health.
